Are Telemedicine Carts Worth It in 2026?
As healthcare delivery becomes more decentralized, many buyers are asking whether telemedicine carts will still deliver ROI in 2026. For hospitals, clinics, and distributors comparing remote patient monitoring tools, from portable ultrasound scanners and smart glucometers to digital blood pressure monitors and wearable ecg monitors, the real question is performance, integration, and long-term value. This guide examines what matters most before you invest.
Yes, telemedicine carts can still be worth it in 2026, but not for every buyer and not in every care model. Their value depends on how often they are used, which clinical workflows they support, how well they integrate with existing systems, and whether they reduce labor friction, travel, delays, or missed consult opportunities. For enterprise buyers, the question is less “Are telemedicine carts good?” and more “In which scenarios do they outperform lighter, cheaper, or more specialized remote care tools?”
Are telemedicine carts worth it in 2026? The short answer for buyers
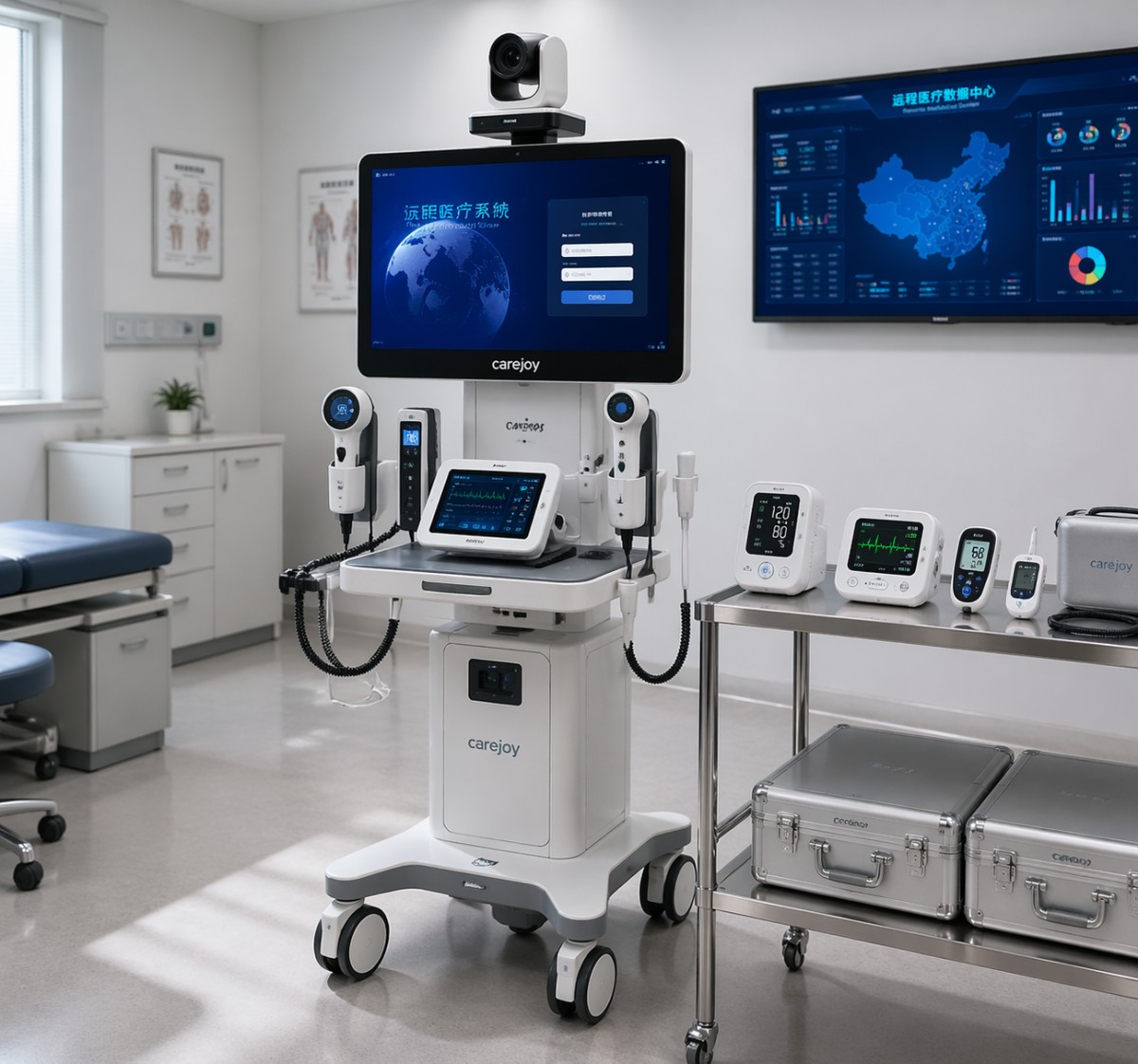
For many hospitals, outpatient networks, long-term care facilities, and urgent care groups, telemedicine carts remain a practical investment when they solve a workflow problem that tablets, fixed-room systems, or standalone devices cannot solve efficiently.
In 2026, the strongest business case usually appears when telemedicine carts are used for:
- Multi-department remote consultations
- Specialist access in understaffed facilities
- Bedside assessments that require mobility and clinical peripherals
- Remote triage in emergency or after-hours settings
- Hospital-at-home and decentralized care support models
- Cross-site care delivery for health systems managing multiple locations
They are usually less compelling when an organization only needs basic video visits, has very low consultation volume, or can meet most needs with lower-cost mobile telehealth kits and connected monitoring devices.
So the investment is worth it when mobility, device integration, clinical-grade communication, and operational reliability matter more than entry-level cost.
What decision-makers actually need to evaluate before buying
Most buyers are not just comparing product specifications. They are assessing whether the cart will create measurable value across clinical, operational, financial, and IT dimensions.
The core evaluation areas are:
- Use-case fit: Is the cart for bedside rounding, tele-specialty consults, ICU support, stroke assessment, discharge coordination, or remote diagnostics?
- Utilization rate: How many consults or assessments will each cart support per day or per week?
- Peripheral compatibility: Can it connect to digital stethoscopes, exam cameras, portable ultrasound scanners, smart glucometers, digital blood pressure monitors, pulse oximeters, and wearable ecg monitors where relevant?
- Integration: Does it work with your EHR, telehealth platform, identity management, device management, and cybersecurity stack?
- Clinical workflow: Will nurses and operators actually use it, or will it become parked equipment?
- Total cost of ownership: Beyond hardware cost, what are the software, maintenance, battery, support, training, and replacement costs?
- Compliance and risk: Does it support privacy, data security, infection control, and documentation requirements?
These factors matter more than screen size, camera resolution, or branding alone.
Where telemedicine carts deliver the strongest ROI
Telemedicine carts tend to justify their cost when they unlock either revenue protection, labor efficiency, or faster clinical response.
1. Specialist access across distributed facilities
Health systems with satellite clinics or regional sites often struggle to provide consistent specialist coverage. A telemedicine cart can help central specialists consult across multiple facilities without travel, improving throughput and reducing delays.
2. Emergency and urgent assessment workflows
In stroke, trauma screening, behavioral health, and after-hours triage, speed matters. A mobile cart can be brought directly to the patient rather than forcing the patient or staff to relocate to a fixed telehealth room.
3. Bedside care in inpatient environments
When providers need video plus attached devices for remote examination, carts outperform consumer-grade tablets. Better audio, camera positioning, power management, and accessory integration improve consistency in real clinical settings.
4. Long-term care and post-acute settings
Nursing homes and rehabilitation settings often benefit from mobile telehealth equipment because patients may have limited mobility and facilities may lack on-site specialists. Avoided transfers and faster escalation decisions can support a meaningful ROI case.
5. Hospital-at-home and hybrid care programs
While many home-based models rely on simpler kits, telemedicine carts still fit command centers, transitional care hubs, and facility-based staging points where multiple connected devices and clinician-grade communications are needed.
When telemedicine carts may not be the best investment
There are many situations where a full telemedicine cart is not the smartest choice.
You may want to consider alternatives if:
- Your primary use case is scheduled video consultation only
- Your team already uses secure mobile tablets effectively
- Clinical peripherals are rarely needed
- Care delivery happens mostly in patients’ homes rather than facility-based environments
- Your budget favors a larger deployment of lower-cost connected devices instead of fewer premium carts
- Your staff lacks time or support for equipment onboarding and maintenance
In these cases, combinations of remote patient monitoring tools may offer better value. For example, portable ultrasound scanners for field imaging, smart glucometers for diabetes monitoring, digital blood pressure monitors for chronic care management, and wearable ecg monitors for cardiac oversight may produce more direct outcome benefits than a cart-heavy approach.
How to compare telemedicine carts against newer remote care tools
By 2026, buyers should not evaluate telemedicine carts in isolation. They should compare them against the broader remote care ecosystem.
A practical comparison framework looks like this:
Telemedicine carts
- Best for mobile, facility-based consults
- Strong for multidisciplinary workflows
- Useful when multiple peripherals are required
- Higher upfront cost, but stronger workflow support in complex settings
Tablets and mobile telehealth stations
- Lower cost and easier to scale
- Suitable for basic video and simple communication workflows
- Less robust in intensive clinical environments
Standalone remote patient monitoring devices
- Best for longitudinal home monitoring
- Excellent for disease-specific programs
- Do not replace the real-time interaction and mobility value of a cart
Integrated hybrid systems
- Often the best option for larger organizations
- Combine telemedicine carts for high-acuity facility workflows with RPM devices for ongoing outpatient monitoring
- Support broader data continuity and better care coordination
For many enterprise buyers, the right answer is not either-or. It is a layered remote care strategy.
What operators, IT teams, and safety managers should check before approval
Procurement decisions often fail because frontline and technical requirements were underestimated. A telemedicine cart may look ideal on paper and still perform poorly in practice if these issues are missed.
For clinical users and operators
- Is the cart easy to move across rooms, elevators, and tight corridors?
- Can the camera be adjusted quickly during bedside use?
- Is audio clear in noisy environments?
- Is battery life sufficient for a full shift or intended use window?
- Are cleaning and disinfection procedures practical?
For IT and security teams
- Does the system support secure authentication and remote management?
- Can it integrate with enterprise software and device fleets?
- How are software updates handled?
- What are the vendor’s cybersecurity controls and incident response commitments?
For quality and safety managers
- Is the hardware stable and safe in active care environments?
- Are cables, mounted peripherals, and charging components managed safely?
- Does the product support infection control protocols?
- Are there documentation trails for maintenance and device performance?
These checks are especially important for larger rollouts where operational failure can scale quickly.
How to calculate total cost of ownership and ROI realistically
In 2026, budget approval will likely depend on a more mature business case than simple hardware pricing.
To estimate telemedicine cart ROI, buyers should model:
- Initial hardware and accessory costs
- Software licensing and telehealth platform fees
- Integration and deployment costs
- Training time for staff
- Maintenance contracts and replacement parts
- Battery replacement and lifecycle management
- Downtime risk and backup workflow costs
Then compare those costs against expected gains, such as:
- Reduced patient transfer costs
- Fewer delayed consults
- Better specialist utilization
- Lower clinician travel time
- Improved patient throughput
- Potential reimbursement support where applicable
- Expanded service coverage without full on-site staffing
A common mistake is assuming ROI will come automatically from “digital transformation.” In reality, telemedicine carts create value only when matched to repeatable workflows with clear volume and accountability.
Questions buyers should ask vendors in 2026
To make a strong purchase decision, ask vendors questions that go beyond marketing claims:
- Which healthcare settings generate the best results with this cart?
- What utilization threshold typically justifies the investment?
- Which peripherals are natively supported, and which require custom integration?
- How does the cart integrate with major EHR and telehealth platforms?
- What is the expected device lifespan under normal clinical use?
- What service response times are included?
- How are updates, patches, and security issues managed?
- What training is provided for frontline staff?
- Can the vendor provide case studies with measurable outcomes?
- What are the most common reasons customers underuse the cart?
The last question is especially valuable because it reveals adoption risk.
Final verdict: worth it for the right workflow, not as a default purchase
Telemedicine carts are still worth it in 2026 when they support mobile, clinical-grade, high-value interactions that cheaper tools cannot handle as well. They are most effective in hospitals, multi-site care networks, urgent assessment environments, long-term care settings, and tele-specialty workflows where mobility, reliability, and peripheral integration are essential.
However, they are not automatically the best investment for every organization. If your use case is mostly routine video communication or home-based monitoring, a combination of tablets, portable ultrasound scanners, smart glucometers, digital blood pressure monitors, wearable ecg monitors, and other connected RPM tools may deliver better returns.
The smartest buyers will evaluate telemedicine carts as part of a broader care technology portfolio, not as a standalone trend purchase. If the cart fits a defined workflow, integrates cleanly, and is used often enough to replace delays, travel, or fragmented assessments, then yes, it can absolutely be worth the investment in 2026.
Get weekly intelligence in your inbox.
No noise. No sponsored content. Pure intelligence.



























