Wearable ECG Monitors: Accuracy vs Comfort
As healthcare technology evolves, wearable ECG monitors are drawing attention for their balance between diagnostic accuracy and everyday comfort. For buyers, operators, and decision-makers comparing smart glucometers, digital blood pressure monitors, portable ultrasound scanners, and broader remote patient monitoring solutions, understanding this trade-off is critical. This article explores how wearable ECG monitors perform in real-world use and what matters most for procurement, safety, and long-term clinical value.
Why does the accuracy-versus-comfort trade-off matter in wearable ECG monitors?
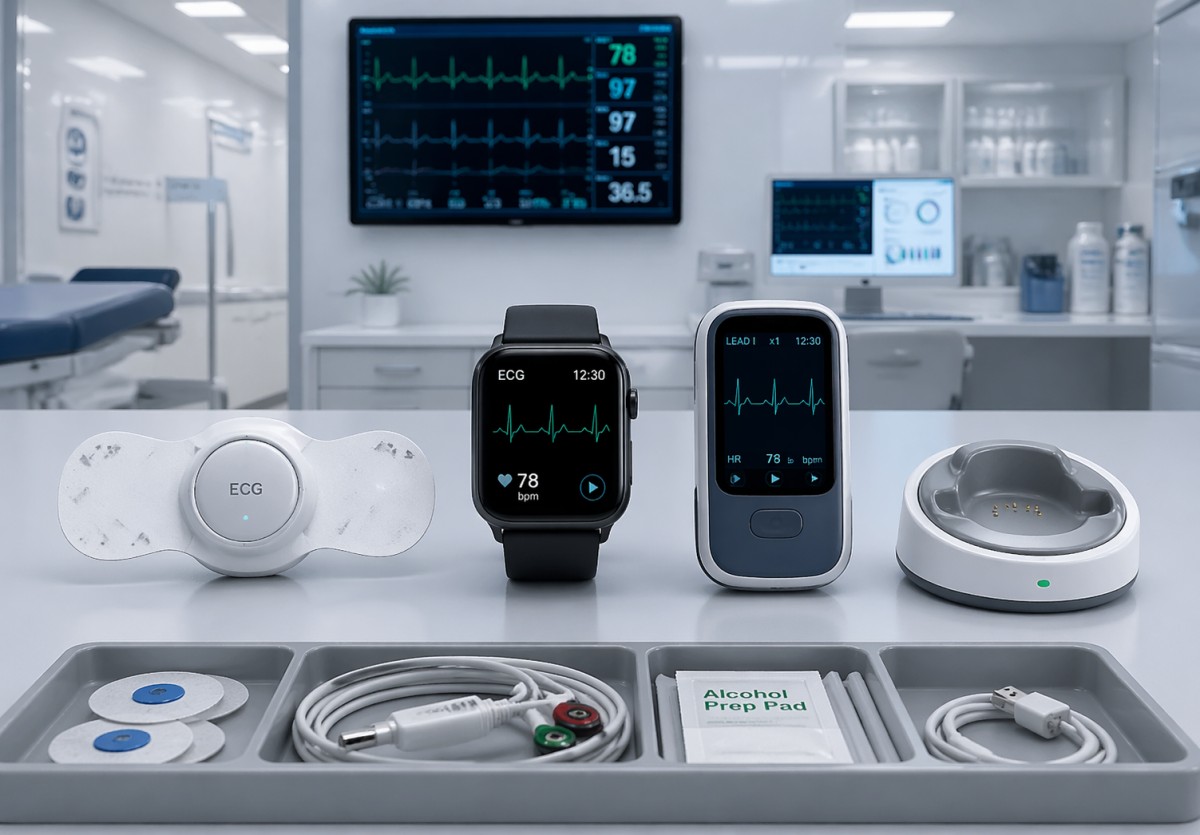
Wearable ECG monitors sit at the intersection of clinical sensing, user compliance, and connected care workflows. In a hospital, outpatient clinic, employer wellness program, or home-monitoring deployment, the device only creates value when it captures interpretable cardiac data over the intended period. That period may range from a spot-check of 30 seconds to continuous wear for 24 hours, 7 days, or even 14 days depending on the care pathway and device category.
Accuracy matters because motion artifacts, electrode placement, skin impedance, and signal dropout can directly reduce diagnostic usefulness. Comfort matters because a highly precise device that patients remove after 6 hours is often less useful than a slightly less intensive form factor that remains on the body for several days. For procurement teams, this is not a simple engineering question. It affects utilization rates, repeat testing costs, training needs, and incident response workflows.
In B2B purchasing, wearable ECG monitors are rarely assessed in isolation. Buyers often compare them against digital blood pressure monitors, smart glucometers, pulse oximeters, and broader remote patient monitoring kits. The question is not only whether the monitor records an ECG waveform, but whether the system fits a care model, an operator skill level, and a reimbursement or budget structure over 1 to 3 years of use.
TradeNexus Pro tracks this category from a cross-sector perspective. That matters because wearable ECG monitors depend on healthcare technology, smart electronics integration, manufacturing reliability, and software interoperability. Procurement directors and enterprise decision-makers need a source that can connect sensor design, supply continuity, regulatory expectations, and deployment practicality instead of viewing the device as a standalone gadget.
Three practical questions buyers should ask first
- Is the wearable ECG monitor intended for intermittent rhythm screening, ambulatory monitoring, or a broader remote patient monitoring program with cloud review and alert handling?
- Can the target user group tolerate the form factor for the required wear duration, such as 8–12 hours per shift, 24–48 hours post-discharge, or 7–14 days in ambulatory follow-up?
- Will the organization evaluate value based on signal quality alone, or on total workflow impact including setup time, consumables, replacement frequency, and integration burden?
These questions help separate a technically interesting product from a procurement-ready solution. They also reduce a common mistake: buying a device optimized for one clinical scenario and forcing it into another where comfort, data transfer, or maintenance requirements are misaligned.
How do different wearable ECG monitor formats compare in real-world use?
Form factor has a direct influence on both ECG accuracy and user acceptance. Chest patches, strap-based devices, watch-style wearables, and lead-based portable systems all offer different trade-offs. A procurement team assessing wearable ECG monitors should compare not only device claims, but also how each design behaves during sleep, walking, work activity, perspiration, and multi-day wear.
The table below summarizes common wearable ECG monitor formats in terms of signal reliability, comfort expectations, and operational fit. These are general industry patterns rather than model-specific claims, but they are useful during early vendor shortlisting and category screening.
For most B2B buyers, patch-based wearable ECG monitors often provide the most balanced profile when the goal is extended ambulatory use with minimal operator intervention. Watch-style devices may fit wellness, screening, or engagement programs, but they should not be assumed equivalent to continuous monitoring systems. Chest straps and lead-based systems may offer stronger signal control in selected contexts, yet comfort and adherence can decline sharply after the first 12–24 hours.
Where each format fits best
Ambulatory cardiology and post-discharge follow-up
In these settings, wearable ECG monitors need to remain stable during sleep, bathing routines, commuting, and normal work activity. Patch devices are commonly favored because they reduce cable management and lower setup complexity. If patient turnover is high, staff also benefit from a faster onboarding sequence that can often be completed in 5–15 minutes rather than requiring more extensive lead placement.
Rehabilitation, occupational health, and activity-linked monitoring
If the organization wants heart rhythm insight during exercise sessions, supervised recovery programs, or physically active work environments, motion robustness becomes more important. Strap or secured patch formats may perform better than casual wearables in these conditions. The trade-off is that some users will tolerate them for a training block or shift, but not for 3–7 consecutive days.
Consumer-adjacent screening and remote engagement
Watch-style ECG wearables can support scalable engagement and symptom-triggered data capture, especially when the goal is early awareness rather than intensive monitoring. For distributors, insurers, or digital health platforms, this format may broaden adoption. Still, procurement teams should distinguish between convenience-led screening and clinically deeper monitoring when comparing offers and total program value.
What technical factors most affect wearable ECG monitor accuracy?
When buyers compare wearable ECG monitors, the biggest accuracy risks are often hidden in deployment details. Electrode-skin contact quality, analog front-end design, sampling approach, filtering strategy, and software interpretation all shape the final ECG trace. A device may perform well on a bench or in ideal demos, yet show weaker real-world results when the user is sweating, repositioning the sensor, or charging the device at irregular intervals.
Battery design also matters. If a wearable ECG monitor needs charging every 18–24 hours, data continuity may suffer in ambulatory programs. If it lasts 5–14 days, comfort and adherence may improve, but the organization must verify whether signal stability remains consistent over the full wear cycle. Long battery life alone is not enough if adhesive wear, electrode drying, or data synchronization failures appear on day 3 or day 5.
Another common issue is overreliance on algorithmic output without checking waveform quality. Automatic rhythm classification can support triage, but poor signal acquisition upstream cannot be fully corrected downstream. Quality managers and safety officers should therefore evaluate both the raw capture pathway and the software reporting layer.
The table below provides a procurement-oriented checklist for technical review. It is especially useful when comparing two or three shortlisted wearable ECG monitors that appear similar in marketing material but differ in service burden and data quality over time.
A useful rule for enterprise evaluation is to score wearable ECG monitors across 4 dimensions: signal reliability, user comfort, workflow compatibility, and lifecycle support. If one device leads in only a single dimension but fails in the other three, it may look attractive in a demo yet create friction in deployment. This is where disciplined procurement outperforms feature-based buying.
Minimum technical review points before approval
- Confirm the intended monitoring duration and whether the device supports that duration without mid-cycle failure or cumbersome recharge behavior.
- Check whether operators need 3 steps or 10 steps to complete setup, because implementation friction scales quickly across larger fleets.
- Review skin-contact materials, replacement accessories, and cleaning procedures if the monitor will be used across varied climates or high-sweat environments.
- Assess export, archive, and review pathways so the wearable ECG monitor does not become a data silo inside a larger remote patient monitoring program.
How should procurement teams evaluate cost, compliance, and implementation risk?
The purchase price of a wearable ECG monitor is only one part of the decision. Financial approvers and project leaders should look at total cost over a 12–36 month horizon. That includes the device or subscription fee, consumables, software access, onboarding time, technical support, replacement policy, and the operational cost of low adherence or repeated monitoring sessions.
Compliance review is equally important. Depending on market and intended use, buyers may need to verify whether the product aligns with relevant medical device regulatory pathways, electrical safety expectations, data privacy controls, and software documentation. Organizations operating across multiple countries should also confirm language support, service responsiveness, and documentation readiness for audits or internal quality reviews.
For distributors and channel partners, another hidden risk is mismatched after-sales support. A wearable ECG monitor may be easy to sell into pilot projects but difficult to scale if consumables are inconsistent, replacement units take 2–6 weeks to arrive, or the vendor cannot support integration discussions with hospital IT teams and digital health platforms.
The procurement framework below helps cross-functional teams align medical, technical, operational, and financial criteria before issuing a request for quotation or beginning vendor negotiations.
A 5-point procurement framework for wearable ECG monitors
- Define the clinical or operational use case first. Screening, ambulatory diagnosis, rehab tracking, and remote patient monitoring do not require the same balance of accuracy and comfort.
- Map the user profile. Elderly users, post-discharge patients, industrial workers, and self-directed wellness participants show different tolerance for adhesives, charging routines, and app interaction.
- Estimate total operating cost over 1 year and 3 years. Include consumables, training, replacements, software fees, and staff review time.
- Check documentation readiness. Ask for regulatory documentation, instructions for use, cleaning guidance, cybersecurity approach, and service response commitments.
- Run a pilot with measurable endpoints. A 2–4 week pilot with 10–30 users can reveal comfort complaints, setup bottlenecks, and data quality gaps before full deployment.
Common implementation mistakes
Buying for specifications only
Some teams focus on waveform claims while ignoring adhesive tolerance, charging behavior, and support capacity. In practice, implementation fails more often because the wearable ECG monitor does not fit daily routines than because the sensor concept is fundamentally weak.
Ignoring staff workflow
If nurses, technicians, or field operators need too many steps to activate, pair, label, and upload each monitor, deployment costs rise quickly. Even an extra 5 minutes per setup becomes significant across 100, 500, or 1,000 monitoring episodes.
Underestimating data governance
A wearable ECG monitor is also a data system. Buyers should confirm retention logic, user permissions, export format, and integration options early rather than treating these as post-purchase details. This is especially important in enterprise health networks and distributed care programs.
Which scenarios justify wearable ECG monitors over adjacent monitoring devices?
Not every monitoring need requires ECG. Buyers comparing wearable ECG monitors with digital blood pressure monitors, pulse devices, or smart glucometers should anchor the decision in the physiological question being asked. ECG is most valuable when rhythm detection, event correlation, or cardiac monitoring continuity is central to care or risk management.
That said, wearable ECG monitors become especially relevant when organizations need more than isolated vital signs. A blood pressure trend or glucose curve can indicate risk, but an ECG trace can add rhythm-specific context during symptom episodes, post-procedure observation, or ambulatory cardiac assessment. For remote patient monitoring vendors, this may strengthen the service proposition in higher-acuity pathways.
The strongest use cases often appear where mobility, compliance, and event timing all matter. In these settings, the comfort of the device directly influences whether enough data is captured to support a clinical or operational conclusion. That is why the best wearable ECG monitor is not always the one with the most technical features, but the one most likely to stay on the user for the required period.
For multi-device procurement programs, a layered strategy may work better than a single-device strategy. For example, a remote monitoring package might combine a wearable ECG monitor for rhythm episodes, a digital blood pressure monitor for hemodynamic tracking, and a glucometer for metabolic risk groups. Selection then depends on program design, not isolated device marketing.
Scenario-based fit
- Post-discharge observation over 3–7 days: wearable ECG monitors can support event tracking without the bulk of traditional setups, provided comfort and battery endurance are adequate.
- Intermittent symptom capture in distributed populations: watch-style or compact ECG solutions may improve adoption if diagnostic depth requirements are moderate.
- Higher-control diagnostic assessments over 24–72 hours: lead-based systems may still be preferred if the workflow can support more complex setup and lower comfort.
- Occupational or rehabilitation environments: secured wearables may outperform casual devices when motion, sweat, and repeated physical activity are expected.
FAQ for buyers and decision-makers
How long does a typical evaluation and procurement cycle take?
For enterprise buyers, a realistic sequence often spans 4 to 12 weeks. Category review may take 1–2 weeks, vendor screening another 1–3 weeks, and a pilot or validation period 2–4 weeks. If regulatory, cybersecurity, or integration review is extensive, timelines can extend further. Planning early prevents rushed decisions driven only by device availability.
What is the most overlooked comfort issue?
Skin tolerance is often underestimated. Adhesive wear that seems acceptable for 8 hours may cause complaints over 3–5 days, especially in warm climates, among elderly users, or in high-mobility settings. A short pilot should include users with different skin types and activity levels rather than only staff volunteers in controlled conditions.
Should distributors prioritize consumer-friendly wearables or clinically oriented systems?
That depends on channel strategy. Consumer-friendly devices may scale faster in wellness and engagement programs, while clinically oriented wearable ECG monitors are more appropriate for care pathways where waveform quality, documentation, and service support matter more than lifestyle design. Many distributors benefit from segmenting offerings instead of forcing one device into every channel.
What evidence should buyers request without overreaching?
Ask for intended use documentation, setup instructions, cleaning or replacement guidance, software workflow explanation, battery specifications, and any generally available regulatory or conformity documentation relevant to the market. If a pilot is possible, define 4–6 success metrics such as wear completion rate, usable recording rate, staff setup time, patient complaints, alert handling time, and data export reliability.
Why work with TradeNexus Pro when evaluating wearable ECG monitor opportunities?
TradeNexus Pro supports B2B buyers, project managers, distributors, and enterprise decision-makers who need more than generic product summaries. Wearable ECG monitors are shaped by healthcare technology requirements, smart electronics design choices, manufacturing stability, and software ecosystem maturity. TNP connects these layers so teams can evaluate vendors and market options with clearer commercial and operational context.
For procurement professionals, that means faster screening of wearable ECG monitor categories, sharper comparison of solution pathways, and stronger preparation before supplier outreach. For distributors and market-entry teams, it means understanding where comfort-led devices, clinical-grade systems, and integrated remote patient monitoring packages fit across different buyer segments and geographies.
If you are assessing wearable ECG monitors for sourcing, channel expansion, program design, or enterprise deployment, TNP can help structure the next step. You can use our platform to clarify parameter priorities, compare solution formats, review implementation risks, and identify where adjacent devices such as smart glucometers, blood pressure monitors, or portable ultrasound tools complement an ECG-centered monitoring strategy.
Contact TradeNexus Pro to discuss practical evaluation points such as device form factor, monitoring duration, comfort considerations, pilot design, estimated delivery windows, documentation expectations, certification questions, sample support, and quotation alignment. If your team needs a clearer shortlist or a more defensible purchasing decision, this is the point where better market intelligence can reduce both cost and deployment risk.
Get weekly intelligence in your inbox.
No noise. No sponsored content. Pure intelligence.



























