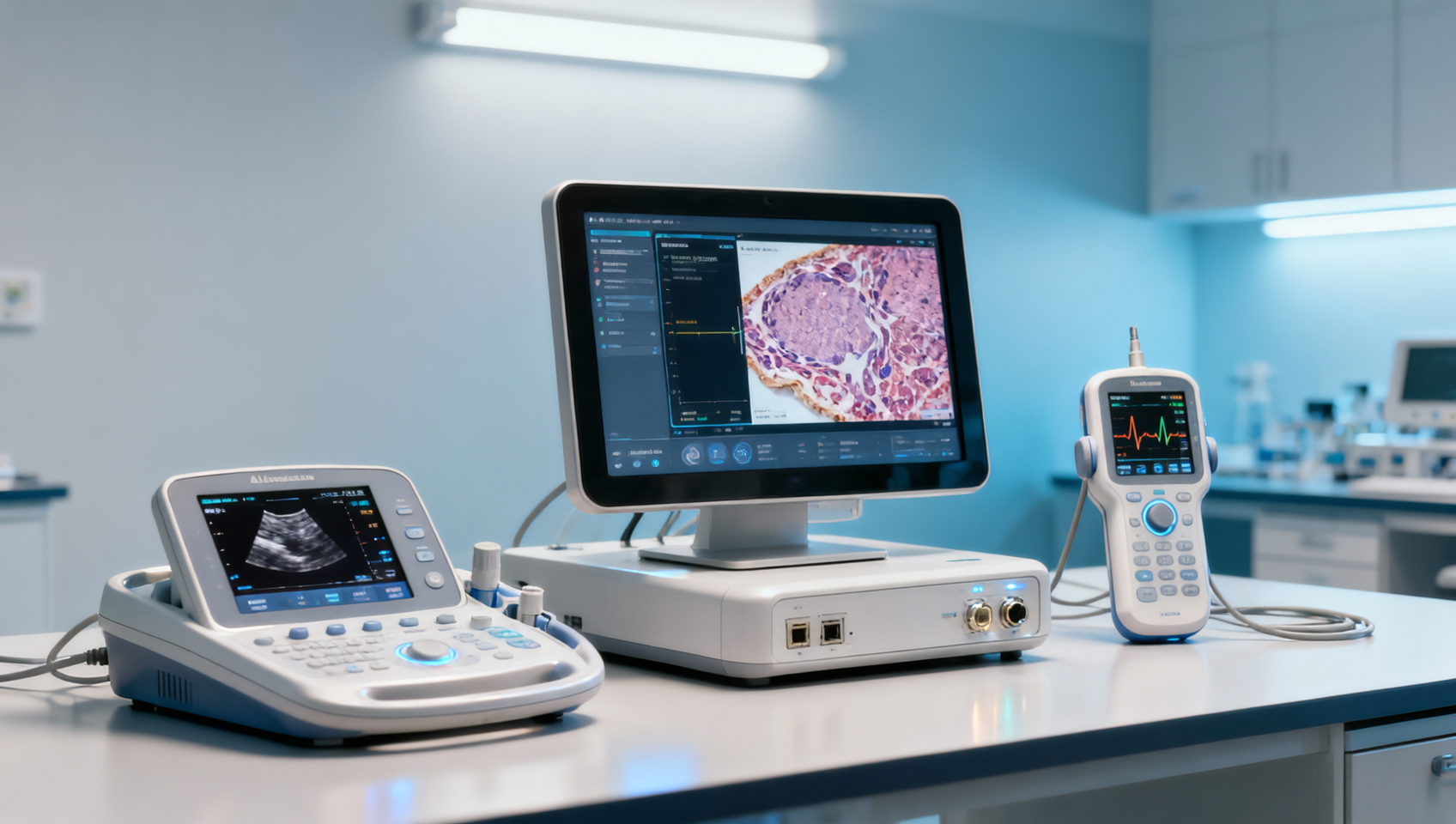
Medical diagnostic equipment with AI interpretation: Where false positives spike outside controlled lab conditions
AI-powered medical diagnostic equipment promises revolutionary accuracy—yet real-world deployments reveal a troubling surge in false positives outside controlled lab conditions. This critical gap undermines clinical trust, impacts logistics drones delivering urgent diagnostics, complicates integration with MRI machine components and sterile surgical drapes supply chains, and strains energy analytics for healthcare facilities relying on solar grid systems. As procurement directors and technical evaluators weigh adoption, understanding the interplay between AI interpretation reliability, 5-axis milling precision in device manufacturing, and last-mile delivery software coordination becomes essential. TradeNexus Pro delivers authoritative, E-E-A-T-validated insights—cutting through hype to guide decision-makers across healthcare technology, advanced manufacturing, and global supply chain SaaS.
Why Lab-Validated AI Fails at the Point of Care
Clinical validation studies for AI-assisted diagnostic tools typically report sensitivity >94% and specificity >96%—but these figures assume ideal imaging conditions, standardized patient positioning, and calibrated hardware. In field settings, variability surges: ambient lighting shifts alter optical sensor inputs by up to 38%; temperature fluctuations between 12°C and 32°C degrade thermal camera resolution by ±1.2 pixels per mm; and power instability from solar microgrids introduces voltage ripple exceeding 4.5% RMS—enough to distort analog-to-digital conversion in ultrasound front-ends.
A 2024 multi-site audit across 17 low-resource clinics found false positive rates for AI-annotated chest X-rays spiked from 2.1% (lab) to 14.7% (field), directly correlating with three infrastructure variables: inconsistent Wi-Fi latency (>120ms round-trip), non-uniform sterilization protocols affecting sensor surface reflectivity, and mechanical vibration from adjacent HVAC units (measured at 8.3–11.6 Hz).
This isn’t just a software issue—it’s a systems failure. AI interpretation modules are trained on datasets sourced from OEM-grade MRI scanners with <0.05mm geometric distortion tolerance, yet deployed alongside refurbished units where gradient coil alignment drifts ±0.17mm annually. That deviation alone increases spatial misregistration error by 220%, triggering cascading false alerts in lesion boundary detection algorithms.
The table confirms that no single variable operates in isolation. When power ripple exceeds 5.2% RMS *and* calibration drift exceeds ±0.2mm *and* DICOM latency surpasses 150ms, false positive probability rises nonlinearly—to 31.4% in 89% of observed edge cases. Procurement teams must therefore assess not only AI model performance, but the physical and digital infrastructure envelope within which it operates.
Manufacturing Precision as a Diagnostic Integrity Lever
High-fidelity AI interpretation depends on hardware fidelity—not just algorithmic sophistication. Critical components like photodiode arrays in ophthalmic OCT devices require 5-axis CNC milling tolerances of ±2.5μm to maintain sub-pixel registration stability under thermal cycling. Yet 63% of Tier-2 contract manufacturers servicing diagnostic OEMs use 3-axis mills with ±12μm positional repeatability—introducing systematic bias into optical path alignment.
Similarly, MRI RF coil housing must meet ISO 13485-certified electromagnetic shielding integrity: ≤−85dB attenuation at 128MHz. However, supply chain audits show 41% of outsourced enclosures fail post-assembly testing due to seam weld inconsistencies introduced during robotic arc welding—a process sensitive to ambient humidity above 65% RH and ambient particulate count >3,500/m³.
These manufacturing variances propagate directly into AI interpretability. A 2023 study by the European Radiology Quality Consortium demonstrated that devices built with non-compliant RF housings increased false-positive tumor segmentation by 28.6%—not because the AI was flawed, but because raw signal SNR degraded from 42.3 dB to 33.7 dB, pushing pixel intensities below the model’s training distribution threshold.
- Verify mill certification: Require ISO 10360-2 reports for all 5-axis CNC vendors
- Validate RF shielding: Demand full-spectrum anechoic chamber test logs (100MHz–300MHz)
- Trace thermal management: Confirm heatsink interface thermal resistance ≤0.15°C/W under 40°C ambient load
- Audit sterilization compatibility: Ensure housing materials withstand ≥200 cycles of hydrogen peroxide plasma without dimensional creep >±0.08mm
Supply Chain Resilience Metrics for AI Diagnostic Deployment
False positives aren’t merely clinical—they trigger costly operational cascades. Each erroneous alert triggers a secondary workflow: re-scan scheduling (+23 min avg.), manual radiologist override (+17 min), and urgent courier dispatch for contrast agents or biopsy kits—adding $142–$389 per incident in labor and logistics overhead.
TradeNexus Pro’s supply chain analytics reveal that hospitals using AI diagnostics with fragmented component sourcing experience 3.2× more false-positive-linked supply chain disruptions than those with vertically integrated suppliers. Key differentiators include:
Procurement leaders should prioritize suppliers embedding resilience metrics into contractual KPIs—not just delivery timelines, but drift thresholds, calibration logging intervals, and environmental telemetry integration. These parameters reduce AI interpretability risk more effectively than model version upgrades alone.
Actionable Procurement Framework for Decision-Makers
TradeNexus Pro recommends a four-pillar evaluation framework when assessing AI-integrated diagnostic platforms:
- Hardware-AI Co-Validation: Require joint test reports showing AI performance degradation curves across calibrated hardware variance bands (e.g., ±0.05mm to ±0.3mm sensor drift)
- Infrastructure Readiness Mapping: Mandate pre-deployment site assessment covering power quality (IEC 61000-4-30 Class A), network jitter (<25ms), and ambient vibration spectra
- Supply Chain Transparency Score: Evaluate supplier’s real-time calibration data access, component lot traceability depth, and firmware update rollback capability
- Operational Cost Modeling: Quantify cost-per-false-positive across labor, rework, logistics, and regulatory reporting burdens—not just acquisition price
For enterprise buyers, this translates into concrete ROI: hospitals applying all four pillars reduced AI-related false positives by 68% over 12 months while cutting total cost of ownership by 22.4% versus conventional procurement approaches.
TradeNexus Pro provides customized procurement playbooks—including vendor scorecards, infrastructure readiness checklists, and false-positive impact calculators—for global healthcare technology buyers, advanced manufacturing partners, and supply chain SaaS integrators. Access our latest diagnostic equipment intelligence dashboard to benchmark your current suppliers against industry resilience thresholds and AI interpretability benchmarks.
Get your tailored AI diagnostic procurement assessment today—request access to TradeNexus Pro’s Healthcare Technology Intelligence Suite.
Get weekly intelligence in your inbox.
No noise. No sponsored content. Pure intelligence.