Medical PPE shortages are easing, but quality gaps remain
Global supply constraints are no longer the only concern in healthcare procurement. As medical PPE availability improves, quality inconsistencies, certification risks, and supplier reliability remain critical challenges for quality control and safety managers. This article examines where the biggest gaps still exist and how procurement teams can strengthen verification, compliance, and sourcing decisions in a more stable but still fragmented market.
For procurement teams, the market has shifted from a pure availability problem to a verification problem. Lead times for many categories of medical PPE have shortened from crisis-era delays of 8–16 weeks to more typical windows of 2–6 weeks, yet product variation between batches, documentation gaps, and uneven factory controls still create operational risk. For quality and safety managers, the key question is no longer only whether PPE can be sourced, but whether it can be trusted at scale.
This matters across hospitals, laboratories, outpatient networks, contract care providers, and industrial health programs that maintain clinical-grade protection. In these settings, a single weak link in medical PPE sourcing can affect fit, barrier performance, worker safety, audit readiness, and even waste costs. A lower unit price may look attractive, but if failure rates rise by even 2%–5%, the downstream cost in reinspection, replacement, and incident management can outweigh the initial savings.
Why medical PPE shortages are easing but procurement risk has not disappeared
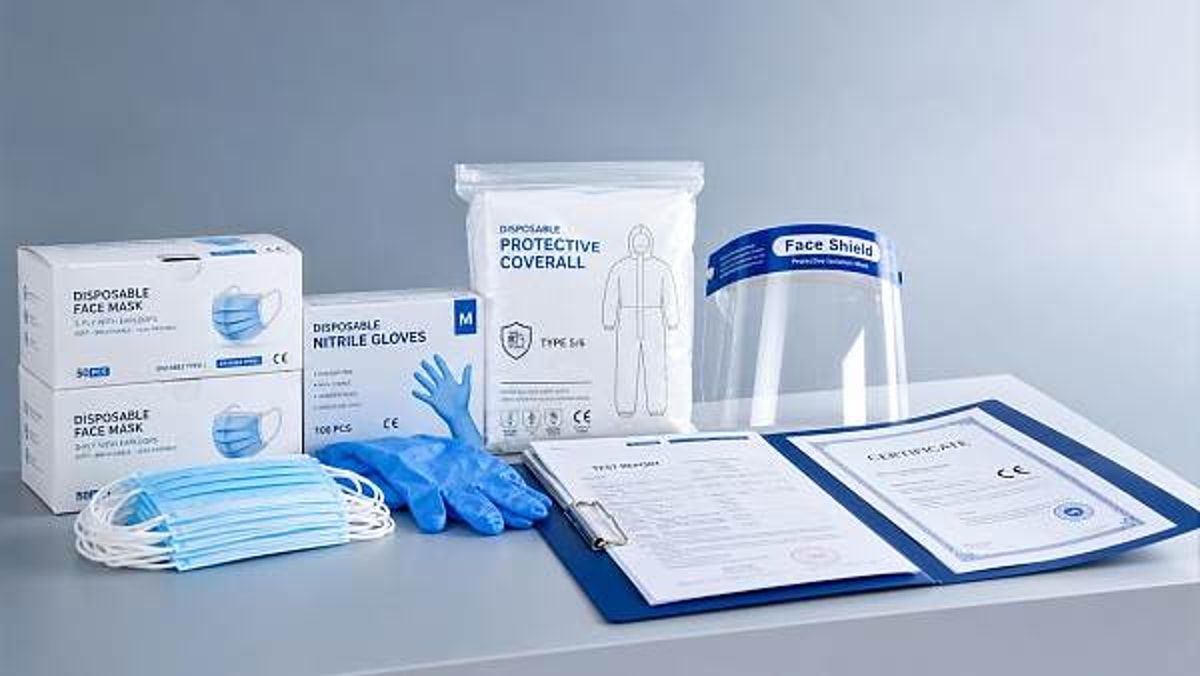
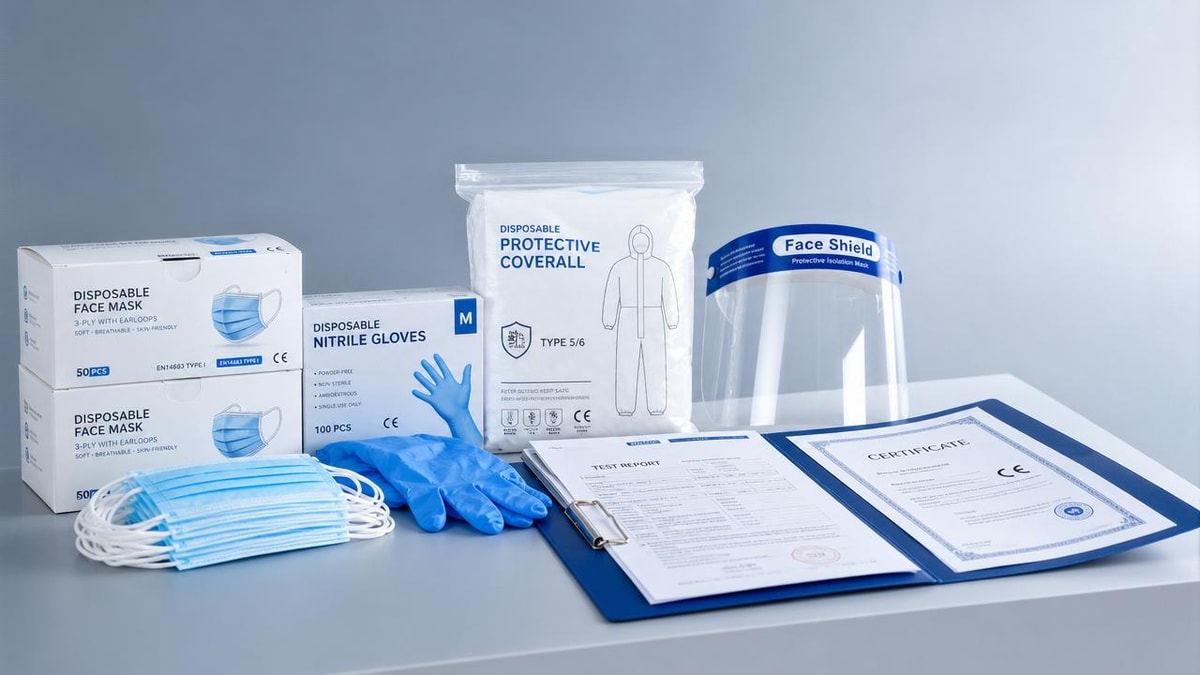
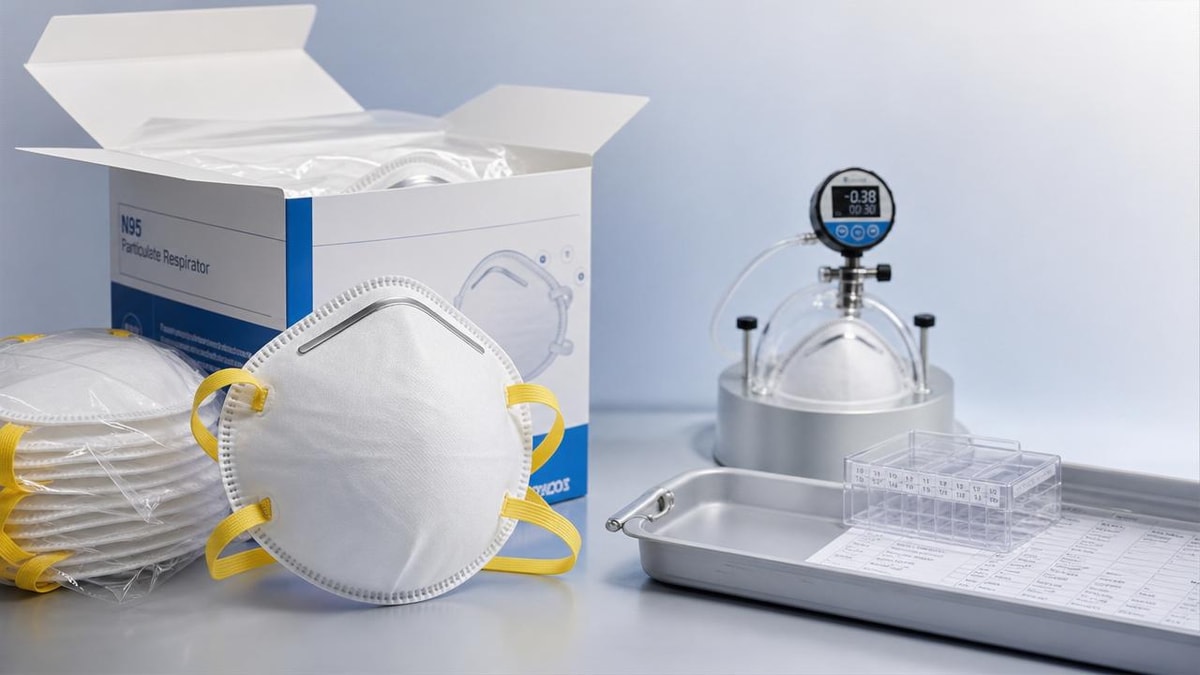
The easing of shortages in medical PPE is largely tied to expanded manufacturing capacity, diversified regional sourcing, and more predictable logistics. Many buyers now see broader access to gloves, masks, gowns, face shields, and respirators than they did 24–36 months ago. However, improved supply does not automatically mean consistent quality. In fact, when more suppliers enter the market quickly, variability often increases before standards stabilize.
The market has moved from scarcity to inconsistency
During peak disruption, buyers often accepted substitute brands and accelerated approvals simply to maintain continuity. That emergency behavior left a legacy issue: supplier lists expanded faster than supplier qualification systems. Today, many organizations still carry 3–5 approved vendors per category, but the depth of validation behind each vendor is uneven. Some suppliers have mature quality systems, while others remain dependent on external traders, changing subcontractors, or inconsistent raw material sources.
This is especially visible in disposable gloves and isolation gowns, where performance can fluctuate by lot, resin source, coating chemistry, or seam integrity. Even where a product technically meets a standard, practical user experience may differ. Tactile sensitivity, tear resistance, fit consistency, and packaging accuracy are all part of the real-world performance picture for medical PPE.
Common quality gaps still affecting safety managers
Quality gaps usually appear in 4 areas: product conformity, document validity, batch traceability, and supplier responsiveness. For safety managers, these are not abstract concerns. A mislabeled respirator, a gown with weak tie attachments, or gloves with elevated pinhole failure can disrupt frontline use within 1 shift. If complaint escalation takes 5–10 business days, the operational burden falls back on the healthcare buyer.
- Certification documents that are outdated, incomplete, or tied to a different product variant
- Lot-to-lot variation in dimensions, weight, tensile strength, or fluid resistance
- Insufficient packaging controls, causing contamination or damaged seals in transit
- Limited visibility into subcontracted production or material sourcing changes
Why stable availability can hide unstable performance
A supplier that can ship 100,000 units within 7 days is not necessarily a low-risk supplier. Availability metrics tell only one part of the story. Quality control teams need evidence of process capability, documented inspections, retained samples, complaint history, and clear corrective action timelines. In many cases, the hidden risk lies not in whether stock exists, but in whether the same specification can be repeated over 6, 12, or 24 months.
The table below outlines where the medical PPE market has improved and where important vulnerabilities still remain for B2B buyers managing regulated or semi-regulated environments.
The key takeaway is clear: supply normalization has improved purchasing flexibility, but it has also increased the need for disciplined validation. For medical PPE, a larger supplier pool should be treated as an opportunity only when paired with stronger incoming quality and documentation review.
Where quality control teams should focus their verification efforts
For quality control personnel, the most effective response is to shift from reactive inspection to structured verification. That means building a repeatable review process before purchase orders scale up. In practical terms, this usually involves 5 checkpoints: specification confirmation, document review, sample approval, production traceability, and post-delivery monitoring. Each step reduces the chance that nonconforming medical PPE enters active use.
1. Confirm the exact product specification
Many procurement errors start with broad descriptions such as “nitrile examination gloves” or “Level 3 gown” without locking in critical details. Teams should confirm at least 6 specification items: material type, size range, sterility status if applicable, barrier level, packaging format, and country of manufacture. If the approved sample is powder-free blue nitrile at a defined thickness range, the purchase contract should not allow silent substitution to a visually similar but lower-performing variant.
2. Review compliance documents against the shipped SKU
Document review must go beyond checking whether a certificate exists. Safety managers should confirm that the file name, product code, revision date, manufacturing site, and applicable standard all match the offered item. A document pack should ideally be reviewed within a 12-month cycle or sooner if there is any packaging change, factory transfer, or material update. In regulated purchasing environments, even a small mismatch can trigger quarantine or audit findings.
Key documents often reviewed for medical PPE
- Product specification sheet and dimensional tolerances
- Test reports relevant to barrier, filtration, splash, or physical integrity claims
- Declaration of conformity or equivalent compliance statement
- Lot coding format and traceability procedure
- Packaging and labeling artwork approval record
3. Use risk-based sampling before full rollout
A practical sourcing strategy is to start with pilot quantities rather than immediate full-volume commitment. For example, instead of moving directly to a 500,000-unit annual award, a buyer may validate 3 pilot lots over 30–60 days. This allows QC teams to check consistency under actual storage, use, and replenishment conditions. The best pilot reviews combine visual inspection, dimensional checks, user feedback, and packaging integrity assessment.
The table below presents a useful verification framework for medical PPE categories commonly purchased by healthcare organizations and safety-led facilities.
A category-based review model helps teams allocate resources more effectively. Not every product requires the same inspection intensity, but every medical PPE category should have a documented acceptance method tied to risk, usage volume, and clinical exposure level.
How to assess supplier reliability beyond price and lead time
Once a product passes basic specification review, supplier reliability becomes the deciding factor. In a fragmented market, two vendors may offer similar pricing and similar sample results, yet perform very differently over 12 months. Buyers should assess supplier reliability through operational indicators, communication discipline, and transparency around production control. This is where many medical PPE sourcing programs either become resilient or remain vulnerable.
Evaluate manufacturing visibility and change control
A dependable supplier should clearly explain whether it is the manufacturer, an authorized distributor, or a trading intermediary. That distinction affects traceability, complaint handling speed, and control over process changes. Quality teams should ask how material substitutions, packaging revisions, and site changes are communicated. A formal notification window of 30–90 days is far safer than informal disclosure after the shipment is already in transit.
Measure responsiveness with operational criteria
Supplier performance should be tracked with concrete service metrics. Useful measures include document turnaround time, nonconformance response time, on-time delivery rate, and complaint closure cycle. For example, a supplier that answers quality deviations within 24–48 hours and provides corrective action within 10 business days usually presents less operational friction than one that takes 1 week just to acknowledge a case.
A practical scorecard for procurement and safety teams
- Documentation accuracy: Are files complete, current, and SKU-specific?
- Quality consistency: Do pilot lots and repeat lots perform within expected tolerance?
- Communication speed: Are questions answered within 1–2 business days?
- Traceability depth: Can the supplier identify lot, site, and production date quickly?
- Corrective action maturity: Are deviations investigated with root-cause detail?
Using a weighted scorecard often gives a better outcome than relying on price comparisons alone. In many B2B healthcare settings, a supplier scoring 85 out of 100 on quality and service criteria may deliver more value than one scoring 70 while offering a unit cost that is 3% lower. The difference often appears later in fewer holds, fewer urgent replacements, and better audit confidence.
Building a more resilient medical PPE sourcing strategy in 2025 and beyond
The next phase of medical PPE procurement is not about returning to old habits. It is about building resilience into a market that now has more supply, but also more variation. For procurement directors, quality managers, and safety leaders, resilience usually means a dual or tri-source model, category-specific validation rules, and closer alignment between sourcing, regulatory, and end-user feedback teams.
Balance source diversification with tighter approval rules
Diversifying suppliers remains important, but excess fragmentation can weaken oversight. A practical approach is to maintain 2 approved suppliers for high-volume core items and 1 qualified backup for surge situations. This keeps optionality without multiplying audit workload. For products with higher use-criticality, such as respirators or surgical barriers, approval standards should be stricter and change management more formal.
Create feedback loops from users to procurement
Frontline feedback should be captured in a structured way, not only when failures occur. Monthly or quarterly review cycles can reveal patterns in fit, donning ease, heat retention, dexterity, or breakage that standard paperwork misses. Even simple 5-point user rating tools can help identify whether a medical PPE issue is isolated to one lot, one site, or one supplier. This is especially valuable when formal test reports look acceptable but user acceptance declines.
Invest in supplier intelligence, not just transaction execution
In a market defined by global trade shifts, tariff changes, and evolving compliance expectations, supplier intelligence is now part of quality assurance. Organizations that monitor manufacturing concentration, regional logistics exposure, and supplier capability changes are better positioned to act before disruption appears. This is where a specialized B2B intelligence platform can support procurement and safety teams by connecting sourcing decisions to market visibility, supplier screening, and sector-specific analysis.
For organizations navigating medical PPE decisions across multiple geographies or product categories, the goal is not simply to buy available stock. The goal is to build a sourcing framework that protects users, withstands audits, and performs predictably across repeated purchasing cycles. That requires sharper qualification standards, clearer cross-functional ownership, and better visibility into supplier reliability over time.
Frequently overlooked mistakes
- Approving a sample without defining acceptable lot-to-lot variation limits
- Accepting compliance files without checking factory location alignment
- Comparing suppliers only on unit cost and not on complaint resolution speed
- Skipping pilot validation because current inventory pressure seems low
- Failing to document who owns quality release when substitute medical PPE is proposed
Medical PPE shortages may be easing, but the quality gap remains a live issue for procurement, QC, and safety leadership. The most effective organizations are treating this new market phase as a call for stronger verification, tighter supplier governance, and smarter data-backed sourcing. TradeNexus Pro helps enterprise buyers and supply chain teams navigate these decisions with deeper market intelligence, sector-focused analysis, and practical visibility into evolving supplier landscapes. To strengthen your medical PPE sourcing strategy, reduce compliance risk, and evaluate supplier options with greater confidence, contact us today to explore tailored insights and procurement support.
Get weekly intelligence in your inbox.
No noise. No sponsored content. Pure intelligence.