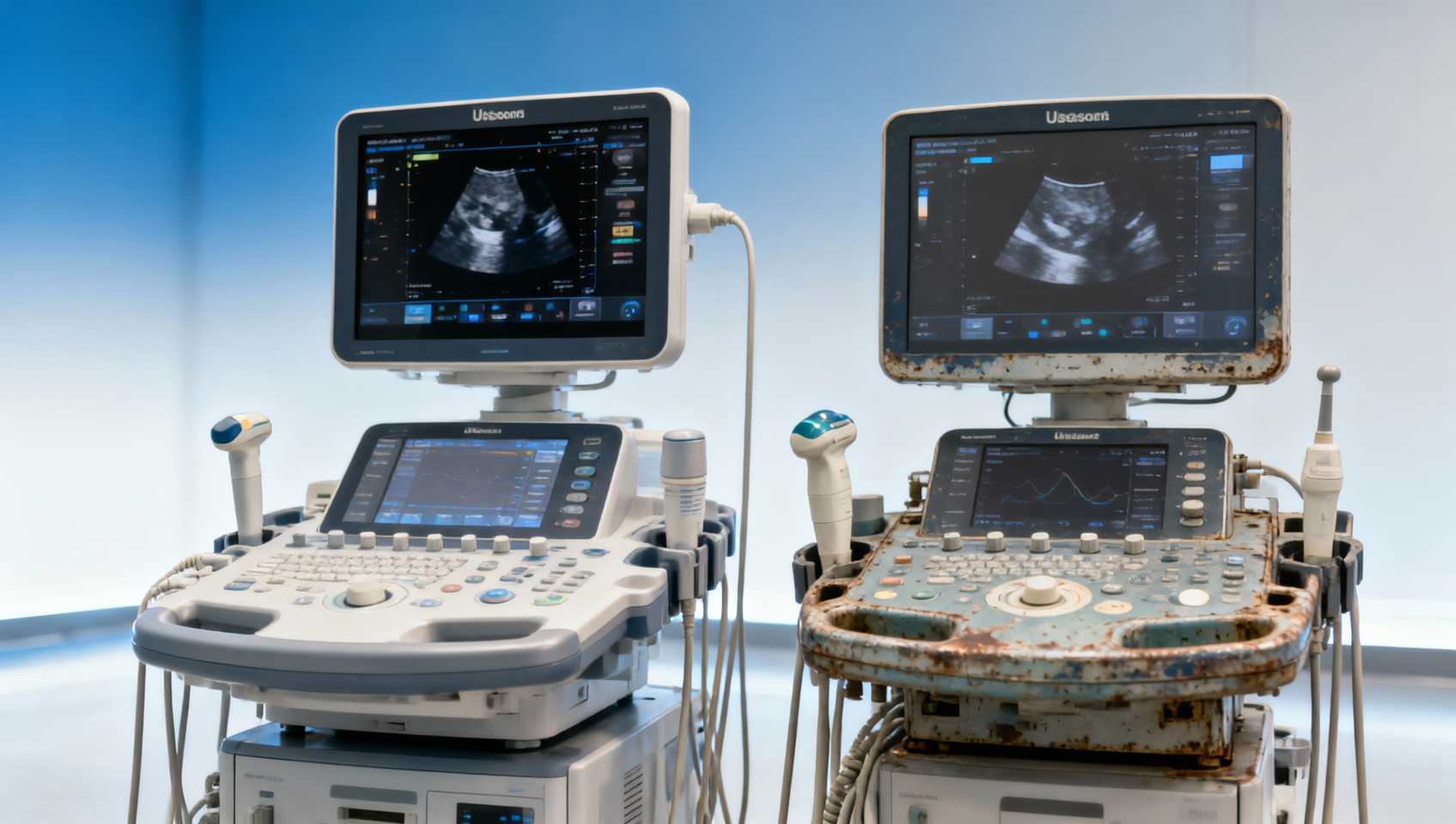
Ultrasound Machines: New vs Refurbished in 2026
In 2026, choosing between new and refurbished ultrasound machines is no longer just a budget decision—it is a strategic move that affects clinical performance, compliance, lifecycle cost, and procurement efficiency. For buyers comparing healthcare technology investments alongside priorities such as energy efficiency and supply chain resilience, understanding the real value, risk, and sourcing logic behind ultrasound machines is essential before making a final purchase.
Why the new vs refurbished ultrasound machine decision matters more in 2026
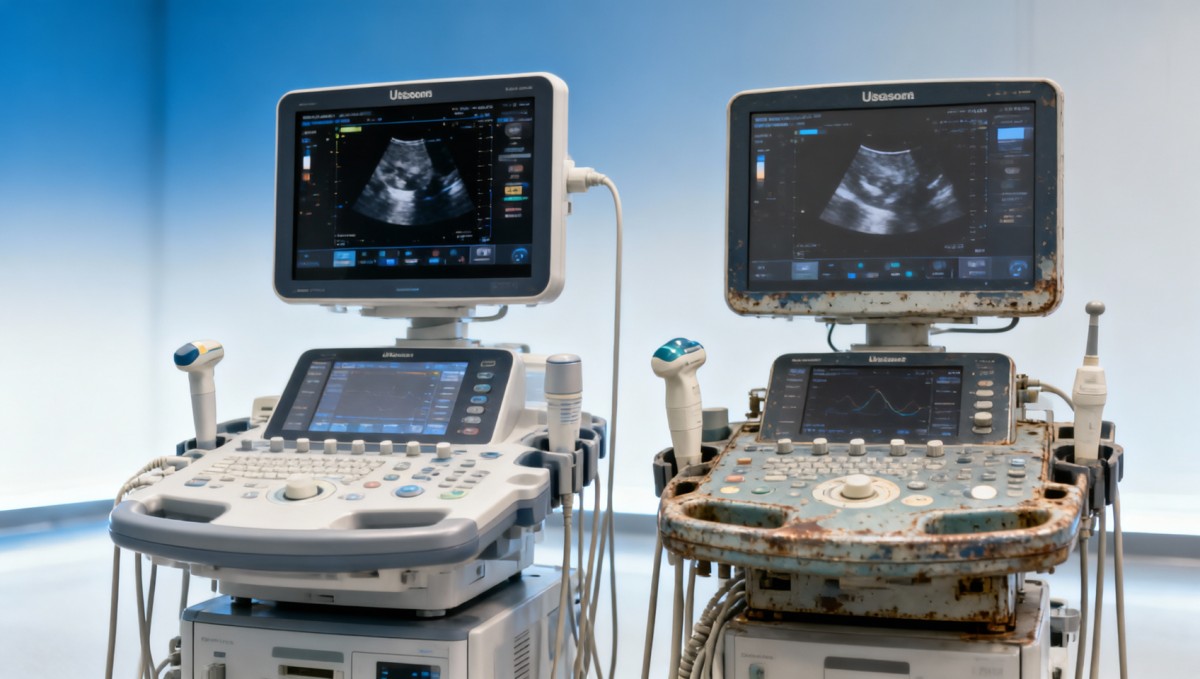
The ultrasound machine market in 2026 is shaped by three practical forces: tighter capital discipline, longer approval chains, and greater scrutiny of uptime. A purchasing team may include a sonographer, biomedical engineer, procurement manager, finance controller, and compliance lead, and each group evaluates the same device from a different angle. That is why the decision is no longer “buy the cheapest acceptable unit” but “buy the option that fits clinical demand, service capacity, and budget over 3–7 years.”
For many hospitals, clinics, imaging centers, and multi-site groups, ultrasound machines now sit inside broader procurement conversations about digital workflows, spare parts risk, cybersecurity, and vendor responsiveness. New systems typically offer the strongest pathway for software updates and manufacturer support, while refurbished ultrasound machines can reduce upfront spend and shorten replacement planning when the use case is well defined.
TradeNexus Pro tracks this category as part of healthcare technology and supply chain intelligence. That matters because ultrasound procurement is rarely isolated. Delivery lead times, regional service availability, probe sourcing, and documentation quality can shift the actual buying decision far more than brochure specifications. In practice, a lower acquisition price may become more expensive if probe replacement takes 4–8 weeks or if acceptance testing reveals undocumented configuration gaps.
A structured comparison helps different stakeholders align faster. Operators want image consistency and user familiarity. Technical evaluators want service history and software clarity. Financial approvers want predictable total cost. Safety and quality teams want documented checks, cleaning records, and traceable installation steps. Without a common framework, ultrasound machine procurement slows down and internal disagreement grows.
What has changed for buyers this year
- Replacement cycles are becoming more selective, with many providers extending equipment use by 1–3 years if preventive maintenance remains stable.
- Refurbished ultrasound machines are under closer review for probe condition, software versioning, and evidence of functional testing before shipment.
- New ultrasound machines are increasingly judged not only by image quality, but also by workflow features, connectivity, and long-term service obligations.
- Cross-border buyers are paying more attention to documentation packs, including installation verification, electrical safety checks, and training readiness.
New vs refurbished ultrasound machines: side-by-side comparison for procurement teams
A useful comparison starts with operational reality, not marketing claims. New and refurbished ultrasound machines can both be valid choices, but they perform differently across budget planning, software access, warranty coverage, and lifecycle certainty. The table below gives a practical procurement view for organizations evaluating replacement, expansion, or temporary capacity support.
This comparison shows why refurbished does not automatically mean risky, and new does not automatically mean optimal. The right choice depends on imaging workload, training needs, financing structure, and the cost of interruption. If a facility performs high daily exam volumes or depends on advanced workflow integration, the premium for a new ultrasound machine can be easier to justify. If the need is overflow coverage, satellite deployment, or a defined specialty with stable requirements, a refurbished unit may be the more rational fit.
Where each option usually fits best
Typical use cases for new systems
New ultrasound machines are commonly preferred for flagship departments, newly opened clinics, and organizations standardizing across several sites. They also make sense when training multiple operators, integrating with newer reporting workflows, or securing a longer support horizon. If your internal requirement is predictable operation over 5 years or more, new systems often reduce policy friction during approval.
They are also favored when the procurement team expects a complete package that includes installation, training, software onboarding, and structured after-sales support. For project managers working on time-bound facility launches, the cleaner documentation path can simplify commissioning and reduce acceptance disputes.
Typical use cases for refurbished systems
Refurbished ultrasound machines often fit outpatient sites, mobile service expansion, secondary procedure rooms, training labs, and staged replacement plans. They can also work well when a buyer needs to restore capacity within 7–15 days and the required feature set is already well understood.
The key condition is discipline in verification. A refurbished machine should never be evaluated only by age or external appearance. Probe condition, keyboard wear, monitor quality, storage performance, included accessories, and service records all influence actual value. Good refurbishment is a process, not a label.
What technical and compliance checks should buyers insist on?
Technical review is where many procurement mistakes can still be prevented. For both new and refurbished ultrasound machines, image quality alone is not enough. Buyers should verify configuration, operating condition, software status, probe compatibility, and acceptance documentation before shipment and again at installation. A machine that scans well in a demo may still create operational issues if ports, presets, or supported transducers do not match the clinical workflow.
In 2026, technical evaluators typically screen 5 core areas: console condition, transducer health, system boot stability, image uniformity, and serviceability. For refurbished units, it is reasonable to ask what was replaced, what was only cleaned, and what was tested under load. For new units, buyers should clarify what is standard, what is optional, and what requires future license activation.
Compliance teams also need practical documentation, not generic assurances. Depending on destination market and facility policy, that may include electrical safety verification, cleaning and disinfection records, serial traceability, user documentation, packing details, and installation checklists. Import procedures and healthcare facility approvals often move faster when the paperwork is complete from the start.
For project owners managing multi-country sourcing, regional support capability matters as much as the equipment itself. A low-priced ultrasound machine becomes difficult to defend if the local team cannot access basic troubleshooting, probe repair options, or replacement parts within a workable time window such as 5–10 business days.
Practical acceptance checklist before purchase approval
- Confirm the exact probe set, frequency ranges, and application presets required for abdominal, vascular, cardiac, obstetric, or point-of-care use.
- Request evidence of power-on testing, image output checks, and control panel functionality across the full user interface.
- Clarify software version, available updates, cybersecurity policy if networked, and any feature licenses that are not permanently included.
- Verify packing method, transit protection, and whether installation support or remote commissioning is part of the supply scope.
- Review warranty boundaries in writing, especially coverage for probes, monitors, keyboards, storage components, and labor response time.
These checks help quality managers and biomedical teams reduce ambiguity before the purchase order is issued. They also improve internal alignment because finance and procurement can see what is actually covered, what remains a future cost, and what operational risks are still open.
How to evaluate total cost, downtime risk, and sourcing efficiency
Price is only one layer of value. The more useful metric is total cost over the expected service period, including delivery, installation, training, preventive maintenance, probes, service calls, and the cost of downtime. A new ultrasound machine may carry a higher purchase price but lower uncertainty in the first 24–36 months. A refurbished ultrasound machine may offer strong value if the workload is moderate and service support is clearly defined.
For financial approvers, three questions usually drive the final decision. First, how long is the machine expected to remain clinically and operationally acceptable? Second, what is the realistic repair exposure, especially for transducers? Third, what revenue loss or scheduling disruption occurs if the unit is unavailable for several days? These questions are often more useful than headline discount percentages.
Procurement efficiency also matters. A buyer may save capital on a refurbished machine yet lose time if documentation, payment terms, logistics, and installation support are fragmented across multiple parties. That is why sourcing intelligence platforms and vetted supplier networks are increasingly relevant. A strong procurement process can reduce approval cycles, improve comparison quality, and prevent rework after arrival.
TradeNexus Pro supports this decision environment by connecting market intelligence with sourcing discipline. For enterprise buyers, the value lies in comparing supplier readiness, documentation depth, logistics feasibility, and service capability alongside the equipment itself. That is especially important when healthcare technology decisions interact with wider supply chain goals such as delivery resilience, cross-border coordination, and capital planning.
Cost factors that should appear in every approval file
Before approval, it helps to convert the ultrasound machine decision into a structured cost worksheet. The table below can be used by procurement, finance, and operational teams to compare new and refurbished options on a more realistic basis.
This framework helps business evaluators move the discussion away from simple invoice price. It also allows project managers to attach operational assumptions to the purchase decision, which is useful when approval requires sign-off from clinical, technical, and finance teams.
How to choose the right ultrasound machine for your use case
The best ultrasound machine choice starts with workload definition. A site performing basic general imaging a few days each week has a very different risk profile from a high-throughput department scanning all day. Start by mapping exam types, number of operators, expected daily utilization, and whether image transfer or reporting integration is required from day one.
A practical selection model uses four filters: clinical fit, technical fit, sourcing fit, and financial fit. Clinical fit means the machine and probes support the required applications. Technical fit means the unit can be maintained within your support environment. Sourcing fit means the supplier can deliver, document, and support the system as promised. Financial fit means the total cost is acceptable over the intended period of use.
For many buyers, the decision becomes clear once they separate essential requirements from optional preferences. If three departments want one system, the buying process often fails because the specification list becomes too broad. Instead, define 5 must-have items, 3 preferred workflow features, and 2 service conditions that are non-negotiable. That structure speeds vendor comparison and avoids overbuying.
Another useful rule is to match the procurement path to urgency. If deployment is required in under 2 weeks, a verified refurbished ultrasound machine from available inventory may be more realistic. If the project is part of a new facility launch with a 3–6 month implementation window, a new machine may support better standardization and long-term planning.
A simple decision path for cross-functional teams
- Define the primary clinical use and minimum probe set before requesting quotations.
- Set the intended service horizon, such as 2–3 years or 5–7 years, to narrow the new versus refurbished choice.
- Ask for documentation packs early, including testing scope, warranty terms, and delivery timeline.
- Evaluate downtime impact and probe replacement exposure before final approval.
- Align procurement, technical, and finance teams on the same scoring sheet so the final recommendation is defendable.
Common mistakes to avoid
One common mistake is treating refurbishment as a single standard. In reality, refurbishment quality varies widely. Some sellers perform structured inspection, cleaning, parts replacement, and functional testing. Others only cosmetically refresh the machine. Buyers should ask what was actually done and request evidence.
Another mistake is focusing on the console but not the probes. A clean main unit with weak or aging transducers can still create a poor operational outcome. The third mistake is underestimating training and workflow fit. Even a technically sound ultrasound machine can reduce productivity if the interface is unfamiliar and onboarding is incomplete.
FAQ: practical questions buyers ask before ordering
Is a refurbished ultrasound machine reliable enough for daily clinical use?
It can be, if the refurbishment process is documented and the machine matches the workload. Reliability depends on platform age, probe condition, parts history, and seller testing discipline. For moderate daily use, a properly verified refurbished system may perform well for 2–5 years. For heavy multi-operator use, buyers often prefer new systems or more extensive support contracts.
What delivery timeline is typical for ultrasound machines?
Typical delivery can range from 7–15 days for ready refurbished inventory to 2–10 weeks for new configured systems, depending on destination, documentation, and probe availability. Buyers should confirm whether the quoted timeline starts from payment, technical approval, or final configuration sign-off.
What should be checked first during supplier evaluation?
Start with five items: exact configuration, probe set, test scope, warranty detail, and support route after installation. These five checks reveal whether the quotation is operationally realistic. If any of them are vague, the purchase risk rises even if the price looks attractive.
When does buying new make more financial sense than refurbished?
Buying new usually makes more sense when the system will be heavily used, shared across departments, or expected to remain in service for 5–7 years with minimal uncertainty. It is also favored when financing conditions are manageable and downtime would create high clinical or scheduling disruption.
Why work with TradeNexus Pro when evaluating ultrasound machines in 2026
TradeNexus Pro is built for buyers who need more than a supplier list. In ultrasound machine sourcing, the real challenge is aligning technical suitability, procurement efficiency, documentation quality, and commercial timing. Our platform supports that process by focusing on decision-grade market intelligence across healthcare technology and adjacent supply chain factors that influence real purchasing outcomes.
For procurement directors, project managers, and enterprise decision-makers, this means faster comparison of sourcing logic, not just product claims. For technical teams, it means clearer visibility into documentation expectations, lifecycle considerations, and service risk. For finance approvers, it means a stronger basis for discussing total cost, not only purchase price.
If your team is comparing new vs refurbished ultrasound machines in 2026, contact TradeNexus Pro for structured support around parameter confirmation, supplier screening, delivery lead time evaluation, refurbishment review points, compliance documentation expectations, and quotation alignment. We can also help frame a shortlist based on intended use, budget range, service horizon, and cross-border procurement requirements.
A strong buying decision starts with the right questions. Reach out when you need help clarifying probe configuration, comparing lifecycle cost, assessing service coverage, planning deployment timing, or narrowing the most suitable ultrasound machine options for your organization.
Get weekly intelligence in your inbox.
No noise. No sponsored content. Pure intelligence.