Telemedicine Carts: What Features Matter?
Choosing the right telemedicine carts can directly affect clinical efficiency, patient safety, and long-term ROI. For buyers and healthcare operators comparing remote patient monitoring tools, from portable ultrasound scanners and smart glucometers to digital blood pressure monitors and wearable ECG monitors, the key is knowing which features truly support workflow, mobility, connectivity, and reliability. This guide explains what matters most when evaluating modern telemedicine carts for real-world healthcare use.
For procurement teams, clinical users, project managers, and healthcare technology distributors, telemedicine carts are no longer simple mobile stands with screens. In most care environments, they function as integrated workstations that must support video consultations, device connectivity, battery-backed mobility, sanitation protocols, and secure data transfer across multiple departments.
A poor selection can create bottlenecks within 3 to 6 months: unstable Wi-Fi performance, short battery life, inadequate cable management, or limited compatibility with diagnostic peripherals. A well-matched cart, by contrast, can reduce setup time, improve staff adoption, and extend service life over a 5 to 7 year deployment window.
The most practical evaluation approach is to look beyond headline specifications and focus on workflow fit. Healthcare organizations need to compare mobility, ergonomics, power architecture, infection-control design, peripheral support, and serviceability as one system rather than as isolated features.
Core Clinical and Operational Features to Evaluate First
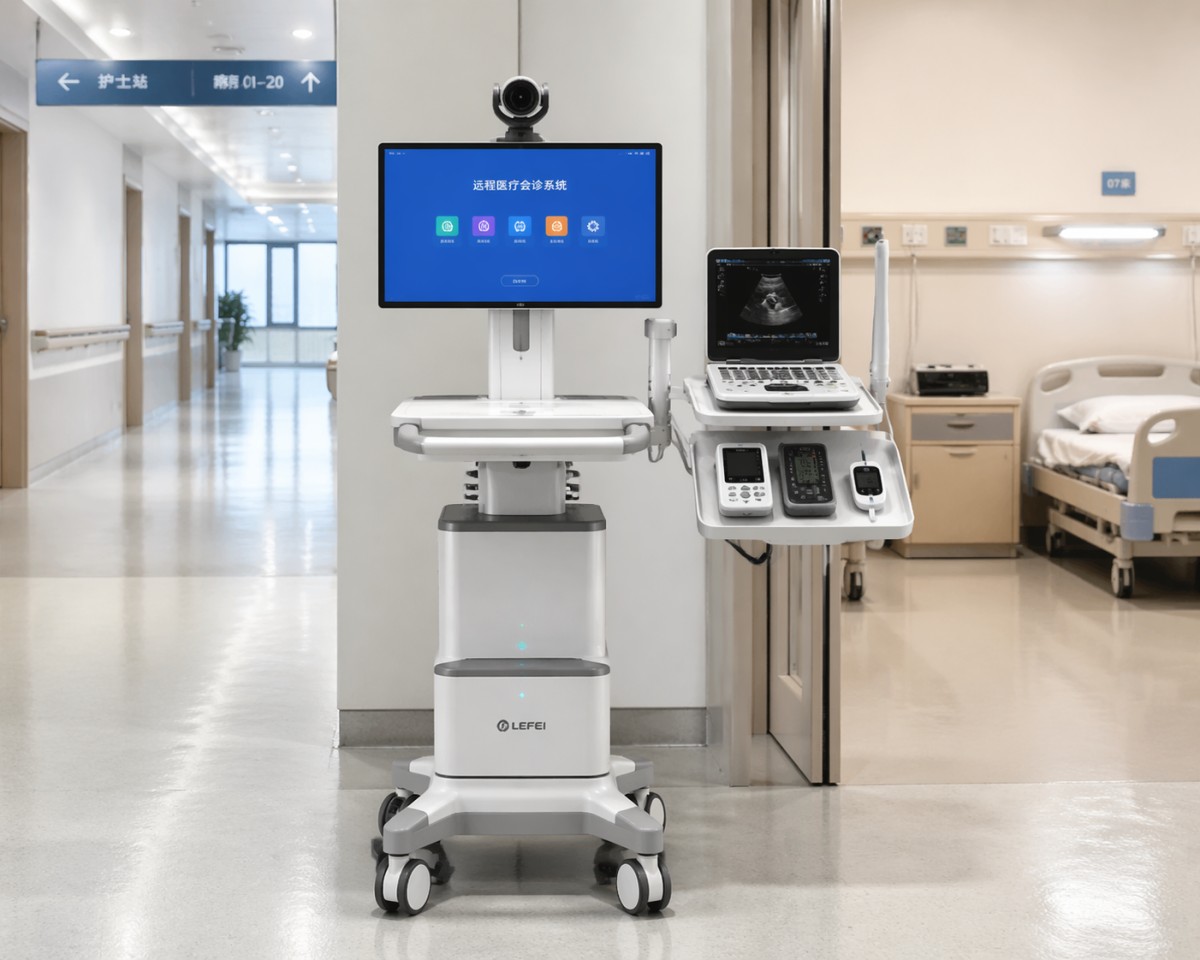
The first screening step is to define where the telemedicine cart will be used. A cart for inpatient rounds, for example, has different priorities than one used in emergency triage, outpatient specialty consults, or long-term care. In fast-moving environments, response time and maneuverability may matter more than large display size. In chronic care settings, stable peripheral integration may take priority.
Most buyers should begin with 4 basic functional questions: Does the cart move easily through narrow corridors? Can it support 6 to 10 hours of operation without recharge? Does it integrate with the cameras, scanners, and monitoring devices already in use? Can frontline staff disinfect all touch surfaces in less than 5 minutes between patients?
Mobility, Stability, and Ergonomics
A mobile cart should be easy to push with one hand, stable during movement, and compact enough for elevators and bedside positioning. In practice, many facilities prefer base footprints that balance tipping resistance with corridor clearance. Casters should roll quietly and lock securely, especially when clinicians are using touchscreens, connected cameras, or point-of-care devices during remote consultations.
Height adjustment is another major factor. If a cart serves both seated and standing users across a 12-hour shift, ergonomic flexibility becomes a productivity issue rather than a comfort issue. Adjustable monitor and work-surface positions can reduce repetitive strain and make documentation easier in shared-use environments.
Power and Runtime Requirements
Battery-backed carts are often expected to support a full shift, but real performance depends on load. A cart powering a display, computer, camera, speaker, and 2 to 4 connected medical devices will drain faster than a video-only unit. Buyers should ask for runtime estimates under realistic use conditions rather than ideal laboratory assumptions.
Hot-swappable battery options can be valuable in hospitals where downtime must be minimized. In larger facilities, centralized charging workflows may support higher fleet availability. In smaller clinics, simple plug-in charging with clear battery indicators may be more practical and lower cost.
The comparison table below highlights the practical feature categories that typically separate entry-level, mid-range, and more advanced telemedicine carts in healthcare operations.
The key takeaway is that feature selection should be tied to care complexity. A simpler cart may be sufficient for scheduled virtual visits, but remote assessment workflows involving vital signs, imaging, or bedside diagnostics usually need stronger power, more robust mounting options, and better peripheral management from day one.
Connectivity, Device Integration, and Data Security
Connectivity is one of the most underestimated purchase criteria. A telemedicine cart may look well designed, but if it cannot maintain stable video sessions or connect reliably to clinical peripherals, user confidence drops quickly. In hospitals and distributed care networks, carts often move between zones with different wireless performance, so antenna placement, signal consistency, and network handoff behavior matter.
Compatibility with remote patient monitoring tools is equally important. Many healthcare teams need carts that can work with digital blood pressure monitors, pulse oximeters, smart glucometers, portable ultrasound scanners, and wearable ECG monitors. The issue is not only whether the port exists, but whether the physical mounting, software workflow, power availability, and cable routing support daily clinical use without clutter or accidental disconnection.
What Integration Looks Like in Real Use
In a real deployment, clinicians may connect 3 to 5 devices during one patient interaction. If the cart lacks organized cable channels, protected USB access, or shelf space for peripherals, setup time increases and infection-control risks can rise. Procurement teams should inspect whether accessories are mounted in a way that preserves balance and allows easy cleaning.
Audio and video quality also affect diagnostic confidence. A high-definition camera alone is not enough. The cart should position the camera at an appropriate eye level, support clear microphone pickup in noisy wards, and provide screen visibility under mixed lighting conditions. These details often have a greater effect on remote exam quality than raw resolution numbers.
Security and IT Governance Checklist
From an IT and compliance perspective, telemedicine carts should support secure login, controlled peripheral access, protected storage for computing components, and simple patching or device replacement workflows. Enterprise buyers should ask whether maintenance teams can access batteries, PCs, and network modules within 10 to 20 minutes without dismantling the full cart.
The checklist below can help cross-functional teams review device integration and security readiness before issuing an RFQ or approving a pilot rollout.
For enterprise decision-makers, the strongest carts are those that fit both clinical and IT workflows. A solution that performs well in a demo but requires frequent adapter changes, special reboots, or manual workarounds will usually increase hidden operating cost over the first 12 to 24 months.
Build Quality, Infection Control, and Service Life
Durability is not just about frame strength. In healthcare environments, telemedicine carts are exposed to repeated cleaning cycles, door impacts, rapid repositioning, and shared-use wear across multiple shifts. Materials should resist common disinfectants, and exposed joints should be minimized so staff can clean surfaces thoroughly without trapping residue around controls, shelves, or handles.
Infection-control design should be reviewed with the same seriousness as electrical and network specifications. A cart used in isolation rooms, emergency departments, or high-turnover clinics may be disinfected dozens of times per week. Rounded edges, sealed surfaces, and simpler accessory layouts often outperform feature-heavy designs that create dust traps and cleaning blind spots.
Serviceability and Lifecycle Planning
A cart with a projected service life of 5 to 7 years should allow practical maintenance. If replacing a worn caster, battery module, or monitor arm requires specialty tools or complete disassembly, maintenance cost rises. Buyers should ask about spare part availability, typical lead times, and whether modular replacement can be performed on site within one service visit.
This is especially important for organizations managing fleets of 10, 50, or 100 units across multiple sites. Even low-cost carts can become expensive if downtime, emergency repair logistics, and inconsistent component availability disrupt care delivery. Distributor networks and regional support coverage are therefore relevant commercial criteria, not just after-sales details.
Practical Quality Checks Before Approval
Before final vendor selection, teams should conduct a structured inspection that includes mechanical stability, cleanability, battery access, cable protection, and repeated movement testing. A practical pilot often runs for 2 to 4 weeks and should involve both clinical users and biomedical or IT support staff.
- Check whether the cart remains stable when a monitor arm is extended and accessories are mounted on one side.
- Verify that surfaces can be wiped quickly and consistently after each patient encounter.
- Review whether power components, batteries, or computing hardware can be replaced without long service interruptions.
- Confirm that casters, brakes, and handles still perform smoothly after repeated transport across thresholds and uneven flooring.
These checks help quality managers and safety teams identify risks early. In many purchase projects, the difference between a successful rollout and a problematic one is not the headline feature list, but how the cart behaves after 30 days of real use in high-frequency clinical workflows.
How Procurement Teams Should Compare Telemedicine Cart Options
Procurement should treat telemedicine carts as a total-solution investment rather than a unit-price purchase. The visible hardware cost is only one part of the equation. Integration labor, training, battery replacement cycles, accessory mounting, maintenance response time, and software environment compatibility all affect total ownership cost over a 3 to 5 year planning horizon.
A strong sourcing process usually combines 5 decision lenses: intended clinical use, technical compatibility, durability, support model, and commercial terms. Enterprise buyers may also add deployment scalability, distributor capability, and parts availability by region. This matters for cross-border projects where service lead times can vary significantly.
Questions to Include in an RFQ
Well-structured RFQs reduce comparison confusion. Instead of asking only for general product brochures, buyers should request runtime under typical load, supported accessory configurations, cleaning guidance, recommended preventive maintenance intervals, replacement part lead times, and implementation support. This helps finance approvers compare long-term value more accurately.
The following table can be used as a practical decision matrix during vendor review, pilot scoring, or internal approval meetings.
The main conclusion is that the best-value telemedicine cart is often not the lowest-priced model. For distributors, healthcare groups, and project owners, the more reliable approach is to quantify operational risk. A cart that avoids even a small number of workflow failures per week can justify a higher upfront investment.
Recommended 5-Step Selection Process
- Map the care scenario: inpatient, emergency, outpatient, long-term care, or mixed use.
- List required peripherals, power needs, and software or network constraints.
- Run a pilot for 2–4 weeks with clinical and technical stakeholders.
- Compare 3–5 year ownership cost, not just purchase price.
- Confirm training, spare parts, and post-install support before approval.
Common Mistakes, Deployment Risks, and FAQ
Many telemedicine cart projects underperform because buyers focus too heavily on visible features such as display size or camera resolution while neglecting fleet management, accessory fit, and support logistics. Another common mistake is testing the cart in a conference room instead of in real patient-care areas where floor transitions, room layouts, and cleaning pressure quickly expose design weaknesses.
There is also a recurring gap between procurement and end-user expectations. A finance team may prioritize lower initial cost, while nurses or operators need fast mobility, easy disinfection, and reliable device charging throughout a 10 to 12 hour shift. Aligning these priorities early can prevent expensive change requests after deployment.
What are the most common buying mistakes?
The top errors are underestimating battery load, ignoring peripheral mounting needs, accepting unclear service terms, and skipping pilot validation. A cart that works for video alone may perform poorly once you add an ultrasound probe, vital signs monitor, barcode scanner, and charging accessories. Always review use cases under expected load, not simplified demo conditions.
How long is the typical delivery and implementation cycle?
For standard configurations, procurement and delivery may take 2 to 8 weeks depending on region, integration complexity, and accessory requirements. More customized deployments, especially those involving multiple peripherals or fleet rollouts, may require additional staging, validation, and user training before go-live.
Which environments need more advanced carts?
Emergency departments, high-acuity wards, isolation units, and multi-specialty hospitals usually benefit from more advanced telemedicine carts with stronger battery systems, better cable control, and more flexible mounts. Smaller outpatient clinics may succeed with lighter configurations if consult duration is shorter and device integration needs are limited.
Final practical guidance
The features that matter most are the ones that survive everyday use: stable mobility, realistic battery runtime, smooth device integration, easy cleaning, secure data handling, and dependable support over time. For B2B buyers evaluating telemedicine carts at scale, the right choice is the model that fits workflows across users, departments, and maintenance teams—not just the one that looks strongest on a specification sheet.
If you are assessing telemedicine carts for healthcare operations, distribution, or enterprise procurement, use a structured comparison process and validate every critical feature in the field. To explore more healthcare technology sourcing insights, request a tailored evaluation framework, or discuss solution-fit criteria for your market, connect with TradeNexus Pro and get a more informed path to selection.
Get weekly intelligence in your inbox.
No noise. No sponsored content. Pure intelligence.



























