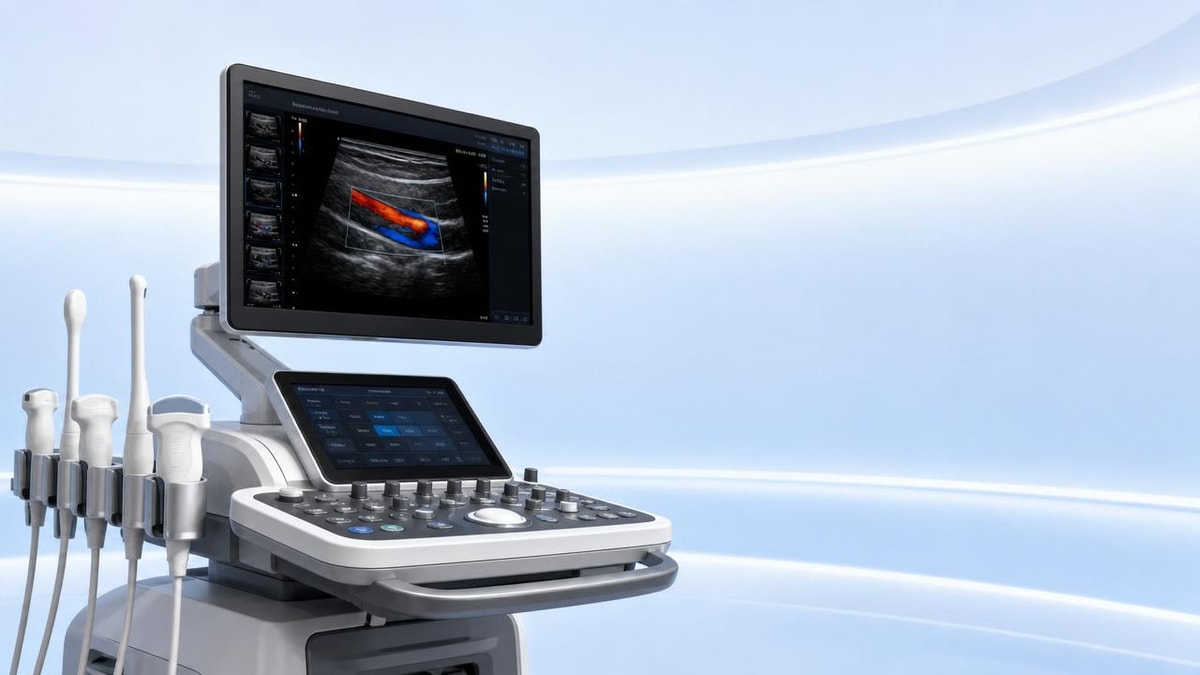
Ultrasound machines: when image quality and workflow clash
For technical evaluators, ultrasound machines often present a difficult trade-off: superior image quality can slow exams, while faster workflow may compromise diagnostic confidence. As healthcare providers push for higher throughput and better outcomes, understanding how system architecture, software optimization, and usability intersect is essential to making smarter procurement and deployment decisions.
Why a checklist approach works better for evaluating ultrasound machines
When teams compare ultrasound machines, they often start with brochure-level claims such as clearer images, AI-assisted measurements, or faster boot-up. That is rarely enough. In real clinical environments, image quality is only valuable if sonographers can obtain it consistently, physicians can trust it across patient types, and operations teams can maintain throughput without increasing fatigue or downtime.
A checklist-based review helps technical evaluators avoid a common procurement error: overvaluing one visible metric while missing the system-level interactions behind performance. For example, excellent spatial resolution may depend on presets that require extra adjustments. A streamlined user interface may save time in routine scans but limit advanced controls in complex cases. The right evaluation method is therefore not “best image” versus “best workflow,” but “which ultrasound machines sustain diagnostic confidence at the speed your care model requires.”
First-pass decision checklist: what to confirm before deep comparison
Before reviewing detailed specifications, technical evaluators should align on a few non-negotiable screening questions. These establish whether a shortlist of ultrasound machines fits the intended operating environment.
- What are the primary exam types: general imaging, cardiology, point-of-care, women’s health, vascular, musculoskeletal, or shared multi-department use?
- What is the average exam duration target, and where does delay usually occur: machine startup, probe switching, image optimization, reporting, or data transfer?
- Which patient factors most frequently challenge performance, such as obesity, motion, low acoustic windows, emergency bedside constraints, or pediatric variability?
- How much standardization is required across locations, operators, and shift patterns?
- What integration level is mandatory with PACS, RIS, EMR, structured reporting, cybersecurity controls, and fleet management tools?
- What service expectations apply, including uptime guarantees, remote diagnostics, software upgrade cadence, and probe replacement lead times?
If these points are not documented first, comparisons between ultrasound machines tend to become subjective and brand-driven rather than operationally grounded.
Core evaluation checklist: how to judge image quality without ignoring workflow
1. Verify image quality under realistic conditions
Do not assess image quality only on optimized demo cases. Ask vendors to demonstrate ultrasound machines on representative patient profiles and difficult scanning scenarios. Review penetration, contrast resolution, clutter suppression, border definition, temporal resolution, and Doppler sensitivity. More importantly, measure how often operators need to intervene to reach acceptable image quality. A system that looks excellent after several manual steps may not perform well in high-volume departments.
2. Measure the workflow cost of image optimization
The hidden cost in many ultrasound machines is the number of touches, menu layers, or mode changes required to move from acquisition to interpretation. Technical evaluators should record time to first image, time to acceptable image, number of manual adjustments per exam, and time to complete measurements and annotations. Workflow should be tested with experienced and mid-level users, because dependence on highly skilled operators may create scaling problems.
3. Check probe and platform architecture
Probe quality, channel architecture, beamforming design, and signal processing heavily influence both image quality and exam speed. Ask whether performance consistency varies across probes, whether transducers share common interfaces, and how quickly the system recognizes and loads presets when probes are changed. For facilities using multiple applications, probe versatility can reduce room turnover delays and training burdens.
4. Review automation critically, not emotionally
AI features in ultrasound machines can improve workflow, but only if they are reliable across real-world cases. Auto measurement, auto optimization, and smart labeling should be tested for repeatability, override flexibility, and failure behavior. Evaluators should ask: when automation is wrong, how quickly can the user detect and correct it? Over-automation that masks uncertainty can damage diagnostic trust.
5. Assess ergonomics as a performance metric
Ergonomics is not a comfort detail; it affects consistency, scan duration, and operator retention. Review monitor adjustability, keyboard logic, trackball placement, touchscreen responsiveness, cable management, cart mobility, and battery design for portable models. In many deployments, the workflow advantage of certain ultrasound machines comes less from software and more from reduced physical strain during repeated exams.
A practical scoring table for technical evaluators
The table below can help create a more balanced review framework when comparing ultrasound machines across departments or procurement rounds.
Scenario-based checks: where priorities change
High-volume radiology or shared imaging centers
In these settings, technical evaluators should prioritize repeatable presets, rapid patient turnover, robust worklist integration, and minimal operator adjustment time. The best ultrasound machines here are not necessarily those with the richest advanced features, but those that maintain acceptable image quality over hundreds of routine exams without workflow drag.
Cardiology and advanced specialty use
For specialty environments, image fidelity and measurement precision may justify more complex workflows. Even so, review whether advanced functions are logically organized and whether quantitative tools reduce reporting burden. In these departments, technical evaluators should distinguish between complexity that supports diagnosis and complexity that simply slows experts down.
Point-of-care and emergency deployments
Portable ultrasound machines in acute care settings require fast boot times, intuitive controls, durable design, battery reliability, and strong image quality in constrained scanning conditions. Here, the cost of workflow friction is immediate. If the interface delays a clinician during a critical decision window, even technically strong image performance may not translate into value.
Common blind spots that distort ultrasound machine selection
- Testing only with vendor application specialists instead of internal users with normal workload patterns.
- Ignoring the time required to train float staff, new hires, or cross-department teams.
- Focusing on flagship image modes that are rarely used in routine care.
- Underestimating probe lifecycle cost, repair frequency, and replacement logistics.
- Treating software upgrades as purely positive without checking workflow changes, validation needs, and cybersecurity implications.
- Failing to compare total output quality, including reports, measurements, labeling accuracy, and archive compatibility.
These blind spots explain why some ultrasound machines perform well in demonstrations but disappoint after deployment. Technical evaluation should reflect operational truth, not idealized test conditions.
Execution plan: how to run a stronger evaluation process
- Define use cases by department, patient mix, and exam volume.
- Create weighted scoring for image quality, workflow, usability, integration, and service.
- Run hands-on trials with real operators and timed scenarios.
- Document exceptions: where image quality drops, automation fails, or workflow becomes inefficient.
- Review total cost of ownership, including probes, licensing, upgrades, and downtime risk.
- Validate deployment readiness: interfaces, training plan, support coverage, and acceptance criteria.
This approach gives procurement teams a defensible basis for choosing ultrasound machines that fit both clinical standards and operational realities. For organizations balancing digital transformation, budget discipline, and service-line growth, that balance is more strategic than any single specification.
FAQ: fast answers for technical evaluators
Should image quality always outweigh workflow?
No. The priority depends on use case. If workflow obstacles prevent consistent image capture, the theoretical quality advantage of some ultrasound machines may never be realized in practice.
What is the best way to compare automation tools?
Measure repeatability, correction time, and operator trust. Automation should reduce steps without reducing transparency.
Which overlooked factor most often affects long-term value?
Probe strategy. Across many ultrasound machines, transducer durability, replacement timing, and application flexibility have a major impact on cost and uptime.
What to prepare before vendor discussions
If your team is moving toward procurement or platform standardization, prepare a practical question set before engaging suppliers. Confirm target exam volumes, required specialties, integration endpoints, user skill mix, expected deployment timeline, and budget model. Then ask vendors to map how their ultrasound machines perform against those exact conditions, not a generic specification sheet.
For deeper review, it is worth requesting benchmark cases, workflow timing evidence, service-level commitments, software roadmap visibility, and probe lifecycle assumptions. That level of preparation supports better decisions and aligns with the data-driven evaluation standards expected by enterprise buyers and sector-focused intelligence platforms such as TradeNexus Pro, where technical assessment, supply chain reliability, and strategic fit increasingly converge.
Get weekly intelligence in your inbox.
No noise. No sponsored content. Pure intelligence.