Best Smart Glucometer Features for Daily Use
Choosing the best smart glucometer for daily use is less about finding the device with the longest feature list and more about selecting one that delivers reliable readings, easy day-to-day operation, secure data sharing, and sustainable total cost. For individual users, care teams, and procurement stakeholders alike, the smartest choice is usually a meter that combines clinically credible accuracy, seamless app connectivity, low-friction testing, and dependable supply availability for strips and lancets. In practice, the best smart glucometer features are the ones that improve adherence, reduce user error, support remote monitoring, and fit real operating environments rather than just sounding advanced on a spec sheet.
As healthcare technology becomes increasingly connected, smart glucometers are no longer standalone devices. They now sit within a broader ecosystem that may include remote patient monitoring tools, digital blood pressure monitors, wearable ECG monitors, portable ultrasound scanners, and other connected diagnostic systems. That makes feature evaluation especially important for buyers comparing products for personal use, clinics, home care programs, distributors, or enterprise healthcare deployment.
What features actually matter most in a smart glucometer for daily use?
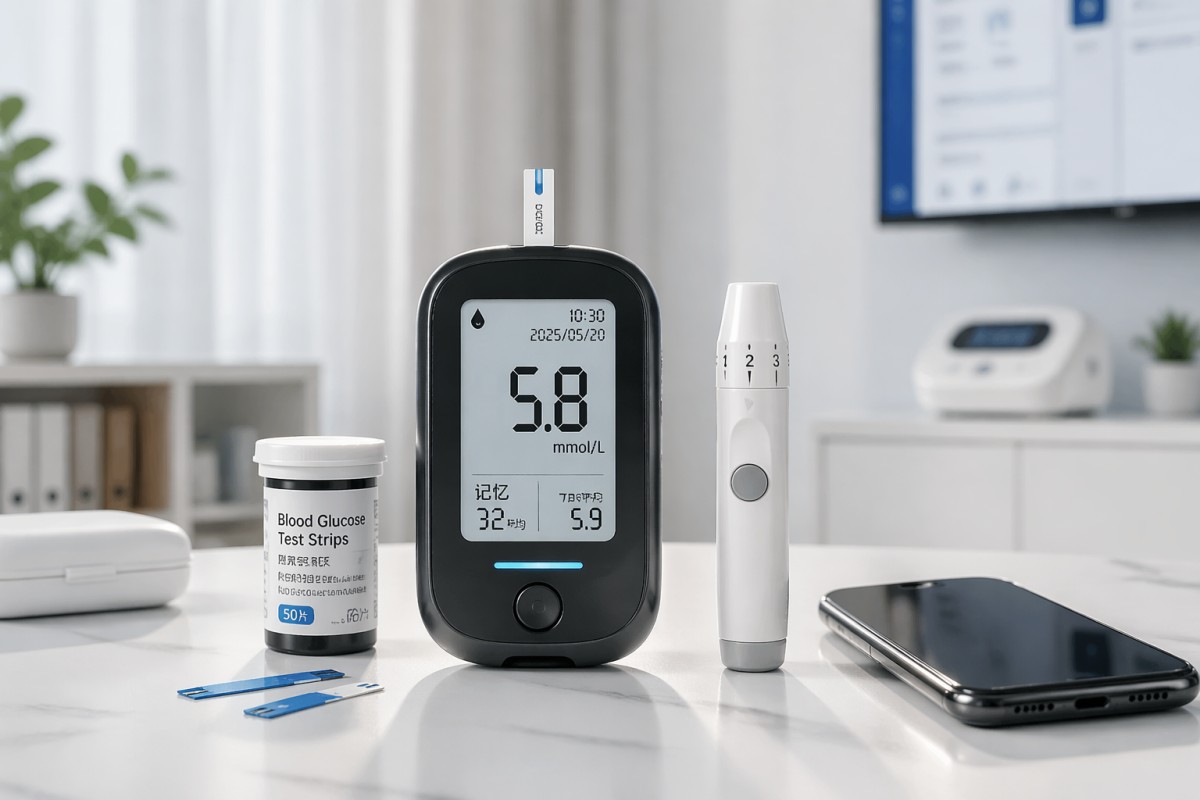
The most valuable smart glucometer features are the ones that consistently improve accuracy, usability, and decision-making. For daily use, priority should usually be given to the following:
- Measurement accuracy and consistency: A smart interface is meaningless if the glucose reading is unreliable. Buyers should first verify compliance with recognized accuracy standards and look for evidence of stable performance across different usage conditions.
- Fast and simple testing workflow: Small blood sample size, quick result time, and intuitive strip insertion reduce user frustration and testing avoidance.
- Bluetooth or app connectivity: Automatic syncing eliminates manual logging errors and makes trend review easier for users, caregivers, and clinicians.
- Clear data visualization: Daily, weekly, and meal-linked trend charts often provide more practical value than raw readings alone.
- Hypo/hyper alerts and reminders: These support adherence and timely action, especially for users who test several times per day.
- Multi-user or caregiver sharing options: This matters for elderly users, chronic disease management programs, and remote support models.
- Long-term operating cost: Strip pricing and supply continuity often influence satisfaction more than the meter’s initial purchase price.
If a buyer has to narrow the list quickly, the best starting filter is simple: accuracy first, usability second, connectivity third, and total cost of ownership fourth. Most poor purchase outcomes happen when flashy app features are prioritized over dependable testing performance and consumables access.
How should users and buyers judge accuracy beyond marketing claims?
Accuracy is the core feature because every downstream action depends on it. A glucometer may influence food decisions, insulin dosing, physician review, and chronic disease monitoring. For that reason, readers researching the best smart glucometer should treat “smart” as an added layer, not the primary value proposition.
Useful evaluation points include:
- Regulatory and standards alignment: Check whether the product is cleared or certified for its target market and whether the manufacturer references accepted blood glucose accuracy standards.
- Clinical validation transparency: Stronger suppliers provide test methodology, comparison data, and quality documentation rather than generic accuracy language.
- Performance under normal daily variables: Temperature range, altitude tolerance, hematocrit handling, and strip stability can all affect results in real use.
- Consistency across batches: Procurement teams should ask about strip lot quality control, calibration approach, and manufacturing traceability.
For distributors, clinics, or healthcare programs, the most practical question is not “Is this meter smart?” but “Can this meter produce dependable readings across a large user base with varied skill levels?” That framing leads to better supplier comparison and lower operational risk.
Which connectivity features create real value instead of unnecessary complexity?
Connectivity is one of the biggest reasons smart glucometers stand out from conventional models, but not every connected feature improves outcomes. The best systems reduce friction and support review, escalation, and follow-up.
High-value connectivity features include:
- Automatic Bluetooth synchronization: Users should not need to manually upload data after every test.
- Companion mobile app with stable performance: The app should be easy to pair, easy to navigate, and reliable across common smartphone operating systems.
- Cloud backup and secure sharing: This helps support family monitoring, physician review, and chronic care programs.
- Exportable reports: PDF, CSV, or clinician-ready summary formats simplify follow-up appointments and internal reporting.
- Integration potential: For enterprise buyers, compatibility with remote patient monitoring platforms or care management systems is increasingly important.
Features that often sound appealing but deserve scrutiny include overly complex dashboards, limited-region app support, and proprietary ecosystems that make data migration difficult. If connectivity fails often or requires repeated setup, adoption drops quickly.
What makes a smart glucometer easier and safer for everyday operation?
Daily-use success depends heavily on ergonomics and workflow design. Even an accurate meter can become a poor fit if it is uncomfortable, confusing, or too time-consuming to use consistently.
Operationally important features include:
- Readable display: Large numbers, high contrast, and intuitive icons are especially important for elderly users or low-light conditions.
- Small blood sample requirement: This reduces discomfort and can improve compliance.
- Fast result delivery: Short wait times make repeated daily testing less disruptive.
- Minimal coding or no-coding design: This lowers error risk and simplifies training.
- Memory and event tagging: Pre-meal, post-meal, exercise, or medication markers make readings more useful for interpretation.
- Reminder functions: Built-in prompts help maintain regular testing routines.
- Hygiene and handling design: Easy-to-clean surfaces, durable strip ports, and straightforward lancet integration matter in both home and professional settings.
For quality and safety managers, human factors are not secondary concerns. Ease of use directly affects testing compliance, reading reliability, and support burden. Devices intended for broad deployment should be evaluated with real users, not only through technical documentation.
How do procurement teams evaluate total cost, supply risk, and long-term value?
For procurement personnel, financial approvers, and business evaluators, the true cost of a smart glucometer extends beyond the initial device price. In many cases, the recurring strip cost will determine long-term affordability and user retention.
Key commercial evaluation points include:
- Test strip pricing and availability: A low-cost meter paired with expensive or scarce strips may become a poor investment.
- Lancet and accessory ecosystem: Standardized, easy-to-source consumables reduce supply disruption.
- Warranty and after-sales support: Fast replacement processes matter for continuous monitoring routines.
- App maintenance and firmware support: A connected device loses value if software updates stop or compatibility breaks over time.
- Regional distribution reliability: Importers and channel partners should assess lead times, stock stability, and documentation readiness.
- Training and onboarding requirements: Lower training demand can reduce rollout cost in clinics, pharmacies, employer wellness programs, or remote care networks.
For B2B decision-makers, a useful selection model is to compare products on a blended scorecard: device cost, annual consumables cost, estimated user adherence impact, support overhead, and data integration value. This approach is more realistic than comparing hardware prices alone.
Which smart glucometer features matter most for different use scenarios?
The best smart glucometer for daily use depends on the operating context. Different readers should prioritize features differently:
- Individual daily users: Prioritize comfort, app simplicity, reminder functions, and affordable strips.
- Elderly users or caregiver-supported patients: Focus on large display, simple workflow, auto-sync, and remote sharing.
- Clinics and chronic care programs: Look for data export, multi-patient management potential, reliable connectivity, and support documentation.
- Distributors and resellers: Emphasize regulatory readiness, supply continuity, brand trust, and channel support materials.
- Enterprise health buyers: Prioritize integration capacity, device fleet manageability, data security, and total cost predictability.
In broader healthcare technology portfolios, smart glucometers are often evaluated alongside other connected devices such as digital blood pressure monitors and wearable ECG monitors. That makes interoperability, user adherence, and service support more important than isolated hardware specifications.
What red flags should buyers watch for before choosing a smart glucometer?
Several warning signs can help readers avoid poor product selection:
- Vague accuracy claims without standards or validation references
- Apps with frequent pairing issues or weak user reviews
- Limited strip availability in the target market
- Poor documentation for distributors or institutional buyers
- Overcomplicated user interface for a daily-use device
- No clear data privacy or sharing policy
- Weak post-sale technical support or unclear warranty terms
These issues can turn a promising product into an operational burden. For any buyer making a serious evaluation, a pilot test with representative users is often the fastest way to validate fit.
Final decision: what defines the best smart glucometer features for daily use?
The best smart glucometer features for daily use are the ones that make glucose monitoring more reliable, easier to sustain, and more useful in decision-making. In most cases, the right device will combine proven accuracy, easy testing, dependable connectivity, meaningful data reporting, and a stable consumables supply chain. For business buyers and healthcare stakeholders, long-term value also depends on support quality, software continuity, and integration readiness.
In short, smart features only matter when they improve real-world outcomes. A good glucometer should help users test consistently, help caregivers and clinicians see patterns clearly, and help buyers manage cost and risk with confidence. That is the standard worth using when comparing options in today’s connected healthcare technology market.
Get weekly intelligence in your inbox.
No noise. No sponsored content. Pure intelligence.



























