How to compare dental chairs for comfort, hygiene, and daily use?
Choosing among dental chairs is not just about price—it affects patient comfort, hygiene control, operator efficiency, and long-term operating costs. For clinics, distributors, and procurement teams, comparing design ergonomics, cleaning-friendly surfaces, adjustability, and reliability in daily use is essential. This guide explains how to evaluate dental chairs with a practical, decision-focused lens.
What should you compare first when reviewing dental chairs?
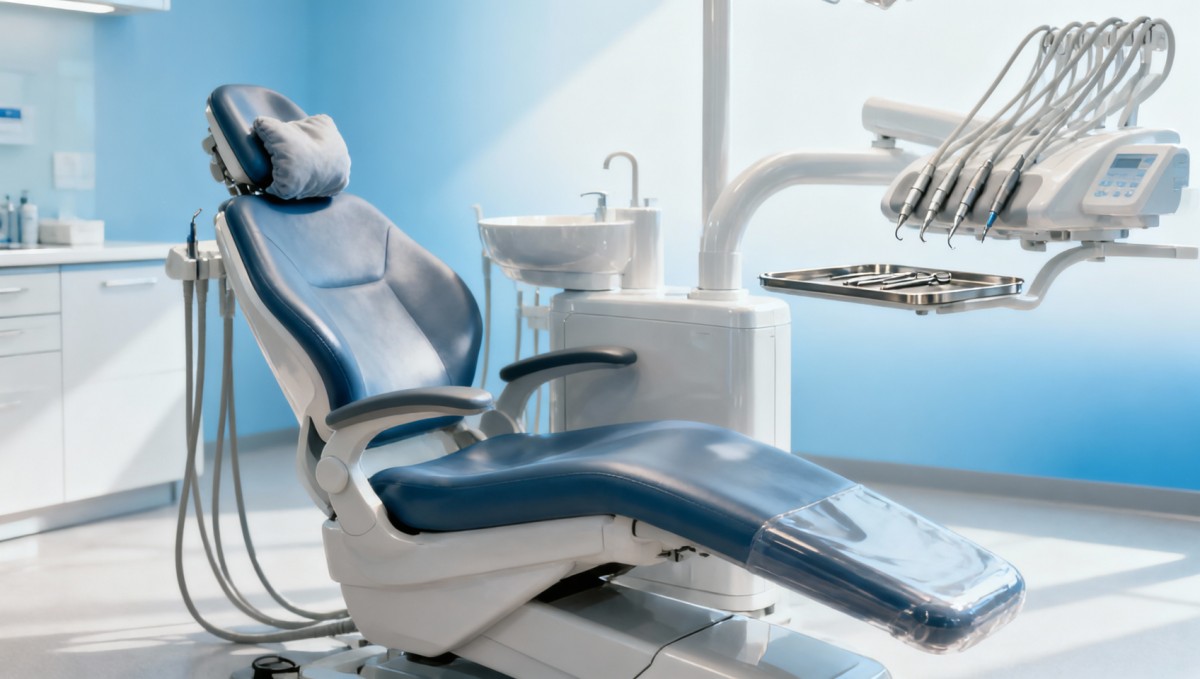
A useful dental chair comparison starts with three primary dimensions: comfort, hygiene, and daily-use durability. Many buyers begin with upholstery color, accessory count, or headline price, but those are secondary. In real clinic operations, the higher-value questions are more practical: Can the chair support patients for 20–90 minute procedures without pressure discomfort? Can staff disinfect high-touch areas between appointments in a short turnover window? Can the system withstand repeated movement across 8–12 hours of daily use?
For operators and assistants, chair ergonomics directly affect posture, reach, and treatment flow. For enterprise decision-makers, the concern is broader: throughput, service intervals, and standardization across multiple treatment rooms. Financial approvers usually want to know whether a lower upfront quote will create higher maintenance costs over 3–5 years. Quality and safety managers focus on cleanability, material integrity, and predictable performance under repeated disinfection cycles.
This is where a structured evaluation framework matters. Instead of asking which dental chair is “best,” procurement teams should ask which chair fits their treatment mix, hygiene protocol, staffing model, and patient profile. A pediatric-heavy clinic, an implant center, and a general dentistry chain will not prioritize the same configuration. Comparing dental chairs without linking them to daily use patterns often leads to overspending on features that bring little operational return.
TradeNexus Pro supports this type of decision-making by helping B2B buyers filter product information through a market intelligence lens. In healthcare technology sourcing, the risk is rarely just choosing the wrong product category. The larger risk is choosing a specification set that mismatches labor flow, compliance expectations, or lifecycle cost targets. A chair that looks competitive on paper may create bottlenecks in cleaning, repairs, or operator positioning once deployed in volume.
The 5 core checkpoints before you compare models
- Patient support geometry: backrest contour, seat width, headrest adjustment range, and entry-exit ease for elderly or limited-mobility patients.
- Operator access: legroom, base shape, working distance, and how easily the chair aligns with common treatment positions.
- Hygiene design: seam reduction, smooth touch surfaces, detachable components, and compatibility with common clinic disinfectants.
- Mechanical reliability: lift stability, articulation smoothness, noise level, and expected service needs under frequent use cycles.
- Procurement fit: delivery lead time, spare parts access, warranty terms, installation support, and training requirements.
If a buying team uses these 5 checkpoints first, shortlisting becomes faster and more objective. It also reduces internal disagreement between clinical users and finance teams because everyone reviews the chair against shared operating criteria instead of isolated preferences.
How do comfort and ergonomics affect daily chair performance?
Comfort in a dental chair is not just a patient satisfaction issue. It affects treatment stability, repositioning time, and operator fatigue. During procedures that last 30–60 minutes, poorly distributed pressure points can cause subtle patient movement. In longer sessions such as endodontic, prosthodontic, or surgical work, even minor discomfort can interrupt workflow. A chair that supports neutral body positioning helps clinicians maintain precision and reduces repeated chair adjustments.
When comparing dental chairs for comfort, assess more than cushion softness. Overly soft padding may feel appealing in a showroom but can compress quickly in routine use. Practical evaluation should include seat density, lumbar support, backrest width, and headrest adaptability for adults of different heights. A useful target is to verify whether the headrest and back support can accommodate at least three common patient groups: smaller adults, average adults, and taller patients, without awkward neck extension.
Operator comfort depends on geometry as much as patient comfort. A bulky chair base can limit stool positioning and knee clearance. Limited access forces clinicians to twist the torso or elevate shoulders during treatment. Over hundreds of procedures per month, that translates into fatigue, slower work, and greater ergonomic strain. For clinics with multiple operators, a chair should allow fast repositioning without complex controls so users can move from consultation to treatment mode in a few seconds.
Project managers and procurement teams should also consider room planning. In compact treatment rooms, chair rotation range, approach angles, and accessory arm placement become critical. A model that fits a 12–15 square meter operatory may not suit tighter layouts if instrument delivery units or assistant modules block movement. Comfort, therefore, should be reviewed as part of the entire workstation system, not as an isolated seat feature.
Comfort comparison factors that matter in real use
The table below helps procurement teams compare dental chairs using measurable comfort and ergonomics criteria rather than showroom impressions alone.
A chair that scores well across these factors usually delivers stronger day-to-day performance than one marketed mainly through cosmetic design. For buyers managing 3–10 treatment rooms, standardizing on ergonomic features can also simplify staff training and reduce adaptation time between operatories.
Practical testing routine before approval
- Run at least 3 position changes: entry, examination, and treatment recline.
- Test with 2–3 user heights to verify headrest and operator reach.
- Observe base clearance using the clinic’s actual stool and assistant movement pattern.
- Simulate a 20-minute treatment setup to identify awkward hand or foot access.
This simple 4-step review often reveals ergonomic issues that specification sheets do not show. For procurement committees, it creates a defensible basis for approval decisions.
Which hygiene features make a dental chair easier to maintain?
Hygiene is one of the most overlooked factors when people compare dental chairs. In daily use, cleaning speed and surface design matter as much as visible aesthetics. High-contact points such as armrests, control interfaces, seams, handles, and delivery-unit touch areas must be easy to wipe thoroughly between patients. If surfaces trap debris or chemical residue, turnaround time increases and infection control becomes harder to standardize.
For quality-control and safety managers, the key question is not whether the chair can be cleaned, but whether it can be cleaned consistently under real scheduling pressure. In many clinics, turnover between patients may be only several minutes. A chair with deep stitching, exposed junctions, porous finishes, or hard-to-remove accessories can slow down protocols and create hygiene weak points. Smooth surfaces, reduced seams, and detachable components support more reliable cleaning routines.
Material compatibility is equally important. Disinfectants used every day can gradually damage lower-grade upholstery or control surfaces. Buyers should ask suppliers which general categories of cleaning agents the chair materials are intended to tolerate and how the finish behaves under repeated wiping. Even without brand-specific claims, this discussion is essential for lifecycle planning. A chair that looks premium at delivery may age poorly after 12–24 months if the surface chemistry does not suit routine disinfectant exposure.
Hygiene also intersects with serviceability. Removable covers, accessible junctions, and fewer unnecessary crevices make periodic deep cleaning easier. For larger clinics or procurement groups, this can save labor hours across many operatories each week. In a B2B evaluation, cleaning efficiency should be treated as a measurable operating factor, not a soft preference.
Hygiene comparison checklist for procurement teams
- Check whether upholstery has minimized seams and whether junctions collect dust, fluids, or polishing compounds.
- Inspect touch surfaces for sharp transitions, exposed fasteners, or difficult-to-wipe contours.
- Ask how many parts can be detached for deeper cleaning and whether removal requires tools.
- Review whether controls are simple to disinfect after each patient and after end-of-day cleaning.
- Confirm maintenance guidance for daily, weekly, and periodic inspection intervals.
These 5 checks help transform hygiene evaluation into a repeatable sourcing process. They are especially useful for multi-site buyers who need consistent cleaning standards across different teams and treatment rooms.
How hygiene design influences cost and compliance
The table below compares common hygiene-related design choices and their likely effect on maintenance effort, cleaning reliability, and daily use suitability.
For financial approvers, this comparison is important because hygiene-friendly design often reduces hidden labor cost. Even a small time saving per turnover becomes meaningful when multiplied by multiple chairs, multiple operators, and a full workweek.
How should buyers compare specifications, reliability, and total cost?
A dental chair should be assessed over its operating life, not just at purchase. That means reviewing mechanical stability, service access, parts availability, and expected maintenance intervals. A low-price chair may appear attractive during budget review, but if it generates more downtime, harder repairs, or frequent upholstery replacement, the total cost of ownership can exceed a mid-tier alternative within a few years.
Procurement teams should separate “must-have” specifications from “nice-to-have” upgrades. Must-haves usually include reliable lift and recline performance, easy hygiene management, ergonomic access, and support coverage. Optional features may include advanced presets, expanded accessory configurations, or design customization. This distinction is critical for project managers working under fixed budgets or phased clinic expansion plans.
Delivery and support timelines also matter. In many healthcare equipment purchases, lead times can vary from several weeks to a few months depending on configuration complexity, regional stock, and installation coordination. Decision-makers should ask not only about shipping, but also about commissioning, user training, and spare part pathways. A chair that arrives quickly but lacks responsive support can slow room activation and affect revenue timing.
TradeNexus Pro is particularly relevant for buyers navigating these variables across cross-border sourcing and multi-supplier comparisons. Instead of reviewing isolated brochures, buyers can evaluate equipment decisions in the broader context of supply chain resilience, category trends, and sourcing risk. This is especially useful for enterprises balancing standardization, cost control, and regional availability across several sites.
A practical dental chair procurement matrix
Use the following matrix to compare shortlisted dental chairs across cost, daily use risk, and procurement suitability.
This type of matrix is useful because it aligns clinical, operational, and financial perspectives in a single view. It is often easier to secure internal approval when cost discussions are linked to downtime exposure, labor impact, and support readiness rather than purchase price alone.
Common sourcing mistakes to avoid
- Comparing dental chairs by price before defining treatment mix and room workflow.
- Ignoring spare parts access, especially for imported equipment in time-sensitive projects.
- Approving a chair based on showroom feel without testing cleaning access and operator posture.
- Overbuying premium features while underestimating maintenance and training needs.
Avoiding these 4 mistakes improves not only equipment selection but also implementation speed and long-term budget control.
Which standards, scenarios, and FAQs should guide the final decision?
Dental chair procurement often involves more than product preference. Buyers may need to align with internal safety procedures, distributor documentation requirements, installation planning, and local regulatory expectations. While specific certification requirements differ by market, procurement teams should still request clear documentation on materials, electrical safety handling, cleaning guidance, and service instructions. Even when a project is time-sensitive, compliance review should not be left until the final approval stage.
Application scenario matters as much as compliance. A high-turnover general clinic may prioritize easy cleaning and fast repositioning. A specialist treatment center may place more weight on patient stability and precise headrest adjustment. A distributor serving multiple clinic types may need a balanced model that covers 70–80% of common use cases rather than a highly specialized configuration. Matching the chair to the operating scenario is often the fastest way to avoid costly misalignment.
Final selection should also include a defined acceptance checklist. Typical review points include delivery condition, movement accuracy, upholstery inspection, accessory completeness, cleaning verification, and user handover. A 6-point acceptance routine is often enough to catch installation issues early while keeping the commissioning process efficient. For multi-room projects, the same checklist should be used across all units for consistency.
Below are several frequently asked questions that procurement teams, clinic operators, and project leaders often raise when comparing dental chairs for comfort, hygiene, and daily use.
How do I choose a dental chair for a busy general clinic?
Focus on three priorities: cleaning speed, operator access, and reliable repositioning. In a clinic with frequent patient turnover, smooth surfaces and simple control geometry usually matter more than advanced cosmetic upgrades. Test whether staff can disinfect key touch areas quickly and whether the chair moves efficiently between consultation and treatment positions. If the clinic runs 8–10 hours a day, daily-use stability is more valuable than rarely used premium features.
What is the biggest mistake in dental chair comparison?
The biggest mistake is evaluating the chair in isolation. A dental chair should be reviewed as part of the full operatory workflow, including stool access, assistant movement, cleaning routine, and support service. A chair can appear comfortable in a demonstration but still cause problems in a compact room or under high-volume scheduling. Compare it in the context of actual use, not showroom conditions only.
How important is upholstery quality in daily use?
It is more important than many buyers expect. Upholstery affects patient comfort, perceived hygiene, and maintenance frequency. Lower-grade material may show wear, cracking, or discoloration sooner under repeated disinfection cycles. Ask practical questions about cleaning compatibility and replacement process. For operators, intact upholstery also improves patient confidence and reinforces a professional treatment environment.
How long should procurement teams plan for selection and deployment?
The timeline depends on sourcing model, site readiness, and configuration complexity, but buyers should separate the process into at least 3 stages: specification review, supplier confirmation, and installation readiness. This helps finance, operations, and project teams coordinate approvals without compressing technical checks. If a clinic opening date is fixed, support lead time and commissioning availability should be confirmed early, not after purchase approval.
Why work with TradeNexus Pro when evaluating dental chair sourcing?
For B2B buyers, the challenge is rarely a lack of product options. The real challenge is filtering those options into a defensible sourcing decision. TradeNexus Pro helps procurement leaders, enterprise decision-makers, financial approvers, and quality managers evaluate healthcare technology purchases with stronger market context. That includes comparing supplier positioning, understanding category shifts, and aligning equipment choices with operational realities rather than surface-level marketing claims.
This is especially valuable when teams must balance comfort, hygiene, lifecycle cost, and implementation timing at the same time. Whether you are sourcing for a single clinic, a regional distributor, or a multi-site healthcare project, structured intelligence reduces guesswork. It also helps internal stakeholders speak the same language when discussing specifications, support, and risk.
If you are comparing dental chairs and need clearer decision support, you can engage with TradeNexus Pro around specific procurement questions. These may include parameter confirmation, model shortlisting, expected delivery windows, configuration trade-offs, supplier communication points, hygiene-oriented design review, documentation expectations, and quotation alignment for different project scales.
Contact TradeNexus Pro if you want a more structured path from product comparison to sourcing action. A focused discussion can help you narrow the right dental chair options for your treatment scenario, budget range, room layout, compliance needs, and deployment schedule—before procurement risk turns into operational cost.
Get weekly intelligence in your inbox.
No noise. No sponsored content. Pure intelligence.



























