Medical Lasers: Which Specs Matter More Than Power Rating?
When procurement teams compare medical lasers, the highest wattage often gets the most attention—but it is rarely the best predictor of clinical performance, operational fit, or return on investment. For business evaluators, the more meaningful specifications are usually wavelength, pulse profile, beam delivery, thermal management, uptime expectations, maintenance burden, and regulatory readiness.
In practical terms, a lower-power system with the right wavelength and pulse characteristics can outperform a higher-power model in a specific specialty. Likewise, a laser that looks impressive on a technical sheet may become a poor investment if consumables are expensive, servicing is slow, or compliance documentation is incomplete. For buyers making sourcing or capital allocation decisions, the key is to assess the full specification stack—not just nominal power output.
This guide explains which specs matter most, why they matter commercially as well as clinically, and how business evaluation teams can compare medical lasers with greater confidence.
What business evaluators should prioritize before looking at power
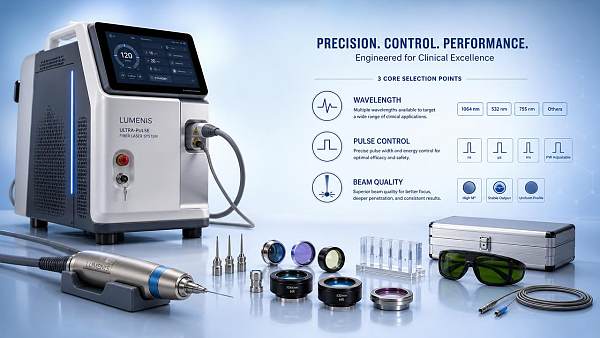
The core search intent behind this topic is not academic curiosity about laser physics. It is a buying and evaluation question: how should we compare medical lasers in a way that reduces procurement risk and improves long-term value? That means the most useful discussion is one that connects technical specifications to use-case fit, revenue potential, maintenance costs, training requirements, and compliance exposure.
For commercial evaluators, the first question should be: what procedure mix is this laser expected to support? A dermatology clinic, ophthalmic center, dental practice, urology department, and hospital surgical unit will each define “best” very differently. The right specification profile depends on target tissue, treatment depth, precision requirements, repetition rate, thermal control needs, and expected patient throughput.
Power rating matters, but mainly as one variable inside a broader framework. On its own, it does not reveal how efficiently energy is absorbed, how much collateral tissue heating occurs, how repeatable the output is, or how suitable the platform is for the intended procedures. A high-power platform may even increase risk if it adds cost and complexity without improving outcomes in the buyer’s real operating environment.
Why wavelength usually matters more than headline wattage
Among all specifications, wavelength is often the most decisive because it determines how laser energy interacts with tissue. Different chromophores—such as water, hemoglobin, melanin, or specific ocular structures—absorb different wavelengths in different ways. This directly affects penetration depth, selectivity, thermal spread, and procedural suitability.
From an evaluation perspective, wavelength is where clinical relevance starts. A system can have impressive power output, but if the wavelength is poorly matched to the procedures the facility performs, the laser may be inefficient, less precise, or commercially underutilized. In contrast, a lower-power system with a wavelength optimized for the intended indication may deliver better outcomes, broader physician acceptance, and stronger utilization rates.
For example, in dermatology or aesthetic applications, tissue targeting may depend heavily on pigment or vascular absorption characteristics. In soft-tissue surgery, water absorption can be more relevant. In ophthalmology, precision at tissue-specific interaction depths becomes critical. Buyers therefore need to ask suppliers not only “how powerful is it?” but “which tissues does this wavelength target best, and for which indications is that useful in our service line?”
This is one of the clearest ways to avoid overbuying. A laser can be technically powerful and commercially wrong at the same time.
Pulse duration and energy delivery often define precision, safety, and versatility
After wavelength, pulse duration and energy delivery profile often matter more than raw power. These specifications influence how energy is deposited over time, which in turn affects precision, thermal injury, patient comfort, healing profile, and treatment efficiency.
Business evaluators should pay close attention to whether a platform operates in continuous wave, long-pulse, short-pulse, or ultra-short pulse modes, and whether those settings align with the practice’s procedural goals. Shorter pulses can reduce thermal diffusion in some applications, while longer pulses may be preferred for controlled heating in others. The point is not that one is universally better, but that the pulse structure must fit the intended indication.
This has direct commercial implications. Better pulse control can expand the number of procedures a device can support, improve physician confidence, reduce adverse event risk, and strengthen patient satisfaction. That can influence utilization rates, reputation, and reimbursement performance. A system that offers flexible pulse settings may therefore be more valuable than a higher-power unit with limited delivery control.
When reviewing vendors, ask for evidence of output consistency across settings. Inconsistent pulse energy or unstable delivery can lead to variable clinical performance and reduce trust among operators. Repeatability is especially important in high-volume environments where standardized outcomes support both efficiency and quality assurance.
Beam quality and spot size affect treatment accuracy more than many buyers expect
Beam quality is frequently underestimated in sourcing discussions, yet it plays a major role in practical performance. Two lasers with similar power ratings may behave very differently if one provides more uniform energy distribution, cleaner beam profiles, or better spot size control.
For precision procedures, especially in specialties where margins are small and tissue preservation matters, beam characteristics can influence targeting accuracy and collateral effects. Poor beam uniformity may require more operator compensation, increase learning curves, and reduce confidence in repeat procedures.
Spot size range is another important buying criterion. A broader and more controllable spot size selection can make a platform more versatile across indications. That versatility matters for buyers assessing utilization and service-line expansion. A laser that can only handle a narrow treatment window may deliver lower long-term value than one that supports multiple applications with reliable beam performance.
Ask suppliers how beam quality is measured, how stable it remains over time, and whether optical degradation affects output consistency. These questions help uncover lifecycle issues that are not visible in a headline power number.
Cooling efficiency, duty cycle, and thermal management shape operational reality
For procurement teams focused on real-world productivity, cooling efficiency and thermal management deserve significant weight. These factors influence uptime, comfort, treatment pacing, and whether the system can sustain high-volume use without performance drops or interruption.
A laser with strong nominal power but weak cooling architecture may require downtime between treatments, limit session throughput, or increase wear on components. In contrast, a platform with a well-designed cooling system may maintain stable operation across longer clinical sessions and support higher daily utilization.
Duty cycle is especially relevant in environments where patient flow matters. If the device cannot maintain output under repeated use, headline specs become less meaningful. Procurement teams should therefore request data on sustained operating performance, not just peak capability.
Cooling also affects patient and operator experience in some applications. Better integrated cooling may reduce discomfort, expand treatment suitability for sensitive cases, and support broader adoption by clinicians. From a business angle, that can improve both scheduling efficiency and patient acceptance.
Service life, maintenance model, and parts availability often determine ROI
For business evaluators, total cost of ownership is often more important than initial purchase price. This is where service life, maintenance requirements, replaceable parts, calibration frequency, and technical support infrastructure become critical.
Medical lasers are capital assets, but they are also service-dependent technologies. A low upfront quote can become expensive if key components have short replacement cycles, if preventive maintenance is frequent, or if field service coverage is weak in the buyer’s region. Procurement teams should evaluate expected lifespan for major components, warranty terms, remote diagnostics capability, and average time to repair.
Another major consideration is consumables and accessories. Fibers, handpieces, tips, cooling modules, software licenses, and calibration tools can materially change cost per procedure. A laser that appears cost-effective on day one may lose its advantage once ongoing operating costs are modeled over three to five years.
Vendor stability matters as well. Buyers should examine whether the manufacturer has a reliable distribution and service network, documented training resources, and a credible installed base. In B2B procurement, equipment value is inseparable from supplier support.
Regulatory compliance and documentation are not secondary details
For any healthcare technology purchase, regulatory compliance is a frontline evaluation issue, not a back-office formality. A laser may be technically impressive, but if approvals, safety documentation, labeling, or market access records are incomplete, the procurement risk rises sharply.
Business evaluators should verify which markets the system is cleared for, what indications are approved, and whether documentation aligns with the intended use environment. Depending on geography, this may include FDA clearance, CE marking under the relevant framework, IEC electrical and laser safety standards, biocompatibility for patient-contact accessories, and local registration requirements.
It is also important to confirm that marketing claims match regulatory scope. Some suppliers imply broad procedural capability while their formal approvals are narrower. That gap can create compliance, liability, and reimbursement problems later.
Training and safety protocols should be reviewed alongside the technical file. A supplier that provides robust user training, risk controls, and documentation support can materially reduce implementation friction. For enterprise buyers, this contributes to smoother onboarding and lower operational risk.
Versatility, reimbursement alignment, and utilization strategy matter for commercial success
Many organizations buy medical lasers not just for one procedure, but as platforms expected to support growth. That makes system versatility an important strategic criterion. However, versatility should be evaluated carefully. More indications are only valuable if they match physician capability, patient demand, reimbursement pathways, and facility strategy.
A versatile platform can strengthen ROI by serving multiple departments or enabling service-line expansion. But complexity can also reduce adoption if workflows become difficult or training burdens rise. Buyers should therefore assess not only the number of potential indications, but also how realistic those indications are within the organization’s operating model.
Reimbursement alignment is especially important for commercial evaluation. If a laser supports procedures with weak reimbursement, uncertain coding pathways, or limited patient demand, utilization may disappoint even if the technology is advanced. On the other hand, a more focused system tied to stable procedure volumes may produce faster payback.
In many cases, the smartest purchase is not the most technically expansive unit, but the one with the clearest path to sustained use.
A practical evaluation framework for comparing suppliers
To make sourcing decisions more defensible, procurement teams should compare vendors across five categories: clinical fit, operational performance, economic model, compliance readiness, and supplier support. This framework helps keep discussions anchored in business outcomes rather than spec-sheet marketing.
Under clinical fit, evaluate wavelength, pulse options, beam quality, spot size, and approved indications. Under operational performance, review cooling, duty cycle, user interface, workflow integration, and output stability. For the economic model, calculate purchase price, consumables, maintenance, service contracts, replacement parts, and projected cost per procedure.
Under compliance readiness, verify approvals, safety standards, documentation quality, and training protocols. Under supplier support, assess geographic service coverage, response time, installed base, reference accounts, spare parts access, and long-term platform roadmap.
A weighted scorecard can help multidisciplinary teams align technical and financial priorities. It also reduces the chance that one attention-grabbing metric—such as power rating—distorts the final decision.
Questions procurement teams should ask before final selection
Before committing to a supplier, evaluators should ask several direct questions. Which procedures generate the majority of expected revenue, and how specifically is this laser optimized for them? How stable is energy output over time and under sustained use? What is the expected replacement cycle for major components? What are the real annual service costs?
They should also ask how quickly field service can respond, what training is included, which accessories are mandatory versus optional, and whether the regulatory scope fully covers the intended applications. If possible, request usage data, case references, and total cost models from comparable installations.
Most importantly, ask vendors to explain trade-offs. A credible supplier should be able to clarify why a given wavelength, pulse architecture, or cooling design is advantageous for specific use cases—and where it may be less ideal. Honest limitation mapping is often a better trust signal than aggressive claims.
Conclusion: power rating is important, but rarely the best buying shortcut
When evaluating medical lasers, power rating should be treated as a supporting metric, not the headline decision rule. For business evaluators, the better predictors of long-term value are wavelength fit, pulse control, beam quality, thermal management, service economics, compliance strength, and alignment with actual utilization strategy.
The most successful sourcing decisions come from connecting technical specifications to commercial reality: what procedures the organization will perform, how reliably the system will operate, what it will cost to maintain, and how quickly it can contribute to revenue and quality goals. In that context, the question is not simply “which laser is more powerful?” but “which laser is more appropriate, sustainable, and profitable for our use case?”
That is the standard procurement teams should use when comparing medical lasers in a competitive healthcare technology market.
Get weekly intelligence in your inbox.
No noise. No sponsored content. Pure intelligence.