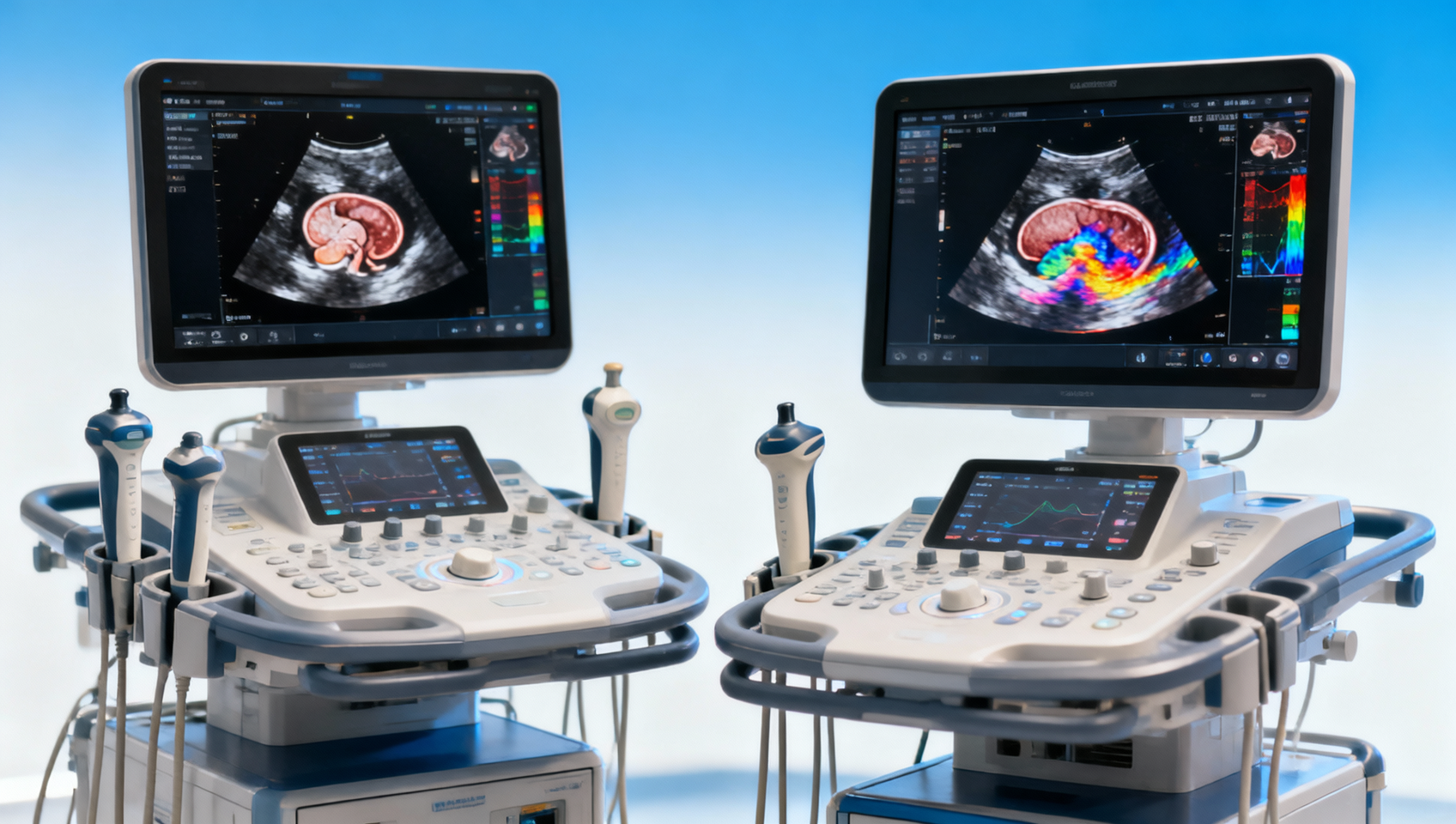
What Makes an Ultrasound Machine Worth the Cost?
For buyers evaluating ultrasound machines, cost is only justified when performance, reliability, imaging quality, and long-term service value align with clinical and business needs. Whether you are comparing systems for routine diagnostics or specialized applications, understanding what truly makes ultrasound machines worth the investment helps reduce risk, improve workflow, and support smarter procurement decisions.
What actually determines ultrasound machine value in a B2B purchase?
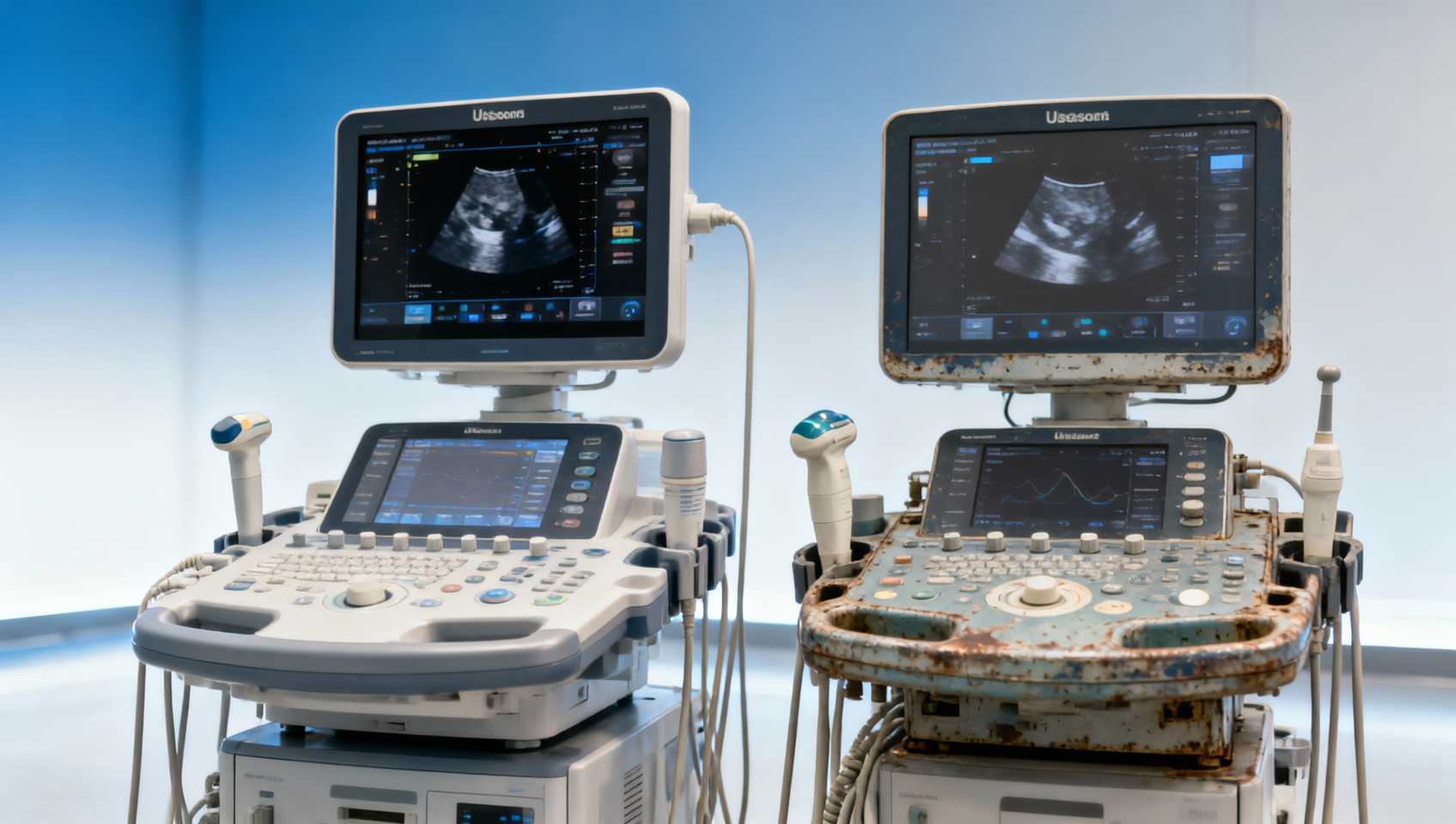
An ultrasound machine is rarely judged by sticker price alone. In hospitals, outpatient centers, imaging chains, and specialized practices, the real question is whether the system can sustain diagnostic quality, support operators with different skill levels, and remain serviceable across a 5–8 year ownership cycle. A lower upfront quote may look attractive, but weak probes, unstable software, or limited service coverage can increase total cost within 12–24 months.
For technical evaluators, value starts with image clarity, penetration, frame rate stability, Doppler performance, and workflow design. For business evaluators and financial approvers, value also includes utilization rate, maintenance burden, training time, expected downtime, and resale or redeployment potential. A machine becomes worth the cost when these factors align with examination volume, specialty requirements, and budget discipline.
This is especially important in healthcare technology procurement, where a machine may serve multiple departments and several user profiles in the same week. One system may need to support abdominal scans in the morning, vascular assessments in the afternoon, and guided procedures later in the day. That makes flexible configuration, probe compatibility, and interface efficiency just as important as raw hardware specifications.
Three value layers buyers should separate
- Clinical value: image detail, diagnostic confidence, reproducibility, and suitability for routine versus advanced scanning.
- Operational value: exam speed, user learning curve, system boot time, reporting integration, and probe switching convenience.
- Commercial value: acquisition cost, service terms, software upgrade path, parts availability, and expected lifecycle planning.
Buyers who do not separate these three layers often overpay for advanced features they rarely use, or underbuy and then face workflow bottlenecks. In practical terms, a system that saves 3–5 minutes per exam across 20–30 scans per day can create stronger return than a premium feature package that remains inactive most of the year.
Which technical features make an ultrasound machine worth the cost?
Technical performance should be reviewed in relation to intended applications, not in isolation. General imaging, cardiology, women’s health, point-of-care, musculoskeletal, and interventional workflows all place different demands on the machine. A procurement team should define 3–5 priority use cases before comparing specifications; otherwise, the review becomes feature-heavy but decision-poor.
Among the most meaningful indicators are transducer range, image processing speed, grayscale uniformity, color Doppler sensitivity, and ergonomic design. Probe frequency ranges often differ by application, such as low-frequency convex probes for deeper abdominal imaging and higher-frequency linear probes for superficial vascular or musculoskeletal work. The machine must support the clinical mix you actually run, not a theoretical feature list.
Operators also feel value through usability. Touchscreen layout, customizable presets, exam templates, and annotation tools can reduce repetitive steps. If a sonographer or clinician needs several extra clicks for each study, time loss compounds quickly. In multi-user environments, consistent user interface design reduces training time from several weeks to a shorter onboarding period, often around 3–10 working days depending on complexity.
For quality and safety managers, reliability matters as much as image output. Stable software, heat management, electrical safety, and robust probe connectors help reduce failures during high-use cycles. In departments running 6–10 hours of daily scanning, even minor instability can disrupt patient scheduling and revenue flow.
Core technical checkpoints before approval
The table below summarizes technical dimensions that commonly influence whether an ultrasound machine is worth the cost for both routine diagnostics and specialty-focused procurement.
A strong specification sheet is useful, but live demonstration remains critical. Decision-makers should request sample scans on at least 2–3 representative case types and compare output under realistic workflow conditions. That is often the fastest way to identify whether a system’s performance justifies its price.
A practical rule for mixed-use departments
If one ultrasound machine will support more than 3 clinical applications, prioritize probe versatility, exam preset management, and upgrade flexibility over niche premium features. That usually creates better long-term value than buying an advanced platform with limited real-world utilization.
How should buyers compare cost, lifecycle, and procurement risk?
The most common procurement mistake is comparing ultrasound machines only by acquisition price. A more reliable method is to compare lifecycle cost over 3–5 years, including warranty coverage, preventive maintenance expectations, software licensing, probe replacement risk, and downtime response. For finance teams, this approach turns a technical purchase into a measurable capital planning decision.
Not all cost drivers are visible in the quotation. Some systems require paid feature activation later. Others bundle core software but charge more for additional probes, service visits, or user training. In high-utilization settings, the replacement cost of a damaged probe can be one of the most important hidden variables, especially if the site relies on a narrow probe inventory.
Project managers should also assess lead time and installation complexity. A typical delivery window can range from 2–8 weeks depending on stock status, configuration, destination market, and import procedures. If deployment is tied to a department launch or budget cycle close, even a technically suitable machine may become a poor choice if support readiness is weak.
Cost comparison framework for ultrasound machine evaluation
The table below can be used by technical teams, procurement managers, and financial approvers to compare whether an ultrasound machine is truly worth the cost beyond its initial purchase value.
This framework helps buyers move from “Which quote is cheaper?” to “Which system will create fewer disruptions and better output over time?” That shift is often what separates a low-cost purchase from a sound capital investment.
Four procurement questions that reduce risk
- Can the machine meet at least 80% of current use cases without immediate add-ons?
- Is local or regional technical support available within a practical service window?
- Are probe options and software upgrades clear at the quotation stage rather than after purchase?
- Does the expected exam volume justify a premium platform, or would a mid-range configuration deliver better return?
What standards, service support, and implementation details matter most?
In medical equipment procurement, value is closely tied to compliance readiness and service execution. Buyers should verify whether the ultrasound machine and its market pathway align with applicable regulatory and electrical safety expectations in the destination country. While exact requirements vary, teams often review documentation related to device registration status, operator safety, labeling, and installation support before approval.
Implementation should be treated as a short project, not a simple shipment. A practical rollout may include 4 stages: requirement confirmation, configuration lock, delivery and installation, then user training and acceptance. Even for standard systems, acceptance should cover image quality checks, probe integrity, connectivity verification, basic workflow setup, and operator signoff. This is particularly useful when one machine will be shared across departments or multiple shifts.
Quality and safety managers should confirm preventive care requirements. For example, they may review cleaning compatibility, storage practices for probes, power conditions, and periodic inspection routines. These factors are not minor details. In many facilities, probe handling and cable stress are among the earliest causes of avoidable service events during the first 12–18 months.
Implementation checklist for cross-functional teams
- Technical team: confirm probe list, imaging modes, connectivity needs, and room power conditions before shipment.
- Procurement team: verify what the quote includes, what is optional, and whether response times are written into service terms.
- Operations team: plan user training for 2–3 shifts if the machine will support broad departmental access.
- Quality team: document acceptance criteria, cleaning instructions, and routine inspection intervals.
Why service support can outweigh a lower unit price
A lower-cost ultrasound machine becomes expensive if support is slow, spare parts are uncertain, or software issues remain unresolved. In contrast, a slightly higher-priced system with better documentation, training, and service coordination may protect uptime and extend usable life. For organizations operating under strict scheduling or reimbursement pressures, that difference is commercially significant.
Common mistakes, buyer FAQs, and when it makes sense to consult specialists
Many teams ask whether a premium ultrasound machine is always worth the cost. The answer depends on workload, clinical complexity, staffing, and expected growth. Overbuying is common when decision-makers assume that the highest specification always delivers the best value. Underbuying is equally common when budget pressure leads teams to ignore service, probe ecosystem, or workflow limitations.
Another frequent issue is evaluating the machine without input from end users. Operators often identify practical concerns faster than anyone else, such as awkward control placement, slow startup, or cumbersome measurement workflows. Technical reviewers may focus on processing power and imaging modes, but end-user friction can determine whether the system performs well in daily practice.
For global B2B buyers, this is where market intelligence becomes useful. TradeNexus Pro helps decision-makers compare supplier positioning, technology direction, delivery readiness, and sourcing signals across healthcare technology markets. Instead of relying on broad marketplace noise, teams can use focused industry analysis to narrow options, identify realistic procurement paths, and prepare more informed internal approvals.
FAQ: how buyers usually frame the decision
How do I know if an ultrasound machine is worth the cost for routine imaging?
Start with exam mix, daily scan volume, and operator profile. If the system handles your 3–5 most common studies efficiently, delivers stable image quality, and fits your service and training model, it is more likely to justify the investment than a feature-rich machine that exceeds your actual workflow needs.
What should financial approvers focus on first?
They should review total ownership logic: initial price, warranty duration, service responsiveness, upgrade costs, and downtime risk. A quote comparison without these elements can misrepresent the true investment profile.
Is a portable or cart-based ultrasound machine the better investment?
Portable systems may suit point-of-care, outreach, or space-limited use. Cart-based systems often provide broader probe support, stronger ergonomics, and better performance for sustained department use. The right choice depends on mobility need, exam duration, and whether the machine serves one clinician or multiple users.
How long does procurement and implementation usually take?
For standard configurations, many projects move through evaluation, quotation alignment, delivery, and installation over several weeks. More complex projects may take longer if they involve specialized probes, import clearance, or multi-site rollout. Planning early helps avoid approval and scheduling pressure.
Why work with TradeNexus Pro
TradeNexus Pro supports buyers who need more than a product listing. Our platform helps procurement leaders, technical evaluators, project owners, and finance stakeholders understand supplier categories, sourcing risks, technology shifts, and commercial positioning across healthcare technology markets. That makes ultrasound machine evaluation more structured and less reactive.
If you are comparing ultrasound machine options, you can use TNP to clarify parameter priorities, shortlist suitable configurations, review likely delivery windows, discuss certification expectations, and prepare internal justification for quotation approval. This is especially useful when your team must balance budget limits, operator needs, and long-term service reliability in one procurement cycle.
Contact TradeNexus Pro to discuss application fit, probe and system selection, implementation planning, service assumptions, supplier screening, and commercial benchmarking. A focused consultation can help you reduce procurement uncertainty before moving to final quotation, sample review, or cross-department approval.
Get weekly intelligence in your inbox.
No noise. No sponsored content. Pure intelligence.