TENS Units: When Do They Help and When Don’t They?
TENS units are widely used for pain relief, but their real value depends on the condition, treatment goals, and user profile. For healthcare buyers, operators, and evaluators comparing tens units with broader health-tech tools like electronic health records software, understanding when they work—and when they do not—is essential for safer decisions, better outcomes, and smarter procurement.
In B2B healthcare technology environments, TENS selection is rarely just a clinical choice. It affects patient safety protocols, operator training time, inventory planning, reimbursement alignment, and device lifecycle cost. A unit that performs well in outpatient musculoskeletal care may add little value in post-surgical pathways, neuropathic pain programs, or digitally integrated home-care models.
For procurement teams, technical evaluators, project leaders, distributors, and quality managers, the key question is not whether TENS units can reduce pain in general. The more useful question is where they fit, what limitations they carry, and how to compare them against other pain-management or rehabilitation tools with realistic expectations.
What TENS Units Actually Do in Clinical and Operational Settings
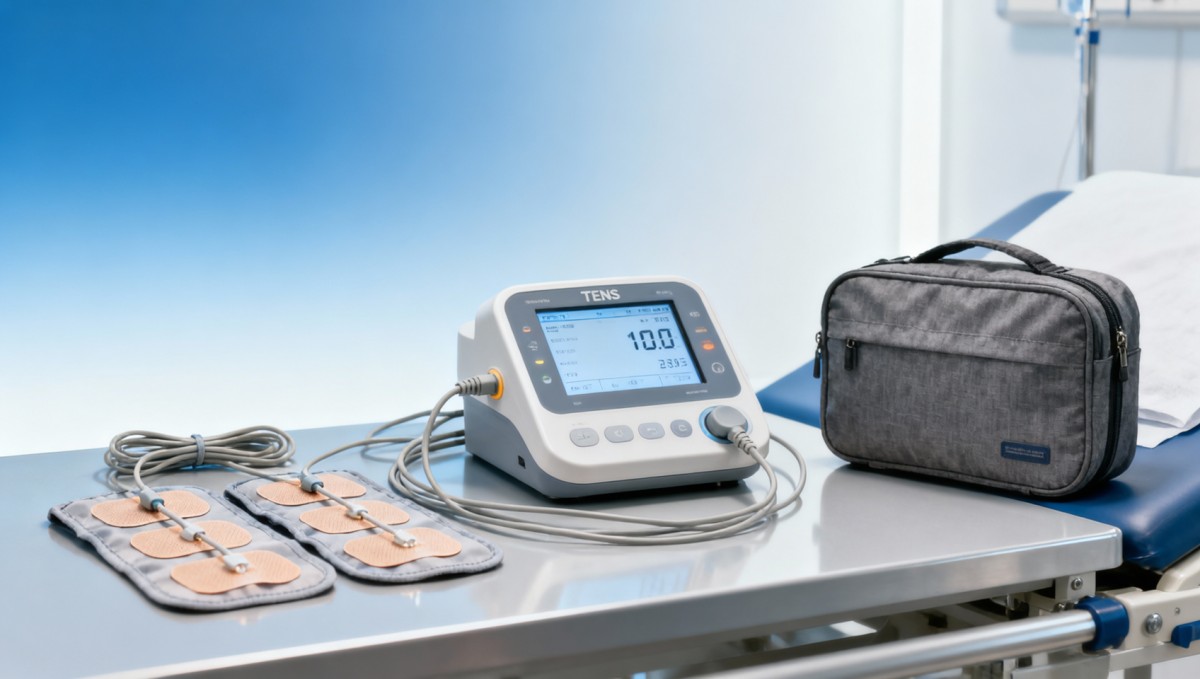
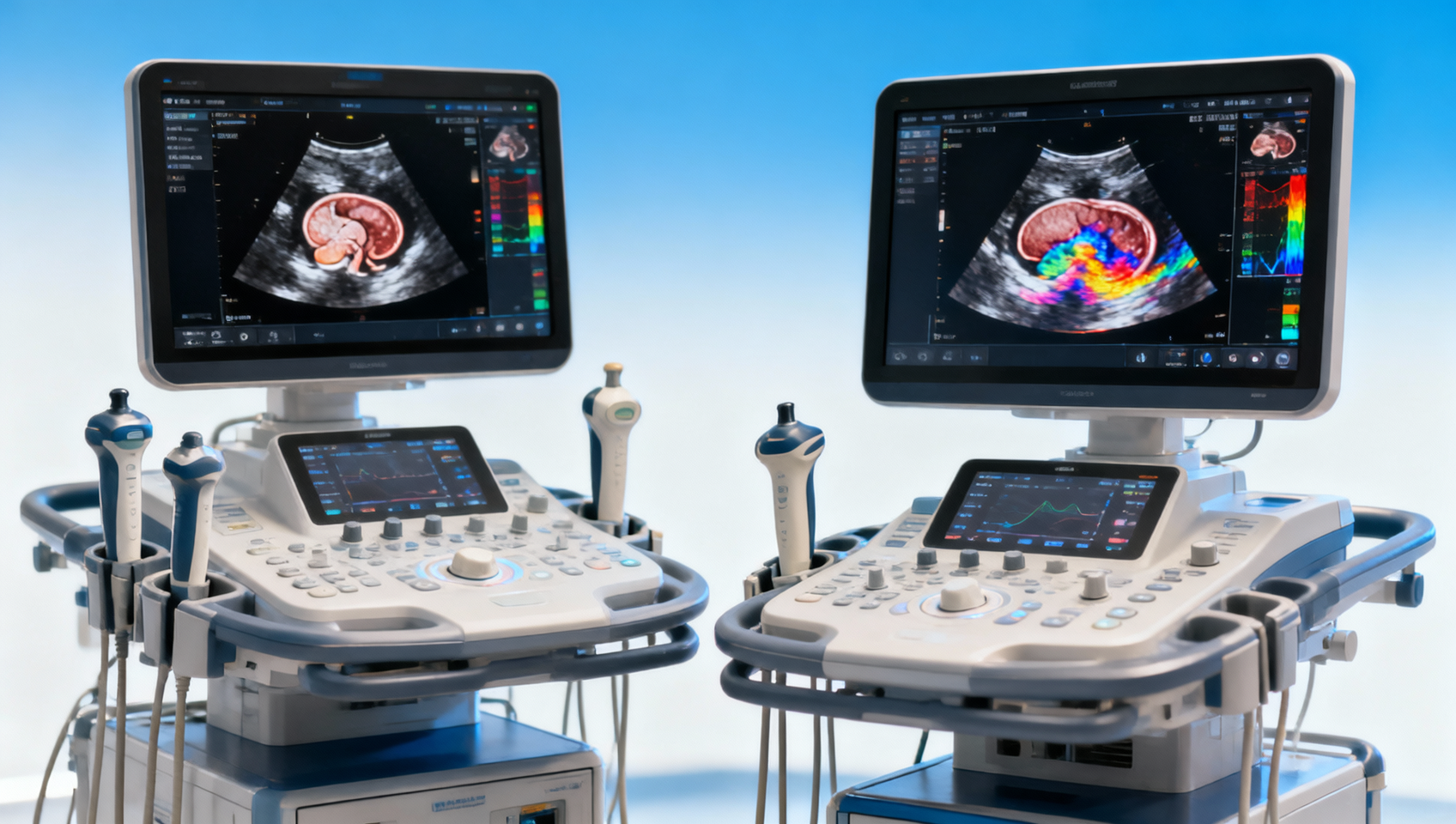
TENS stands for transcutaneous electrical nerve stimulation. These devices deliver low-voltage electrical impulses through electrodes placed on the skin. In practical use, most units allow adjustment of pulse frequency, pulse width, and intensity, often within ranges such as 1–150 Hz for frequency and 50–250 microseconds for pulse width. Those settings influence how the stimulation feels and how tolerable it is for different users.
In outpatient clinics, rehabilitation centers, sports recovery settings, and some home-use programs, TENS is usually positioned as a noninvasive adjunct rather than a stand-alone cure. Sessions often last 15–45 minutes, 1–3 times per day depending on clinical guidance. That operating model matters for decision-makers because utilization rate affects return on procurement and staff workflow planning.
The mechanism is generally discussed in two ways. First, stimulation may help disrupt or modulate pain signal transmission. Second, for some users, it can support short-term comfort that enables movement, stretching, or rehabilitation exercises. That means the value of a TENS unit often depends on whether the organization wants immediate symptom relief, exercise participation support, or a lower-medication complementary pathway.
From a B2B evaluation perspective, TENS units are not equivalent to digital records systems, remote monitoring platforms, or advanced therapeutic devices. They are relatively low-complexity electrotherapy tools. Their strongest business case usually appears when the buyer clearly defines use case, operator profile, and expected frequency of deployment over a 6–24 month device cycle.
Core functional variables buyers should review
Before shortlisting devices, technical and commercial teams should compare several functional basics instead of focusing only on unit price.
- Adjustable intensity range, because underpowered units may limit use in larger muscle groups.
- Preset versus manual programming, which affects training time and user control.
- Number of channels, often 1-channel or 2-channel, which changes treatment flexibility.
- Battery type and operating duration, commonly 5–20 hours between charges depending on mode.
- Electrode compatibility and replacement frequency, often every 15–30 uses under normal care.
The table below summarizes how TENS typically fits into different care and operational goals.
The main takeaway is that TENS is most useful where pain reduction needs are moderate, repeatable, and compatible with self-use or therapist-guided use. It is much less compelling where clinical complexity, severe pathology, or workflow integration demands exceed what a simple electrotherapy device can provide.
When TENS Units Commonly Help
TENS units most often help in cases where pain is persistent but not medically unstable, where the user can communicate sensation clearly, and where treatment goals are realistic. Typical examples include nonacute low back pain, neck tension, osteoarthritis-related discomfort, and some soft-tissue or repetitive-strain complaints. In these scenarios, relief may be partial rather than complete, but even a 20–40 minute reduction in discomfort can improve treatment adherence.
They can also be useful in rehabilitation workflows where pain is blocking participation. A patient who avoids range-of-motion work because of moderate pain may tolerate movement better after a short TENS session. For clinics and therapy operators, that matters because the device becomes a functional enabler, not just a symptom-management tool. This practical distinction improves how value is measured during pilot programs.
Another good fit is structured home use for carefully screened users. In a home program lasting 2–6 weeks, TENS may support repeated symptom control without adding significant staffing burden. For distributors and procurement teams, this makes the device relevant in community care, outpatient follow-up, and certain employer health programs where portability, ease of setup, and low training overhead are priorities.
TENS can also make sense when buyers want a lower-risk adjunct before escalating to more resource-intensive interventions. It is not a substitute for diagnosis, rehabilitation planning, or records management, but within a multi-tool care pathway it can occupy a sensible low-cost tier.
Application scenarios with the strongest practical fit
1. Repetitive outpatient therapy
When a facility delivers high volumes of musculoskeletal care, even a simple device can create value if used across 10–30 patients per week. In these settings, standardized electrode placement charts and treatment presets reduce operator variability.
2. Guided home-care continuity
If the patient population is stable and trainable, home-use TENS may support continuity between clinic visits spaced 7–14 days apart. This is especially useful where travel burden or appointment capacity limits in-person care.
3. Conservative pain-support pathways
Organizations that want nonpharmacological adjuncts often place TENS alongside exercise, manual therapy, education, and ergonomic adjustment. Its contribution is strongest when bundled rather than marketed as an all-in-one answer.
The following comparison helps buyers match TENS use cases to expected outcomes.
For buyers, the table highlights a recurring pattern: TENS performs best where expectations are narrow, treatment pathways are stable, and users can actively report comfort and response. That is why pilot testing in one service line before enterprise-wide rollout is usually a better strategy than broad immediate deployment.
When TENS Units Do Not Help Enough—or Should Be Avoided
TENS units do not help much when pain is caused by a condition that requires urgent medical intervention, structural correction, or more advanced clinical management. For example, they should not be treated as a primary response to unresolved fracture pain, unexplained chest pain, severe neurological compromise, or rapidly worsening symptoms. In those cases, delaying escalation can create safety and liability issues.
Even in nonemergency situations, benefit may be limited if the user cannot tolerate stimulation, cannot communicate intensity accurately, or expects a durable effect after only one or two sessions. Some users experience little response after 3–5 properly conducted treatments. For B2B programs, this means outcome variability should be built into purchasing assumptions rather than ignored.
TENS may also be a poor fit where workflow complexity is high. In acute care settings with multiple monitoring devices, mobility restrictions, wound concerns, or short nursing windows, adding electrode placement and stimulation setup may offer low operational payoff. Likewise, if a health system’s current priority is data integration, care coordination, or remote documentation, investment in TENS may rank below software or connected-device infrastructure.
Quality and safety teams should also screen for standard contraindication zones and risk factors. While detailed clinical policies vary, common caution areas include users with implanted electrical devices, placement near certain sensitive anatomical areas, compromised skin, or settings where unsupervised use could lead to misuse. Procurement without protocol alignment increases avoidable risk.
Common reasons B2B buyers overestimate TENS value
- They treat pain relief as a uniform category and ignore differences between acute, chronic, neuropathic, and functional pain patterns.
- They assume a device with 10 or more preset modes automatically improves outcomes, even when operators use only 2 or 3 settings.
- They compare TENS to system-level digital tools such as electronic health records software, even though the value metrics are entirely different.
- They underestimate consumable management, including electrode replacement, battery charging, cleaning, and user instruction time.
Risk points for safety and compliance teams
A practical risk review should cover at least 4 items: user screening, electrode placement guidance, cleaning protocol, and documentation of adverse discomfort or nonresponse. If any of those steps are missing, the device may create more operational burden than clinical benefit.
The central lesson is that a TENS unit is not ineffective by default, but it becomes ineffective in the wrong context. The more complex the pain pathway and the more variable the user population, the more important it is to compare TENS against alternative investments such as rehabilitation devices, digital therapy support, or workflow software.
How to Evaluate TENS Units for Procurement, Distribution, and Technical Review
A sound procurement process starts with use-case mapping. Buyers should define whether the units are for clinic treatment rooms, home distribution, sports recovery services, occupational health programs, or reseller channels. That decision shapes preferred device format, packaging, language support, training materials, and after-sales expectations. A product suitable for 50 home users per quarter is not necessarily suitable for a busy rehab department with daily multi-operator use.
The next step is technical screening. Instead of collecting long feature lists, evaluators should review 5 core dimensions: output adjustability, ease of controls, electrode ecosystem, power management, and durability. In many real environments, simpler interfaces reduce errors more effectively than feature-heavy menus. A device that new staff can learn in 20 minutes may outperform a more advanced unit that requires repeated configuration support.
Commercial review should include total operating cost, not just landed unit price. Consumables, replacement pads, warranty terms, expected service life, and training burden can materially change cost per use over 12 months. For distributors and financial approvers, one of the most overlooked variables is reorder behavior: low-cost devices with hard-to-source accessories often create avoidable channel friction.
Implementation teams should also ask whether the organization needs integration at all. Most standard TENS units are not deeply connected devices. If the broader project objective is care-pathway visibility, usage documentation, or enterprise reporting, then a simple standalone electrotherapy unit may need to be complemented by software tools rather than evaluated in isolation.
A practical procurement checklist
The table below provides a decision framework that technical and business teams can adapt during supplier comparison.
This framework helps separate meaningful performance indicators from marketing noise. In many tenders, the strongest supplier is not the one with the most modes, but the one with stable accessory supply, clear instructions, and predictable service performance over 12–24 months.
Recommended review process in 5 steps
- Define target user groups and treatment environments.
- Set minimum technical thresholds for settings and safety documentation.
- Run a pilot with a limited sample, such as 10–20 users or one department.
- Track usability, nonresponse rate, consumable turnover, and training time for 2–4 weeks.
- Decide whether TENS should scale, remain niche, or be replaced by another solution type.
Implementation, Training, and FAQ for Real-World Adoption
Successful TENS deployment depends less on the hardware alone and more on how the organization structures use. A clear implementation package should include screening criteria, treatment-duration guidance, electrode placement charts, cleaning instructions, and escalation rules for nonresponse. Without those basics, a device that is technically adequate can still fail in practice.
Training should be role-specific. Operators may need 30–60 minutes of hands-on instruction, while distributors may need commercial positioning guidance and quality managers may focus on storage, inspection, and complaint handling. If the buyer expects home use, patient-facing materials should be simplified into short steps with visual cues and frequency limits.
Maintenance is usually straightforward, but it should not be ignored. Electrode care, cable inspection, battery charging cycles, and periodic performance checks are basic quality controls. A practical inspection rhythm might be weekly for high-use clinic devices and monthly for lower-volume settings, with accessory stock review every 30–90 days.
For enterprise decision-makers, the smartest position is often balanced adoption. TENS units can be useful, affordable, and operationally light in the right lane. They simply should not displace investments that solve larger clinical documentation, workflow, or coordination gaps.
FAQ
How long does it usually take to evaluate a TENS program?
A basic pilot can often be completed in 2–4 weeks if the organization already has a defined user group. A broader evaluation involving multiple departments may take 6–8 weeks to account for training, accessory use, and comparative feedback.
Which buyers get the most value from TENS units?
Outpatient rehabilitation providers, occupational health programs, community care teams, and distributors serving conservative pain-support channels often see the clearest value. High-acuity hospitals and digitally transformation-focused health systems may prioritize other tools first.
What are the most common purchasing mistakes?
The top 3 mistakes are buying without a clear use case, ignoring consumable logistics, and expecting TENS to solve severe or complex pain on its own. Another common issue is selecting advanced settings that operators rarely use.
How should buyers compare TENS with digital health tools?
They should compare by function, not by category label. TENS addresses a narrow therapeutic need. Tools such as electronic health records software address documentation, care coordination, reporting, and interoperability. In many organizations, the right question is how both fit within the same care pathway rather than which one is “better.”
TENS units help most when pain is moderate, the treatment objective is specific, and the user can follow a structured protocol. They help far less when clinical complexity is high, diagnosis is unclear, or the organization expects broad system-level impact from a simple device. For B2B healthcare buyers, the most reliable approach is to evaluate TENS within the full operational context: patient profile, training burden, accessory supply, and competing technology priorities.
If your team is assessing TENS units alongside broader healthcare technology investments, TradeNexus Pro can help you compare solution fit, procurement variables, and implementation risk across product categories. Contact us to discuss your sourcing criteria, request a tailored evaluation framework, or explore more healthcare technology solutions aligned with your market and operational goals.
Get weekly intelligence in your inbox.
No noise. No sponsored content. Pure intelligence.