When Should You Replace Emergency Medical Kits at Work?
When should emergency medical kits at work be replaced?
Emergency medical kits are only effective when they are complete, compliant, and immediately usable during a workplace incident.
Knowing when to replace emergency medical kits helps reduce response delays, supports compliance, and protects staff across offices, warehouses, factories, laboratories, and field operations.
Replacement is not based on one date alone. It depends on expiration, usage, contamination, packaging damage, regulation changes, and workplace risk levels.
A clear review process keeps emergency medical kits reliable and prevents hidden failures during emergencies, audits, and daily safety inspections.
Why a structured review process matters
Many workplaces check supplies only after an injury happens. That approach increases risk because missing items are usually discovered when response time matters most.
A structured review process turns emergency medical kits into controlled safety assets instead of neglected storage boxes.
It also supports documentation, restocking discipline, and better alignment with OSHA guidance, ISO-based safety systems, and internal EHS procedures.
For multi-site operations, a checklist-based method creates consistency, simplifies training, and makes replacement decisions faster and easier to defend.
Core signs that emergency medical kits need replacement
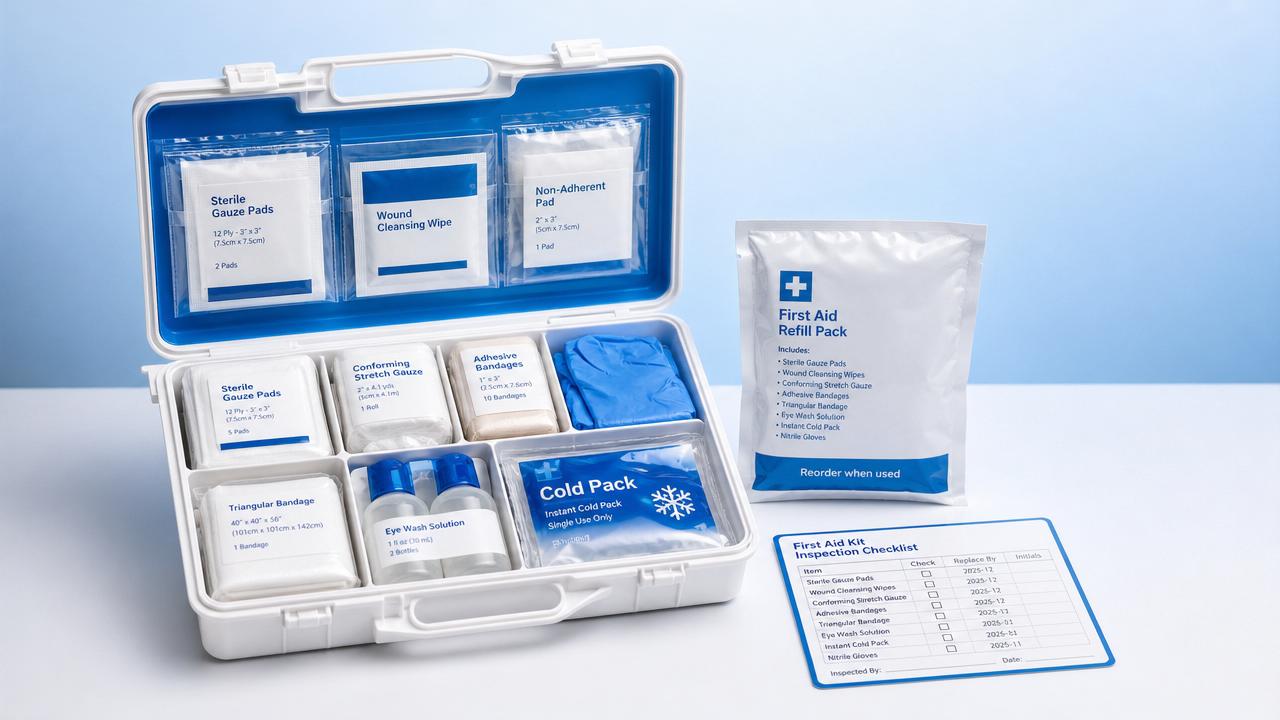
Use the following points to decide whether emergency medical kits need partial replenishment or full replacement.
- Replace any item past its expiration date, especially antiseptics, burn dressings, eye wash, medications, and sterile products with manufacturer time limits.
- Replace the full kit if moisture, dust, chemicals, or pests entered the case and may have compromised sterile contents or packaging integrity.
- Replace supplies immediately after use when quantities fall below minimum levels needed for the site’s injury profile and workforce size.
- Replace damaged kits if latches fail, seals break, hinges crack, or labels become unreadable and delay emergency identification or access.
- Replace outdated contents when regulations, internal protocols, or certified first-aid standards change and the current kit no longer matches requirements.
- Replace emergency medical kits sooner in high-traffic areas where frequent handling increases loss, contamination, and unnoticed depletion between inspections.
- Replace contents after extreme heat or freezing exposure because temperature swings can weaken adhesives, solutions, wraps, and sealed sterile barriers.
- Replace kits lacking a current inventory sheet because missing documentation often hides expired items, incomplete sets, and inconsistent restocking practices.
How often should emergency medical kits be inspected?
Inspection frequency should match the environment, hazard level, and usage rate.
For most workplaces, a monthly review is a practical baseline. High-risk sites often need weekly checks, while remote vehicles may need pre-shift verification.
A simple schedule can include:
- Visual check every week for seal condition, storage damage, and accessibility.
- Full inventory review every month for count, expiry, and packaging integrity.
- Immediate post-incident review after any item is used.
- Quarterly compliance review against current workplace safety requirements.
Emergency medical kits should also be reviewed after site moves, renovations, process changes, or staffing increases that alter exposure risks.
Replacement timelines by item type
Different items within emergency medical kits age at different rates. A single annual replacement date is often too simplistic.
If several categories are affected at once, replacing the entire kit may be faster, cleaner, and more auditable than piecemeal replenishment.
Workplace scenarios that change replacement needs
Office environments
Office emergency medical kits usually experience lower usage, but neglect is common because incidents seem less severe.
Focus on expiration control, easy visibility, and replacement after minor but frequent use of bandages, wipes, and gloves.
Manufacturing and warehouse sites
These settings often face cuts, crush risks, burns, and dust exposure. Emergency medical kits here need more frequent checks and stronger case durability.
Replace kits faster when cabinets become dirty, contents shift, or trauma-oriented items are repeatedly used or removed without reporting.
Laboratories and healthcare-adjacent facilities
Sterility, splash protection, and chemical compatibility matter more in these environments.
Replace emergency medical kits immediately after contamination concerns, liquid exposure, or protocol updates related to biohazard handling.
Vehicles, field service, and remote operations
Mobile emergency medical kits degrade faster because of vibration, heat, freezing, and irregular inspections.
Use shorter replacement cycles and assign responsibility before each trip or shift begins.
Commonly overlooked risks
One common mistake is replacing only expired items while ignoring the kit container. A broken case can delay access just as much as missing supplies.
Another overlooked issue is undocumented usage. Small removals accumulate, leaving emergency medical kits incomplete long before the next formal review.
Temperature exposure is also underestimated. Supplies stored near loading docks, vehicles, rooftops, or machinery can degrade well before printed expiry dates.
Outdated layouts create risk too. If workers cannot quickly find trauma pads, eye wash, or gloves, the kit is functionally deficient.
Finally, many sites treat all emergency medical kits the same, even when hazards differ sharply by department, floor, or job task.
Practical steps to improve replacement decisions
- Create a master inventory list for every kit location, including item counts, expiry dates, and approved replacements.
- Use tamper seals or inspection tags so missing reviews become obvious during internal audits.
- Assign one accountable owner per kit, even when several people may access the contents.
- Standardize replacement thresholds for low stock, damaged packaging, and environmental exposure.
- Review incident records to identify which emergency medical kits need upgraded contents or larger quantities.
Digital logs can simplify this process, especially for multi-site operations where consistency and proof of maintenance are essential.
FAQ about replacing emergency medical kits
Can emergency medical kits be used past expiration dates?
They should not be relied on past expiration dates, especially sterile or liquid items. Replace them before they become noncompliant or unreliable.
Should you replace the whole kit or only used items?
If only one or two items were used, replenishment may be enough. If several items are expired, damaged, or contaminated, replace the full kit.
Are emergency medical kits legally required to follow one universal standard?
Requirements vary by country, site risk, and industry guidance. The safest approach is to align kit contents with actual hazards and current regulations.
Final action points
Emergency medical kits should be replaced whenever expiration, damage, contamination, stock loss, or compliance changes reduce readiness.
The best replacement program combines scheduled inspections, clear ownership, environment-specific standards, and fast post-use replenishment.
For organizations building resilient safety systems, emergency medical kits deserve the same disciplined oversight as any other critical operational safeguard.
Start with a site-wide audit, document gaps, and set replacement rules that match real workplace risks rather than generic assumptions.
Get weekly intelligence in your inbox.
No noise. No sponsored content. Pure intelligence.