Intraoral Scanners: What Slows Scan Accuracy in Daily Practice?
In daily dentistry workflows, intraoral scanners are expected to deliver fast, highly accurate digital impressions. Yet in practice, scan precision can degrade for reasons that are often small, cumulative, and easy to miss. The gap between laboratory specifications and chairside outcomes usually comes from operator movement, scanning path inconsistency, reflective or wet surfaces, patient cooperation limits, software stitching behavior, and calibration discipline. For anyone evaluating intraoral scanners for clinical use, service planning, or technology benchmarking, understanding what slows scan accuracy is essential for reducing rescans, comparing systems fairly, and improving digital workflow reliability.
Why a structured review matters when assessing intraoral scanners
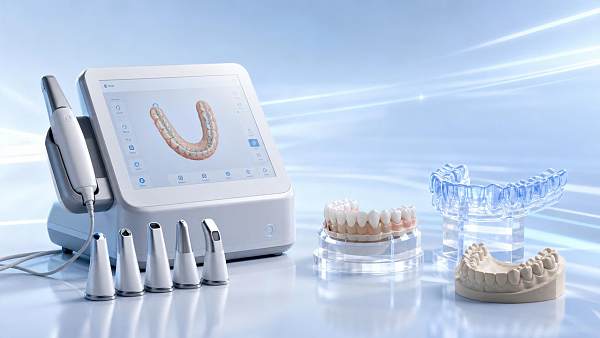
A structured review matters because scan accuracy is not determined by hardware alone. Two clinics using the same intraoral scanners can produce different results if one has better isolation, more stable scanning sequences, stricter calibration routines, or stronger training habits. Without a checklist-based approach, decision-makers may overvalue headline accuracy claims while underestimating real-world workflow drag.
This is also why intraoral scanners should be assessed as part of a broader healthcare technology and digital operations context. Accuracy is affected by the interaction of optics, ergonomics, software logic, connectivity, maintenance, and human factors. In a B2B environment, that makes performance evaluation less about a single specification and more about repeatability under normal daily conditions.
Core points to check when intraoral scanners seem slower or less accurate
The following points help identify why intraoral scanners lose precision in routine use. Each item reflects a practical source of error that can affect scan stitching, margin capture, occlusal detail, and full-arch consistency.
- Confirm whether the scanning path is consistent, because abrupt direction changes and skipped surfaces often force software to guess spatial relationships.
- Check moisture control carefully, since saliva pooling, fogging, and incomplete drying reduce surface readability and introduce noisy data points.
- Evaluate patient motion during longer captures, especially in posterior regions where tongue movement and limited opening disturb image stitching.
- Review reflective materials and translucent restorations, because these surfaces can distort optical capture and lower edge definition.
- Inspect calibration frequency and procedure quality, as delayed or incorrect calibration can shift baseline scanner performance over time.
- Assess operator hand stability and tip positioning, since uneven distance from the tooth surface weakens image consistency.
- Measure how software handles data stitching across long spans, because full-arch scans are more vulnerable to cumulative deviation.
- Verify that scan tips are clean and undamaged, as residue, scratches, or clouding can degrade image quality before capture starts.
- Examine soft tissue management around margins, because mobile gingiva and poor retraction reduce the clarity of preparation boundaries.
- Compare computing performance and update status, since lag, unstable firmware, or outdated algorithms can slow or compromise processing accuracy.
- Test lighting and field contamination factors, especially if ambient reflections or debris repeatedly interfere with capture consistency.
- Separate single-unit, quadrant, and full-arch results, because many intraoral scanners perform well in short spans but drift across larger cases.
How daily workflow conditions slow scan accuracy
Operator technique
Among all variables, operator technique is one of the most decisive. Intraoral scanners depend on a stable scanning pattern with predictable overlap between frames. If the handpiece moves too quickly, rotates abruptly, or loses orientation near posterior teeth, the software may fill gaps with less reliable data. Accuracy problems often appear not as immediate failures, but as subtle distortions that are only noticed later during fit evaluation.
A practical review should focus on path standardization. Start point, arch progression, buccal-lingual sequence, and occlusion capture method should remain consistent across operators. Even highly advanced intraoral scanners will produce variable outcomes if every user develops a different scanning rhythm.
Patient-related variables
Patients introduce movement, moisture, limited access, and soft tissue instability. These variables are especially relevant in pediatric care, elderly cases, limited opening cases, and posterior preparations. When the patient shifts the tongue, swallows repeatedly, or cannot maintain a steady open position, the scanner must re-acquire reference geometry, slowing the process and raising the chance of stitching error.
For this reason, performance comparisons among intraoral scanners should note whether the case mix includes difficult anatomy or compromised cooperation. A system that looks fast on ideal typodonts may not maintain the same accuracy in everyday chairside conditions.
Surface and material conditions
Surface physics matters more than many evaluations acknowledge. Glossy enamel, metallic restorations, highly translucent ceramics, blood contamination, and pooled saliva can all alter how light is reflected or absorbed. This affects feature detection and can create holes, blurred margins, or false continuity across surfaces.
When comparing intraoral scanners, it is useful to test mixed-material environments rather than idealized uniform surfaces. Real mouths contain restorations, wet fields, and varied textures. Systems should be judged on how reliably they capture these combinations without repeated rescans.
Software, calibration, and hardware support
Scan accuracy is strongly shaped by software behavior. Image stitching, noise filtering, AI-assisted reconstruction, and bite alignment all influence the final digital model. Sometimes the issue is not optical capture, but how the software merges datasets. Full-arch deviations, for example, can come from cumulative alignment drift rather than a single bad image.
Calibration routines also deserve closer attention. Intraoral scanners that are not calibrated at recommended intervals may gradually lose consistency, especially in high-volume settings. The same applies to tip wear, firmware mismatches, and underpowered workstations that create lag during rendering or processing.
Application-specific considerations for intraoral scanners
Single-unit restorations
Single-unit scanning is usually the easiest environment for intraoral scanners, but margin clarity still depends on retraction, drying, and stable angulation. The key checks are whether preparation edges remain visible throughout capture and whether neighboring anatomy provides enough reference for software alignment.
Quadrant workflows
Quadrant cases introduce a moderate stitching burden. Accuracy can slow when operators jump between occlusal, buccal, and lingual surfaces without maintaining overlap. Here, intraoral scanners should be reviewed for how quickly they recover from minor tracking loss and how consistently they register interproximal detail.
Full-arch scanning
Full-arch work is where many intraoral scanners reveal their limits. Small local errors accumulate over long spans, and patient movement becomes more likely as scan time increases. The most important checks are arch-length drift, software stitching stability, and repeatability across multiple scans of the same case.
Implant and mixed restorative cases
Implant cases can challenge intraoral scanners because scan bodies require precise geometry capture, and adjacent reflective or soft tissue conditions can interfere with data quality. Mixed restorative environments add more complexity due to different optical responses across metals, ceramics, composites, and natural dentition.
Often overlooked risks that reduce accuracy
Inconsistent retraining: Teams often receive initial onboarding but not periodic refreshers. Over time, scanning paths drift, bad habits return, and different users create different levels of accuracy with the same intraoral scanners.
Overreliance on auto-correction: Modern software can hide weak capture quality by filling gaps or smoothing surfaces. This creates false confidence. A visually acceptable model is not always a dimensionally trustworthy one.
Insufficient maintenance logs: Without records for calibration, tip replacement, software updates, and service events, it becomes difficult to explain why intraoral scanners perform differently over time.
Unfair benchmarking conditions: Comparing systems across different case types, operators, or room setups produces misleading conclusions. Intraoral scanners should be tested under standardized conditions whenever possible.
Ignoring downstream feedback: Fit issues, remakes, or repeated lab adjustments often reveal scan quality problems earlier than internal scan completion metrics do. Accuracy should be judged by outcomes, not only by successful capture on screen.
Practical steps to improve daily scan performance
- Create one standard scan path for each case type and document it with short visual instructions.
- Introduce a pre-scan routine covering isolation, drying, retraction, mirror clearing, and tip inspection.
- Schedule calibration checks and log every event, including software updates and scanner servicing.
- Audit repeatability by rescanning selected cases and comparing deviations across users and sessions.
- Separate performance review by indication, since not all intraoral scanners behave the same across single-unit and full-arch cases.
- Collect downstream fit data from design and production stages to connect scanner performance with restoration outcomes.
FAQ about what slows intraoral scanners in real practice
Do faster intraoral scanners always deliver better accuracy?
No. Speed can improve workflow, but only if tracking remains stable and image data quality stays consistent. Some intraoral scanners feel fast yet require more corrections later.
Why do full-arch scans fail more often than short-span scans?
Because long-span capture increases cumulative stitching error and gives more time for motion, moisture, and operator inconsistency to affect the result.
Can software updates improve scan accuracy?
Yes. Updates can improve stitching algorithms, data filtering, and alignment logic. However, updates should be validated in real cases rather than assumed to improve all outcomes automatically.
Conclusion and next actions
Intraoral scanners do not lose accuracy for one reason alone. Daily performance slows when small operational factors combine: unstable scanning paths, wet fields, mobile tissue, reflective materials, software drift, weak calibration habits, and inconsistent user technique. The most reliable way to assess intraoral scanners is to examine these variables systematically rather than relying on brochure claims or isolated demos.
A strong next step is to build an internal evaluation sheet covering case type, operator, scan duration, rescan rate, calibration status, and downstream fit outcome. That approach makes comparisons more objective and supports better equipment selection, better workflow design, and more dependable digital dentistry results.
Get weekly intelligence in your inbox.
No noise. No sponsored content. Pure intelligence.