Portable Ultrasound Scanners: What to Avoid
Portable ultrasound scanners can expand access to imaging, but poor choices may lead to weak performance, safety risks, and wasted budgets. For buyers comparing portable ultrasound scanners alongside smart glucometers, digital blood pressure monitors, wearable ECG monitors, remote patient monitoring tools, or telemedicine carts, knowing what to avoid is essential. This guide highlights the most common pitfalls so procurement teams, operators, and decision-makers can evaluate options with greater confidence.
For most buyers, the biggest mistake is not choosing a “bad” device on paper, but choosing a portable ultrasound scanner that does not match the clinical task, workflow, connectivity needs, compliance requirements, or service model. In practice, image quality alone is not enough. A scanner that performs well in a demo can still fail in real use if probe options are limited, battery life is weak, software is hard to use, or maintenance support is unreliable. If your goal is safer procurement and better return on investment, focus first on what to avoid.
Do not buy a portable ultrasound scanner before defining the real use case
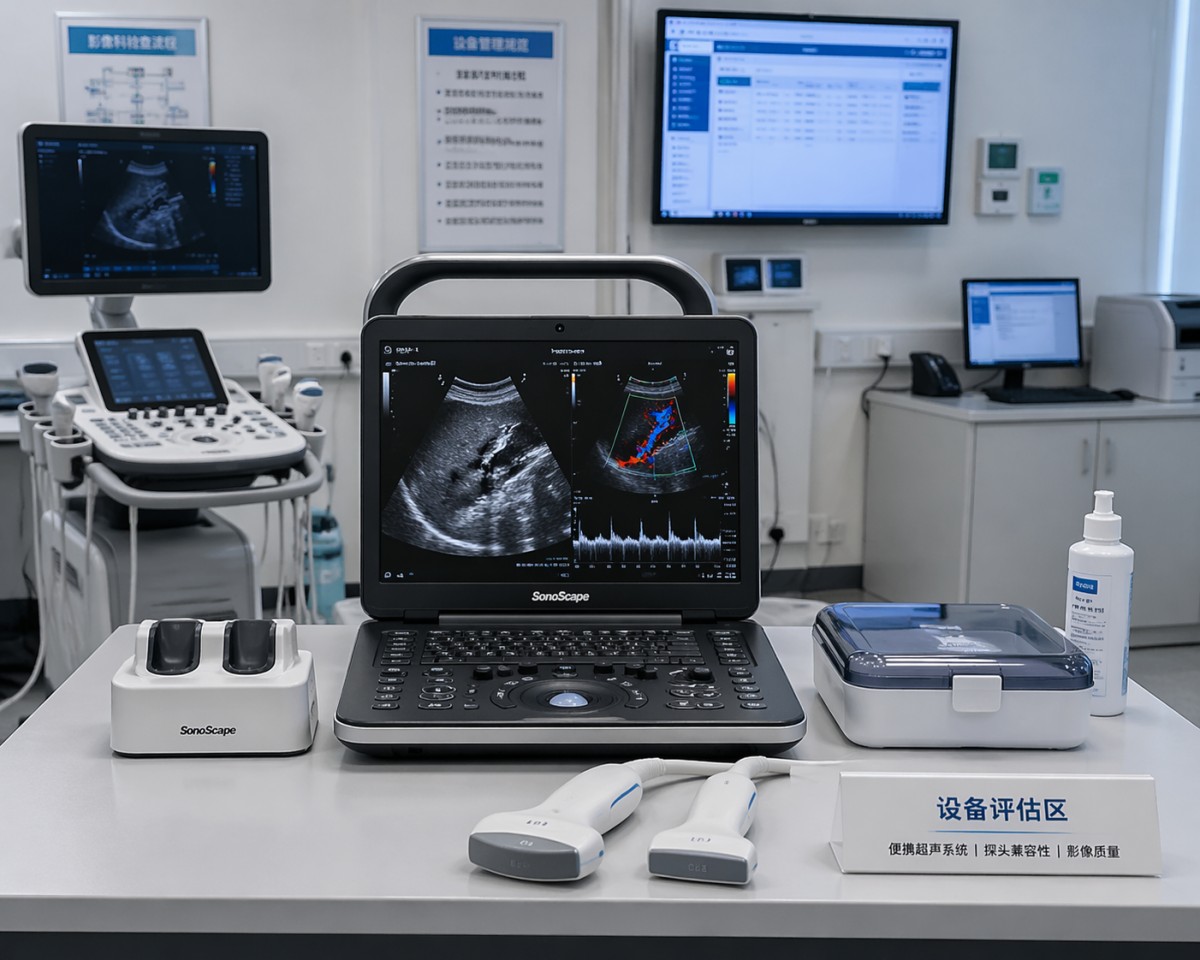
One of the most common procurement errors is treating all portable ultrasound scanners as interchangeable. They are not. A unit suitable for bedside vascular access may be a poor choice for abdominal imaging, obstetrics, cardiac assessment, emergency triage, musculoskeletal exams, or remote outreach programs.
Before comparing brands or prices, clarify the intended use:
- Who will operate the device: radiologists, general physicians, emergency teams, nurses, technicians, or mobile field staff?
- What exams are required most often?
- Will the scanner be used for screening, guided procedures, follow-up imaging, or diagnostic decision support?
- Will it be used in hospitals, ambulances, rural clinics, home care, telemedicine environments, or temporary project sites?
If the use case is vague, buyers often overspend on features they do not need or underbuy and face workflow limitations later. For enterprise decision-makers, this is where budget discipline starts. The best portable ultrasound scanner is the one that fits the real clinical and operational scope, not the one with the longest feature list.
Avoid overvaluing portability while underestimating imaging performance
Portable devices are attractive because they are small, mobile, and easier to deploy across departments or field teams. But extreme portability can come with trade-offs. A highly compact scanner may have limitations in processing power, display size, probe compatibility, thermal stability, battery endurance, or image optimization functions.
Buyers should be cautious if a product is marketed mainly around convenience while offering limited proof of actual imaging performance. Ask practical questions such as:
- Is image quality consistent across deep and superficial structures?
- How does the scanner perform in difficult patients, including higher BMI cases?
- Does it support Doppler modes needed for your application?
- Can users adjust presets quickly in real working conditions?
- Is the display sufficient for confident interpretation?
For quality managers and safety personnel, this matters because weak image performance can lead to repeat scans, delayed decisions, or clinical uncertainty. For finance approvers, poor performance reduces utilization and weakens the business case.
Do not ignore probe ecosystem limitations
Many buyers focus on the main unit and forget that probe selection often determines whether a portable ultrasound scanner remains useful over time. Some low-cost or narrowly designed systems support only one or two probes, which may limit future applications and reduce flexibility across departments.
Probe-related risks to avoid include:
- Limited transducer options for different specialties
- High replacement cost for probes
- Poor durability in high-use environments
- Long lead times for spare parts
- Compatibility restrictions on future upgrades
For procurement teams, probe strategy is part of total cost of ownership. A lower upfront price may become expensive if expansion options are poor or probe replacement is frequent. For distributors and channel partners, a broader probe ecosystem can also improve marketability and long-term customer retention.
Avoid systems with weak workflow integration and connectivity
In many organizations, the value of portable ultrasound scanners depends not only on scanning capability but also on how well they fit into digital workflows. Devices that cannot integrate with PACS, RIS, EHR, cloud review platforms, or telemedicine systems can create bottlenecks even if scanning quality is acceptable.
This is especially important for buyers also evaluating broader connected-care tools such as remote patient monitoring systems or telemedicine carts. If the ultrasound device operates as an isolated tool, clinical efficiency and data continuity may suffer.
Watch for these warning signs:
- Complicated image export or manual file handling
- Weak DICOM support or limited interoperability
- Insecure wireless transmission methods
- No clear user management or audit trail features
- Cloud functions that are difficult to validate for compliance
Enterprise buyers should assess whether the scanner supports actual deployment needs, not just technical marketing claims. Integration failures can increase labor time, create documentation gaps, and reduce confidence among operators and IT teams.
Do not underestimate training requirements and user variability
Even a technically strong portable ultrasound scanner can deliver poor outcomes if the user interface is confusing or training support is weak. This is a major issue in multi-site organizations, mobile programs, and mixed-skill environments where operators have different levels of ultrasound experience.
Common mistakes include assuming that:
- Portable means easy to use
- Short onboarding is enough for all user groups
- Operators will adapt without structured protocols
- Vendor training can be treated as optional
Operational leaders should ask how quickly a new user can become competent for the intended applications. Evaluate preset design, exam workflow simplicity, annotation tools, reporting support, and the quality of training materials. If the scanner will be used in emergency, bedside, or field settings, ease of use under pressure becomes even more important.
For project managers and implementation leads, smoother adoption often matters as much as raw specifications. A device that staff actually use correctly is more valuable than a more advanced system that sits idle.
Avoid unclear compliance, safety, and data security claims
In healthcare technology procurement, vague claims create unnecessary risk. Portable ultrasound scanners may move between locations, users, and networks, which increases the importance of regulatory clarity, infection control suitability, cybersecurity, and device traceability.
Buyers should verify:
- Applicable regulatory approvals in target markets
- Electrical and operational safety standards
- Cleaning and disinfection guidance for probes and surfaces
- Data encryption, user access control, and software update policies
- Documented cybersecurity and privacy protection measures
For quality control teams and safety managers, this is not a secondary issue. A scanner that lacks clear documentation can complicate audits, delay approvals, and increase operational risk. In telehealth or cross-site workflows, data security concerns should be reviewed as carefully as imaging features.
Do not evaluate price without calculating total cost of ownership
A low initial price can be misleading. Portable ultrasound scanners should be assessed based on lifecycle cost, uptime, support quality, training needs, software licensing, accessories, consumables if applicable, and replacement planning.
Total cost of ownership often includes:
- Base unit and probe cost
- Software modules and subscription fees
- Warranty terms and service coverage
- Training and onboarding expenses
- Downtime risk and replacement logistics
- Battery replacement or accessory refresh cycles
Financial approvers and business evaluators should also look at expected utilization. If a scanner is too complex, too limited, or poorly supported, utilization may stay low and ROI may never materialize. A slightly higher-cost model with stronger service support and better workflow fit may create better long-term value.
Avoid vendors that cannot support scaling, service, and accountability
For many B2B buyers, vendor reliability is just as important as device specifications. A portable ultrasound scanner may be used across multiple sites, geographies, or clinical teams. If service response is slow, spare parts are difficult to source, or product support is inconsistent, operational disruption can quickly outweigh any savings.
Vendor due diligence should cover:
- Service network strength
- Response times for technical issues
- Software update history
- Availability of local application support
- References from similar deployments
- Clarity of warranty obligations and escalation paths
This is particularly relevant for distributors, procurement directors, and enterprise buyers responsible for long-term performance. A scanner is not only a product purchase; it is also a service relationship. Weak post-sale support is one of the most expensive mistakes to make.
How to make a better buying decision
If you want to reduce risk when sourcing portable ultrasound scanners, use a structured evaluation framework rather than relying on demos or brochures alone. A practical shortlist process should compare each option across five areas:
- Clinical fit: Does it meet the required exam types and user skill levels?
- Operational fit: Does it suit the care setting, mobility needs, and workflow?
- Digital fit: Can it integrate securely into existing systems?
- Financial fit: Is the total cost justified by expected utilization and outcomes?
- Vendor fit: Can the supplier provide reliable long-term support?
Request real-use demonstrations, not just ideal-condition presentations. Involve operators, procurement stakeholders, IT, quality teams, and finance reviewers early. For larger organizations, pilot testing in a live workflow can reveal issues that specification sheets will never show.
Portable ultrasound scanners can be highly valuable, but only when the purchase decision is disciplined. Buyers who avoid common mistakes are more likely to achieve better clinical utility, lower operational friction, and stronger long-term returns.
In summary, what to avoid is clear: unclear use cases, weak imaging performance, narrow probe support, poor integration, inadequate training, vague compliance claims, misleading low prices, and unreliable vendors. If decision-makers assess portable ultrasound scanners through the lens of workflow, risk, support, and total value, they can make more confident investments and avoid costly procurement errors.
Get weekly intelligence in your inbox.
No noise. No sponsored content. Pure intelligence.



























