Portable Ultrasound Scanners for Small Clinics
Portable ultrasound scanners are reshaping frontline diagnostics for small clinics by improving access, speed, and cost efficiency. For buyers, operators, and healthcare decision-makers comparing portable ultrasound scanners with tools such as smart glucometers, digital blood pressure monitors, wearable ECG monitors, remote patient monitoring systems, and telemedicine carts, understanding performance, integration, and procurement value is essential.
In small clinics, every capital purchase must justify itself across workflow, patient throughput, training effort, and reimbursement potential. Portable ultrasound scanners stand out because they support immediate imaging at the point of care, reduce referrals for routine assessments, and help clinicians make faster decisions in primary care, urgent care, women’s health, musculoskeletal screening, and community outreach settings.
For procurement teams, the question is no longer whether compact imaging has value, but which system profile fits the clinic’s service mix, staffing model, IT environment, and budget cycle. This article examines the practical selection criteria, deployment process, cost factors, and operational risks that matter most to researchers, operators, finance approvers, quality managers, project leads, and channel partners.
Why Portable Ultrasound Matters in Small-Clinic Diagnostics
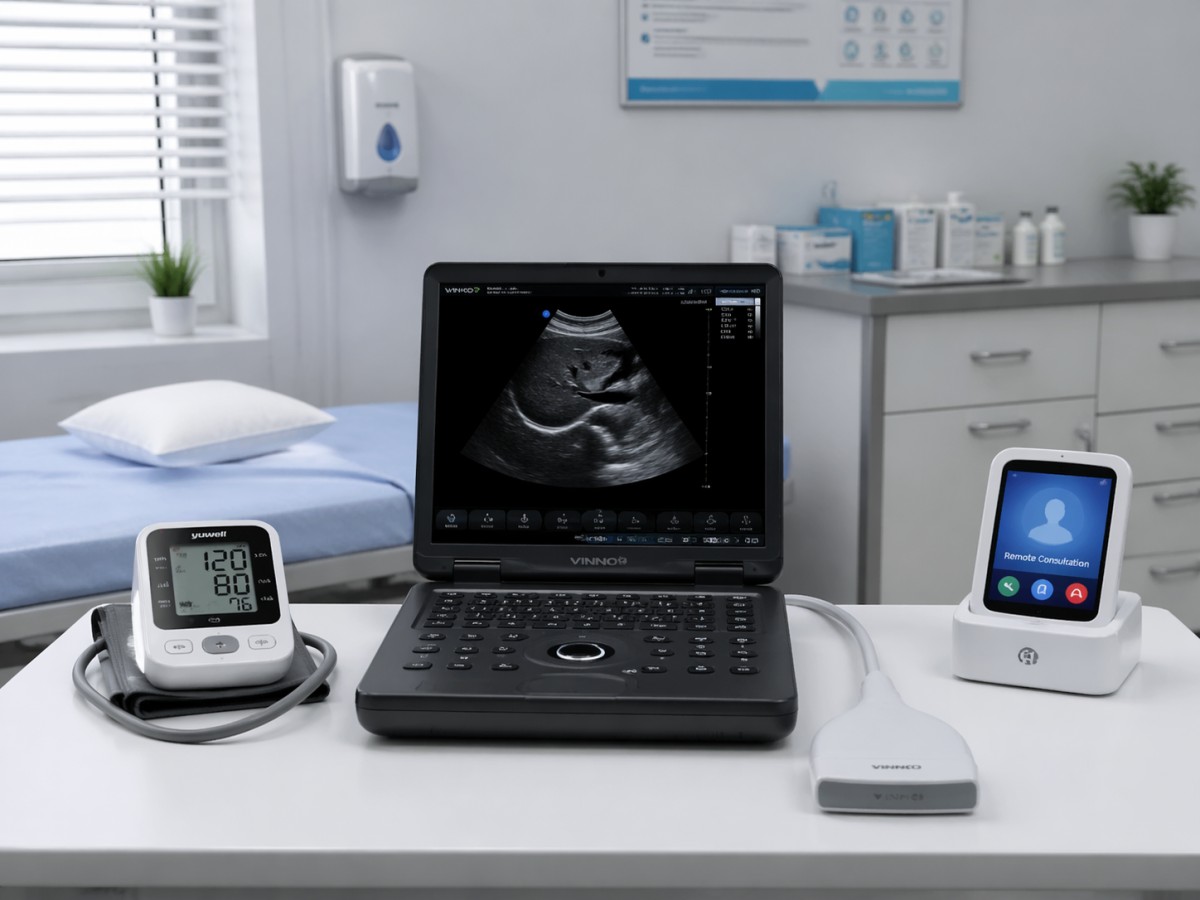
A portable ultrasound scanner is a compact imaging system designed for point-of-care use, often weighing less than 5 kg for cart-light units or operating as a handheld probe connected to a tablet or smartphone. In small clinics, this mobility changes care delivery because imaging can move to the patient rather than forcing the patient into a separate radiology workflow.
The main operational advantage is time. When a clinician can complete a focused scan in 5–15 minutes during the same visit, the clinic reduces delays linked to external imaging referrals, repeated appointments, and administrative follow-up. That improvement matters in practices seeing 20–60 patients per day, where bottlenecks quickly affect revenue and patient satisfaction.
Portable ultrasound also complements other connected diagnostic tools. A smart glucometer or blood pressure monitor can flag chronic disease risks, a wearable ECG can capture rhythm events, and a remote patient monitoring system can track trends over time. Ultrasound adds anatomical and functional context, helping clinicians assess soft tissue, abdominal structures, vascular flow, pregnancy status, bladder volume, or cardiac activity at the bedside.
For business evaluators, the real value lies in service expansion. A clinic that previously offered only basic screening may be able to add first-line obstetric checks, procedural guidance, venous assessment, or musculoskeletal evaluation. Even if only 3–5 use cases are introduced first, the scanner can become a multi-department asset instead of a single-purpose purchase.
However, not every clinic needs the same device category. Some require a rugged handheld platform for outreach and home visits, while others need a laptop-style portable unit with Doppler capability and a larger display for more demanding exams. Selection should therefore begin with care pathways, not with marketing labels.
Common Small-Clinic Use Cases
- Primary care: focused abdominal, bladder, thyroid, and soft-tissue checks during routine consultations.
- Women’s health: early pregnancy confirmation, pelvic assessment, and follow-up triage before referral.
- Urgent care: FAST-style screening, fluid detection, vascular access guidance, and injury review.
- MSK practice: tendon, ligament, joint effusion, and injection guidance for sports or rehabilitation clinics.
Portable Ultrasound Versus Adjacent Diagnostic Devices
The table below shows how portable ultrasound scanners differ from other digital tools often considered in the same procurement cycle. This comparison helps decision-makers avoid treating them as substitutes when they are often complementary assets.
The key takeaway is that portable ultrasound scanners create diagnostic visibility where other devices provide numerical or monitoring data. For clinics building a connected care stack, ultrasound often becomes the highest-impact imaging layer, especially when same-visit clinical decisions are a priority.
How to Evaluate Performance, Features, and Clinical Fit
A practical evaluation starts with image quality, but image quality should be defined by intended use. A clinic focused on bladder scans and basic abdominal checks may not need the same transducer flexibility as a practice performing vascular or cardiac assessments. Buyers should map expected exam types over a 12-month period and identify the 3–6 most common protocols before requesting quotes.
Display size, battery endurance, boot time, and probe options directly affect usability. In small clinics, devices that take more than 60–90 seconds to start or that require frequent cable changes can slow workflow. Battery runtime of 2–4 hours may be enough for room-to-room use, but outreach programs and mobile teams often prefer 4–8 hours or hot-swap support.
Software matters as much as hardware. Features such as auto-measurement, preset templates, image annotation, Doppler modes, and secure exam export reduce the burden on operators who are not full-time sonographers. For clinics with limited training capacity, systems with intuitive interfaces and guided workflows shorten the learning curve and improve consistency.
Probe selection should reflect actual clinical demand. Linear probes are common for vascular and musculoskeletal work, convex probes for abdominal and obstetric scanning, and phased array probes for cardiac applications. Some handheld platforms support one or two integrated probe formats, while modular systems allow multiple transducers but raise total cost.
Quality and safety teams should also review cleaning compatibility, electrical safety documentation, software update policy, and data export controls. In a clinic environment with multiple users across shifts, durability and reprocessing requirements can have as much effect on total ownership cost as the initial purchase price.
Core Selection Criteria
- Clinical scope: define whether the scanner will support general imaging, women’s health, MSK, vascular, or cardiac use.
- Mobility profile: choose between handheld, tablet-based, and compact cartless systems based on room turnover and field use.
- Connectivity: confirm DICOM, PACS, EMR export, Wi-Fi security, and local storage encryption requirements.
- Training burden: estimate whether staff can complete basic adoption in 1–2 days or need role-specific training over several weeks.
- Serviceability: check update delivery, replacement probe lead times, and on-site versus depot support options.
Typical Feature Ranges to Compare
Not every vendor presents technical details in the same format, so procurement teams benefit from a normalized comparison table. This makes it easier to evaluate whether a lower quote is truly lower cost or simply lower capability.
A well-structured comparison often reveals that the best portable ultrasound scanner is not the one with the most features, but the one with the lowest friction for the clinic’s top exam types. That distinction is especially important when the user base includes physicians, nurse practitioners, and technicians with different scanning experience levels.
Procurement Strategy, Cost Control, and Vendor Due Diligence
In B2B healthcare procurement, device price is only one component of the investment decision. A portable ultrasound scanner budget should include probes, software licenses, training, warranty terms, replacement accessories, cybersecurity requirements, and possible integration work. In many small-clinic projects, the 3-year ownership view is more useful than the initial invoice.
Lead time and service coverage deserve early attention. Depending on supplier location, configuration complexity, and import conditions, delivery can range from 2–4 weeks for standard stock to 6–12 weeks for bundled systems with onboarding and integration. For clinics with planned openings or grant-based budgets, timing risk can be just as important as unit cost.
Finance approvers usually ask three questions: how quickly the system will be used, whether it reduces external referral costs, and whether it supports additional billable services. Commercial teams should therefore translate technical features into utilization assumptions such as scans per week, average exam duration, and cross-department use rate.
For distributors and channel partners, packaging matters. Small clinics often prefer simplified bundles that include the primary probe, charger, carrying case, software activation, starter training, and basic support for the first 12 months. Fragmented quotations increase decision time and can create scope disputes after delivery.
Vendor due diligence should extend beyond brochures. Buyers should ask about software update frequency, downtime process, loaner availability, response times, and spare-part access. A lower-cost device can become more expensive if probe replacement takes 30 days and the clinic has no backup unit.
Procurement Checklist for Small Clinics
- Confirm intended exam volume per week and number of active users in the first 6 months.
- Review quote inclusions line by line: probes, software modules, accessories, training, and warranty.
- Verify device compatibility with clinic IT policies, image storage workflow, and user authentication process.
- Request a cleaning and maintenance protocol suitable for multi-user outpatient settings.
- Define acceptance criteria before purchase, including image quality, startup time, export function, and operator sign-off.
Commercial Evaluation Framework
The table below can help procurement teams compare bids in a disciplined way rather than relying only on headline pricing. It is particularly useful when evaluating several vendors or regional distributors.
A disciplined procurement matrix makes cross-functional approval easier because clinical, financial, IT, and quality concerns are visible in one document. That shared visibility often shortens decision cycles and reduces post-purchase surprises.
Implementation, Training, and Operational Risk Management
Successful deployment depends less on unboxing speed and more on structured rollout. Small clinics often assume a portable ultrasound scanner is simple because it is physically compact, but operational adoption still requires protocols, user accountability, and documentation standards. A realistic rollout plan usually spans 2–6 weeks, depending on staffing and IT complexity.
The first priority is defining who can scan, for which indications, and with what escalation pathway. A physician-led clinic may authorize 2–4 core users at launch, while larger outpatient groups may train multiple operators and centralize image review. This helps maintain quality while expanding access gradually rather than allowing uncontrolled use from day one.
Training should combine device operation with scenario-based practice. Operators need more than button knowledge; they need repeatable workflows for probe selection, patient positioning, image capture, cleaning, and report handoff. Even a basic adoption program should include supervised scanning, competency verification, and review of common image-acquisition errors.
Risk management often centers on three areas: poor image quality due to insufficient training, delayed repairs due to weak service terms, and data handling gaps when images are stored on local devices without governance. Each of these risks can be reduced through standard operating procedures, maintenance schedules, and defined escalation contacts.
For project managers and quality leaders, the goal is measurable adoption. Useful metrics include average scan duration, percentage of successful exports, repeat scan rate, cleaning compliance, and user utilization after 30, 60, and 90 days. These indicators show whether the system is actually improving care delivery or simply adding another underused asset.
A Practical 5-Step Rollout Model
- Define scope: select clinical indications, user roles, and documentation requirements before delivery.
- Validate setup: test startup, battery, probe recognition, image export, and local network behavior.
- Train users: combine vendor-led orientation with supervised live or simulated scanning sessions.
- Run pilot phase: monitor the first 20–50 scans for workflow, image quality, and reporting consistency.
- Formalize routine use: approve SOPs, cleaning logs, support contacts, and periodic competency review.
Common Mistakes to Avoid
One frequent mistake is buying a scanner with advanced modes that the clinic will not use in the first year. Another is underestimating the importance of after-sales support. A third is treating handheld imaging as a consumer device rather than a managed clinical asset. In practice, the most resilient deployments are usually the ones with modest scope, strong protocols, and vendor responsiveness defined upfront.
FAQ for Buyers, Operators, and Decision-Makers
How do small clinics choose between handheld and laptop-style portable ultrasound scanners?
Handheld systems are best when mobility, quick triage, and outreach use are priorities. They work well for focused exams and shared-room workflows. Laptop-style portable units are more suitable when the clinic needs larger displays, broader probe support, and more advanced imaging modes. If more than 4 clinical applications are planned from the start, the larger format may offer better long-term flexibility.
What procurement metrics matter most beyond purchase price?
The most useful metrics are time to deployment, number of supported exam types, service response window, training hours required, and expected utilization per week. A cheaper unit may not be the better choice if it lacks export capability, requires frequent downtime, or cannot scale to additional departments within 12–24 months.
How long does implementation usually take?
For a standard small-clinic rollout, basic deployment can often be completed in 1–2 weeks after delivery, while full workflow stabilization may take 2–6 weeks. If EMR or PACS integration is involved, add extra time for testing, user permissions, and acceptance checks. Clinics with a clear pilot protocol generally reach stable use faster than those rolling out to all users at once.
What are the most common quality and safety concerns?
The main concerns are inconsistent image acquisition, inadequate cleaning between patients, unclear operator authorization, and poor data governance. These risks can be reduced by limiting initial access to trained users, documenting cleaning steps, validating export workflows, and reviewing image quality during the first 30 days of use.
Can portable ultrasound scanners support broader digital health strategies?
Yes. In a modern small clinic, portable ultrasound can sit alongside RPM, telemedicine, digital vitals, and connected diagnostic tools. It fills a different role by providing visual clinical evidence at the point of care. When integrated properly, it supports faster triage, more informed referrals, and better documentation for multidisciplinary follow-up.
Portable ultrasound scanners give small clinics a practical way to expand frontline imaging without the footprint or workflow burden of traditional fixed systems. The strongest purchasing decisions are built on clinical-use mapping, normalized vendor comparison, realistic training plans, and clear service expectations over a 3-year horizon.
For procurement teams, operators, and healthcare decision-makers, the right platform is the one that balances imaging performance, portability, integration, and predictable support. If you are evaluating portable ultrasound scanners for a clinic network, channel program, or healthcare technology portfolio, now is the time to review your application mix, define acceptance criteria, and align commercial terms with operational reality.
To explore tailored sourcing insights, supplier comparisons, or healthcare technology market intelligence, contact TradeNexus Pro to discuss your requirements, request a customized evaluation framework, or learn more about solution options for small-clinic diagnostics.
Get weekly intelligence in your inbox.
No noise. No sponsored content. Pure intelligence.



























