Which MRI Machine Parts Fail Most Often?
MRI downtime often starts with a few vulnerable mri machine components, from RF coils and gradient amplifiers to cooling and power modules. For hospitals, service teams, and procurement leaders comparing healthcare technology investments alongside portable ultrasound scanners, smart glucometers, digital blood pressure monitors, wearable ecg monitors, remote patient monitoring, and telemedicine carts, understanding the most failure-prone parts is essential for reducing risk, controlling maintenance costs, and improving equipment uptime.
In practice, MRI reliability is not determined by a single flagship subsystem. It depends on how electromagnetic, thermal, mechanical, and software-controlled parts perform together over thousands of scan hours. For operators, even a minor fault can trigger canceled appointments, patient rescheduling, and compliance reviews. For procurement and finance teams, the larger issue is total cost of ownership across a 7- to 12-year asset life.
This article examines which MRI machine parts fail most often, why they fail, how those failures affect throughput and service budgets, and what buyers should verify before purchasing service contracts, refurbished modules, or complete imaging systems. The goal is to support more informed maintenance planning, sourcing decisions, and risk control across healthcare technology operations.
The MRI Components That Fail Most Often
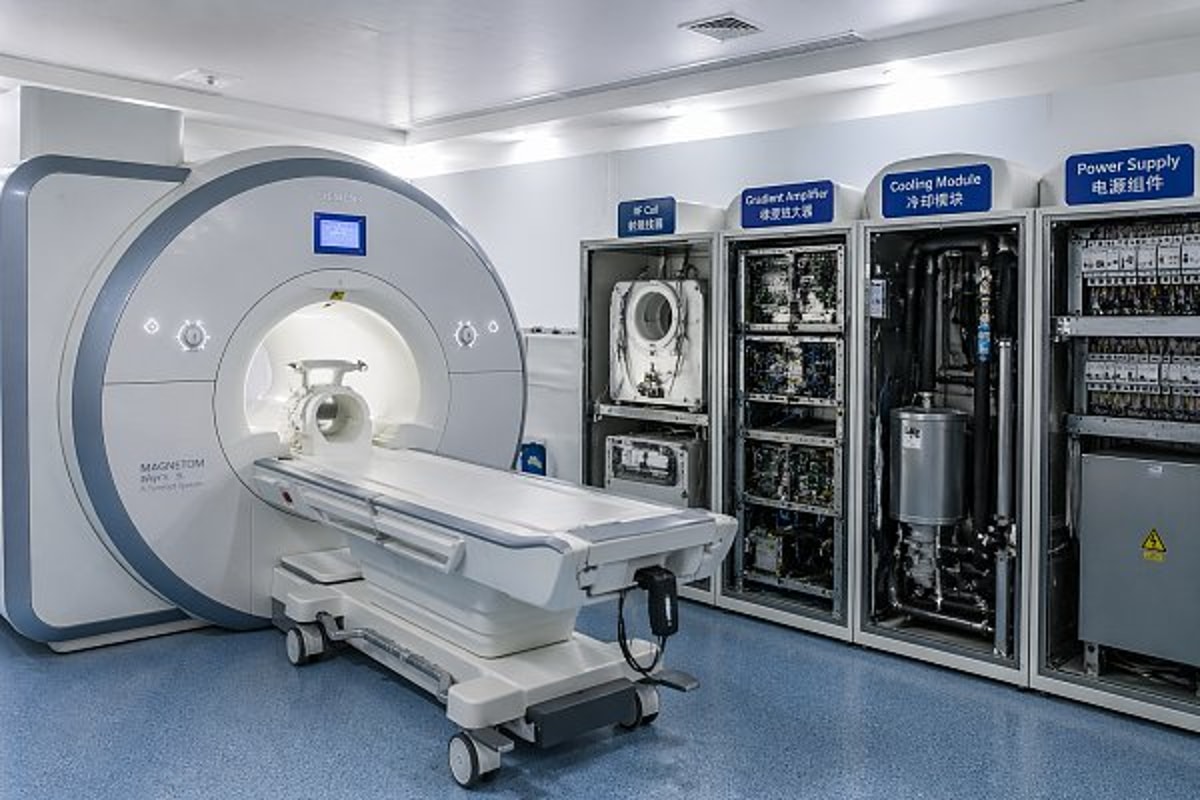
Although failure patterns vary by system age, field strength, utilization, and installation quality, several MRI machine parts repeatedly appear in service discussions: RF coils, gradient amplifiers, cooling assemblies, patient table motion systems, and power-related modules. In high-use imaging centers running 20 to 40 exams per day, wear accumulates much faster than in lower-volume departments.
RF coils are among the most frequently affected components because they are handled directly by staff, positioned around patients, and exposed to cable strain, connector wear, fluid ingress, and repeated cleaning cycles. A coil may still function partially while producing image artifacts, reduced signal-to-noise ratio, or failed channel detection, making early diagnosis essential.
Gradient amplifiers and associated electronics are another common pain point. These parts operate under significant thermal and electrical stress during rapid imaging sequences. Repeated high-duty cycles, unstable power quality, or insufficient cooling can shorten service life. When these parts degrade, the symptoms may include scan aborts, system trips, or inconsistent gradient performance.
Cooling systems also fail more often than many nontechnical stakeholders expect. MRI platforms depend on controlled operating temperatures for electronics cabinets, chillers, heat exchangers, and, in some setups, helium management support. Even a temperature drift of a few degrees can accelerate wear on sensitive boards, amplifiers, and power supplies.
Patient table assemblies, docking sensors, emergency stop circuits, and door interlock-related parts tend to fail through mechanical fatigue and repeated daily use. These failures may seem less critical than magnet or gradient faults, but they can still halt scans immediately because patient positioning and safety interlocks must operate within strict tolerances.
High-frequency failure areas at a glance
The table below summarizes common high-risk parts, typical failure drivers, and likely operational effects. Exact service intervals differ by OEM, site conditions, and exam mix, but the pattern is consistent across many installed systems.
For decision-makers, the key takeaway is that MRI failure risk is distributed across consumable-like accessories, electronics, and facility-dependent support systems. The most expensive part is not always the part most likely to fail. In many facilities, smaller assemblies cause the most frequent interruptions while larger subsystems create the highest single-event repair cost.
Why These Parts Fail: Stress, Environment, and Usage Patterns
MRI machine parts usually fail because of cumulative stress rather than sudden isolated defects. A system that operates 5 days per week with standard neuro and spine protocols faces a different wear profile from a center running 6 days per week with cardiac, diffusion, and high-duty advanced sequences. Usage intensity directly affects gradient loading, fan runtime, cable movement, and thermal cycling.
Environmental conditions are equally important. Equipment rooms should generally maintain stable temperature and humidity within site-recommended ranges, often around 20°C to 24°C with controlled moisture levels. If ambient heat climbs, dust filtration is poor, or airflow around cabinets is restricted, amplifier boards, power modules, and cooling components age faster than expected.
Human factors also matter. RF coils are vulnerable to drops, improper storage, tight cable wrapping, and rushed patient setup. Table components face repetitive loading, especially in sites with bariatric workflows or frequent patient transfers. Small process gaps repeated 15 to 30 times daily can produce large maintenance consequences within 12 to 24 months.
Power quality is another underestimated issue. Facilities without effective voltage conditioning or backup planning may expose MRI electronics to surges, brownouts, or abrupt shutdowns. Sensitive boards and supplies often tolerate minor fluctuation, but repeated instability increases intermittent failures that are difficult to diagnose and costly to trace.
Four operational stress categories
- Thermal stress: prolonged scan sessions, blocked airflow, fan degradation, or chiller inefficiency.
- Mechanical stress: cable bending, connector insertion cycles, table movement, vibration, and transport impact.
- Electrical stress: unstable mains power, overloaded circuits, sudden restarts, and aging capacitors.
- Process stress: inadequate cleaning practice, poor storage, delayed preventive maintenance, and limited operator training.
Aging profile by service life stage
During years 1 to 3, failures are more likely to stem from installation, early-use handling, or isolated parts issues. Between years 4 and 7, wear-driven problems become more visible in fans, connectors, motion systems, and cooling components. After year 8, boards, amplifiers, and hard-to-source modules may present both higher failure risk and longer replacement lead times.
For procurement teams comparing new, refurbished, or service-supported installed systems, these lifecycle stages should shape budgeting. A lower acquisition price may look attractive, but if a critical module has a 2- to 6-week sourcing lead time, lost scanning capacity can outweigh the initial savings.
How Failure-Prone Parts Affect Uptime, Safety, and Cost Control
Not every MRI failure has the same business impact. Some faults degrade image quality gradually, while others stop operations immediately. An RF coil issue may only affect selected studies, but a gradient amplifier or cooling shutdown can take the entire scanner offline. This difference matters for service prioritization, spare strategy, and financial approval processes.
Downtime cost is not limited to repair invoices. Hospitals also absorb schedule disruption, staff idle time, referral leakage, overtime for rescheduling, and reputational damage among clinicians. In facilities with 15 to 25 booked MRI slots per day, even one lost day can create a backlog that takes several days to recover, depending on staffing and patient acuity.
Safety and quality teams should also distinguish between nuisance faults and compliance-sensitive faults. Table locking issues, emergency stop irregularities, cooling alarms, and door interlock failures can all trigger additional review before the scanner is returned to service. In many organizations, that means coordination between engineering, radiology leadership, and risk management.
For capital planning, the practical question is not simply “Which part fails most?” but “Which part creates the highest operational penalty when it fails?” The answer often combines failure frequency, replacement lead time, labor hours, and impact on patient throughput.
Operational impact matrix
The following matrix helps procurement, service, and finance stakeholders rank common failures by business consequence rather than technical complexity alone.
This comparison shows why service strategy should combine critical spare planning with workflow contingency planning. A less expensive part may still deserve higher stocking priority if it fails frequently and blocks a large share of common exam protocols.
What finance and approval teams should ask
- What is the expected lead time for each high-risk part: 24 hours, 3 to 5 days, or 2 to 4 weeks?
- Does the service agreement include loaner coils, remote diagnostics, and after-hours response?
- How many unplanned outages occurred in the last 12 months, and which components caused them?
- Is the scanner environment audited for power quality, airflow, and preventive maintenance completion?
What Buyers Should Evaluate Before Sourcing Parts, Service, or Replacement Systems
For procurement professionals, the best response to frequent MRI machine part failures is not reactive buying. It is structured evaluation. Whether sourcing an RF coil, a refurbished amplifier, a multiyear service contract, or a replacement scanner, buyers should assess compatibility, traceability, installation support, and expected remaining service life.
A common mistake is focusing only on purchase price. In B2B healthcare technology environments, a part that arrives 20% cheaper but lacks testing documentation or has unclear service history can create higher downstream cost. Verification should include functional test records, packaging standards, warranty terms, return workflow, and the supplier’s response window for dead-on-arrival or intermittent faults.
Service agreements should also be segmented by risk. Sites with one scanner and no referral backup usually need faster response and stronger parts coverage than hospital networks with multiple imaging locations. A 4-hour remote response, next-business-day field service, and defined escalation process can be more valuable than broad but vague “full support” language.
When comparing MRI investments with other healthcare technology assets such as telemedicine carts or remote patient monitoring systems, MRI deserves a different procurement model. Its downtime cost is concentrated, installation-dependent, and operationally disruptive. That means engineering review, facilities input, clinical workflow mapping, and finance approval should all occur before contract signature.
Practical supplier evaluation checklist
The checklist below can help distributors, hospital buyers, and project managers qualify suppliers or service partners more consistently.
For enterprise buyers, the strongest sourcing approach combines technical validation with commercial discipline. A reliable supplier should be able to discuss lead times, installation dependencies, and likely failure modes in clear operational terms, not just provide a quotation.
Maintenance, Risk Reduction, and FAQ for Long-Term Uptime
Reducing failure frequency begins with preventive routines that match actual workload. High-volume MRI departments should review coil condition, cable integrity, airflow clearance, and alarm history weekly, while broader preventive maintenance tasks may follow monthly, quarterly, and annual schedules. The objective is to catch drift early, before a minor issue becomes a service-stopping fault.
Operator training is one of the lowest-cost ways to protect MRI machine parts. Staff should know how to store coils without sharp cable bends, inspect connectors visually, recognize abnormal noise or fan behavior, and escalate recurring warnings. Even a 30-minute refresher every 6 months can improve handling consistency in busy departments.
Facilities teams should also monitor room conditions, maintenance logs, and utility stability. Where scanners are mission-critical, a simple governance model with 3 owners—clinical operations, biomedical engineering, and facilities—often improves response speed and accountability. This is especially useful when MRI competes for budget with other digital health and diagnostic technologies.
Risk reduction actions that usually deliver value
- Track repeat faults by subsystem over rolling 90-day and 12-month periods.
- Keep critical accessories such as high-use coils or connectors under tighter inspection cycles.
- Audit cooling performance and filter cleanliness before summer load peaks or extended operating periods.
- Review whether your service contract aligns with current exam volume, not last year’s volume.
How often do RF coils fail compared with larger MRI components?
RF coils typically experience more frequent handling-related issues than large fixed subsystems because they are moved, cleaned, connected, and repositioned throughout the day. Their individual repair cost may be lower than amplifier or cooling failures, but the recurrence rate can be higher in sites with heavy patient turnover.
Which failure creates the most expensive downtime?
Gradient amplifier, power module, and cooling-related failures often create the most expensive downtime because they can disable the entire scanner. Total impact depends on parts availability, engineer access, and whether the site has backup imaging capacity. In many cases, the business loss of 2 to 3 outage days exceeds the hardware invoice itself.
Should buyers stock spare MRI parts on-site?
That decision depends on exam volume, service geography, and single-point failure risk. For isolated sites or high-throughput centers, selected spares such as commonly used coils, connectors, or certain cooling consumables may be justified. Expensive boards and amplifiers are usually better managed through defined supplier access and response commitments unless utilization is exceptionally high.
What is a reasonable review cycle for MRI maintenance strategy?
A practical cadence is quarterly review for outage trends and annual review for contract scope, environmental controls, and replacement planning. If the scanner is older than 8 years or utilization has increased by more than 15%, a midyear risk review is also advisable.
MRI uptime depends on identifying failure-prone parts early, linking technical risk to operational impact, and sourcing support with clear service terms. RF coils, gradient amplifiers, cooling modules, power supplies, and table-related assemblies deserve close attention because they combine frequent wear, workflow sensitivity, and meaningful cost consequences.
For hospitals, distributors, project leaders, and enterprise buyers, the most effective strategy is a combination of preventive maintenance, disciplined supplier qualification, and lifecycle-based budgeting. If you are evaluating MRI parts sourcing, service coverage, or broader healthcare technology investment priorities, TradeNexus Pro can help you compare solutions with stronger market context and procurement insight. Contact us to discuss your requirements, request a tailored sourcing framework, or explore more healthcare technology solutions.
Get weekly intelligence in your inbox.
No noise. No sponsored content. Pure intelligence.




























